Abstract
Background
The normative blood pressure values in preterm infants still not well defined during postnatal transition. We aimed to create normative blood pressure (BP) reference values in preterm infants <29 weeks gestational age recorded hourly during the postnatal transition.
Methods
We included only data from hemodynamically stable newborns. Only BP values measured by umbilical arterial catheter (UAC) were included. The regression model showed that only gestational age and postnatal age in hours determine the BP.
Results
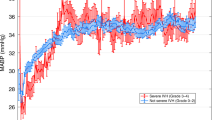
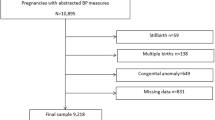
We included 206 out of 547 admitted preterm infants. The BP increases with increasing gestational ages and overtime during the postnatal transition. We constructed 5 BP centile values for each gestational group. BP histograms show that the BP most of the time fluctuated between the 5th and 75th centile values, particularity during day one of life.
Conclusions
The BP trend values gradually increase in stable preterm infants during the postnatal transition, and preterm infants who do not follow this trend might require hemodynamics assessment.
Impact
-
The normative blood pressure is increasing gradually during the first 3 days after birth and is different with gestational ages.
-
This is first normative blood pressure centile values in stable preterm infant and based on invasive blood pressure monitoring.
-
The data enable more accurate monitoring of hemodynamics in preterm infants during postnatal transition.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 14 print issues and online access
$259.00 per year
only $18.50 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Stebor, A. D. Basic principles of noninvasive blood pressure measurement in infants. Adv. Neonatal Care 5, 252–261 (2005).
James, G. D. & Gerber, L. M. Measuring arterial blood pressure in humans: auscultatory and automatic measurement techniques for human biological field studies. Am. J. Hum. Biol. 30, e23063 (2018).
Lurbe, E., Torro, I., Rodríguez, C., Alvarez, V. & Redón, J. Birth weight influences blood pressure values and variability in children and adolescents. Hypertension 38, 389–393 (2001).
Lang, S. M., Giuliano, J. S. Jr, Carroll, C. L., Rosenkrantz, T. S. & Eisenfeld, L. Neonatal/infant validation study of the CAS model 740 noninvasive blood pressure monitor with the Orion/MaxIQ NIBP module. Blood Press Monit. 19, 180–2 (2014).
Evans, N. & Iyer, P. Change in blood pressure after treatment of patent ductus arteriosus with indomethacin. Arch. Dis. Child 68, 584–587, http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=1029308&tool=pmcentrez&rendertype=abstract (1993).
Doyle, L. W., Faber, B., Callanan, C. & Morley, R. Blood pressure in late adolescence and very low birth weight. Pediatrics 111, 252–257 (2003).
Kent, A. L. & Chaudhari, T. Determinants of neonatal Blood pressure. Curr. Hypertens. Rep. 15, 426–432 (2013).
Weber, F., Koning, L. & Scoones, G. P. Defining hypotension in anesthetized infants by individual awake blood pressure values: a prospective observational study. Paediatr. Anaesth. 27, 377–384 (2017).
Modanlou, H., Yeh, S. Y., Siassi, B. & Hon, E. H. Direct monitoring of arterial blood pressure in depressed and normal newborn infants during the first hour of life. J. Pediatr. 85, 553–559 (1974).
Alderliesten, T. et al. Hypotension in preterm neonates: low blood pressure alone does not affect neurodevelopmental outcome. J. Pediatr. 164, 986–991 (2014).
Fisher, D. J., Heymann, M. A. & Rudolph, A. M. Regional myocardial blood flow and oxygen delivery in fetal, newborn, and adult sheep. Am. J. Physiol. 243, H729–H731 (1982).
Batton, B. et al. Evolving blood pressure dynamics for extremely preterm infants. J. Perinatol. 34, 301–305 (2014).
Cayabyab, R., McLean, C. W. & Seri, I. Definition of hypotension and assessment of hemodynamics in the preterm neonate. J. Perinatol. 29, S58–S62 (2009).
Shimokaze, T., Akaba, K. & Saito, E. Oscillometric and intra-arterial blood pressure in preterm and term infants: extent of discrepancy and factors associated with inaccuracy. Am. J. Perinatol. 32, 277–82 (2015).
Pereira, S. S. et al. Blood pressure intervention levels in preterm infants: pilot randomised trial. Arch. Dis. Child Fetal Neonatal Ed. 104, F298–F305 (2019).
Banerjee, J., Leung, T. S. & Aladangady, N. Cerebral blood flow and oximetry response to blood transfusion in relation to chronological age in preterm infants. Early Hum. Dev. 97, 1–8 (2016).
Fanaroff, J. M. & Fanaroff, A. A. Blood pressure disorders in the neonate: hypotension and hypertension. Semin. Fetal Neonatal Med. 11, 174–181 (2006).
Nelson, R. M. et al. Determination of accuracy in neonates for non-invasive blood pressure device using an improved algorithm. Blood Press Monit. 7, 123–129 (2002).
Batton, B. Neonatal blood pressure standards: what is “normal”? Clin. Perinatol. 47, 469–485 (2020).
Elsayed, Y. & Abdul Wahab, M. G. A new physiologic-based integrated algorithm in the management of neonatal hemodynamic instability. Eur. J. Pediatr. 181, 1277–1291 (2022).
Amer, R., Moddemann, D., Seshia, M., Ruben, A. & Anne, S. Neurodevelopmental outcomes of infants born at <29 weeks of gestation admitted to Canadian neonatal intensive care units based on location of birth. J. Pediatr. 196, 31–37.e1 (2018).
Eliason, S. Y., Whyte, H., Dow, K., Cronin, C. & Lee, S. Variations in transport outcomes of outborn infants among Canadian neonatal intensive care units. Am. J. Perinatol. 30, 377–382 (2013).
Binder-Heschl, C., Urlesberger, B., Schwaberger, B., Baik, N. & Pichler, G. Borderline-hypotension, how does it influence the cerebral tissue oxygenation? J. Paediatr. Child Health 51, 45 (2015).
Filippi, L. et al. Rescue treatment with terlipressin in different scenarios of refractory hypotension in newborns and infants. Pediatr. Crit. Care Med. 12, 237–241 (2011).
Meyer, S., Sander, J., Gräber, S., Gottschling, S. & Gortner, L. Agreement of invasive versus non-invasive blood pressure in preterm neonates is not dependent on birth weight or gestational age. J. Paediatr. Child Health 46, 249–254 (2010).
Rabe, H. et al. Antenatal and perinatal factors influencing neonatal blood pressure: a systematic review. J. Perinatol. 41, 2317–2329 (2021).
Funding
This study was supported by a grant from iNO Therapeutics, LLC, a subsidiary of Mallinckrodt Pharmaceuticals.
Author information
Authors and Affiliations
Contributions
Y.E. conceptualized the article, conducted the background literature search, and revised the manuscript and both authors agree to the formatting and contents. F.A. collected the blood pressure values.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This study was approved by the ethics board at the University of Manitoba.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Elsayed, Y., Ahmed, F. Blood pressure normative values in preterm infants during postnatal transition. Pediatr Res 95, 698–704 (2024). https://doi.org/10.1038/s41390-023-02788-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-023-02788-8