Abstract
Background
We reviewed the medical case report literature to determine the proportion of cases of idiopathic intracranial hypertension (IIH) that were either inappropriately labelled as IIH or prematurely given this diagnosis.
Methods
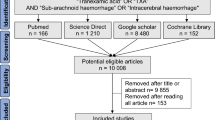
We searched OVID MEDLINE from 2012 to 2022 to identify case reports that diagnosed patients with IIH. Case reports were assessed for diagnostic accuracy using Friedman et al.‘s revised diagnostic criteria for primary pseudotumor cerebri syndrome. Our primary outcome was the crude prevalence of inappropriate or premature IIH diagnoses. Our secondary outcome was determining if inaccurate IIH diagnoses were associated with variables such as journal subscription model and impact factor, author affiliation, country of origin, and year of publication.
Results
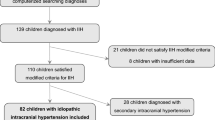
A total of 33/185 case reports (17.8%) either incorrectly labelled a patient as having IIH or did not perform all of the investigations necessary to make a diagnosis of IIH. Some of these studies (4.8%) were believed to still represent ‘probable’ IIH given the clinical presentation, whereas 13.0% of studies were determined to have mislabelled their patients as having IIH. The most common reason that case reports did not meet diagnostic criteria included: a lack of MRV in atypical patient cases (42.4%, n = 14), no papilledema in addition to a lack of characteristic neuroimaging features (33.3%, n = 11), intracranial hypertension being secondary to another documented cause (12.1%, n = 4), normal LP opening pressure in addition to other factors (12.1%,n = 4), no description of neuroimaging (6.1%, n = 2), and abnormal CSF composition (6.1%, n = 2). Case reports that used the term ‘IIH’ incorrectly had a significantly lower journal impact factor (2.0 vs. 2.6, p = 0.01).
Conclusions
There is a high prevalence of premature or inappropriate diagnoses of IIH in the peer-reviewed case report literature. Adherence to published diagnostic criteria is needed when publishing IIH case reports, and authors are expected to report all relevant data in their report to ensure that an accurate diagnosis is made.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The datasets generated during the current study are available from the corresponding author upon request.
References
Mollan SP, Aguiar M, Evison F, Frew E, Sinclair AJ. The expanding burden of idiopathic intracranial hypertension. Eye. 2019;33:478–85.
Giuseffi V, Wall M, Siegel PZ, Rojas PB. Symptoms and disease associations in idiopathic intracranial hypertension (pseudotumor cerebri): a case-control study. Neurology. 1991;41:239–44.
Friedman DI, Liu GT, Digre KB. Revised diagnostic criteria for the pseudotumor cerebri syndrome in adults and children. Neurology. 2013;81:1159–65.
Saindane AM, Bruce BB, Riggeal BD, Newman NJ, Biousse V. Association of MRI findings and visual outcome in idiopathic intraCranial hypertension. Am J Roentgenol. 2013;201:412–8.
Tao B, Vosoughi A, Margolin E, Micieli J. Inappropriate use of the term “Papilledema” in the medical literature: a systematic review of case reports across specialties. Ophthalmology. 2022;130:129–36.
Web of Science. Web of Science - Clarivate. Clarivate Analytics. 2019.
Mollan SP, Chong YJ, Grech O, Sinclair AJ, Wakerley BR. Current perspectives on idiopathic intracranial hypertension without papilloedema. Life. 2021;11:472.
Blokhin IO, Lentz SR. Mechanisms of thrombosis in obesity. Curr Opin Hematol. 2013;20:437–44.
Agarwal P, Kumar M, Arora V. Clinical profile of cerebral venous sinus thrombosis and the role of imaging in its diagnosis in patients with presumed idiopathic intracranial hypertension. Indian J Ophthalmol. 2010;58;153–5.
Barboza MA, Chiquete E, Arauz A, Merlos-Benitez M, Quiroz-Compeán A, Barinagarrementería F, et al. A practical score for prediction of outcome after cerebral venous thrombosis. Front Neurol. 2018;9:882.
Morris PP, Black DF, Port J, Campeau N. Transverse sinus stenosis is the most sensitive MR imaging correlate of idiopathic intracranial hypertension. Am J Neuroradiol. 2017;38:471–7.
Matalia J, Shirke S, Anaspure H, Ghalla P, Kekatpure M. Management of idiopathic intracranial hypertension in an infant with bilateral congenital cataract and associated comitant sensory esotropia. Indian J Ophthalmol. 2017;65:1053.
Talukder NT, Clorfeine AH, Black MK, Moody SB. Atypical idiopathic intracranial hypertension presenting as cyclic vomiting syndrome: a case report. J Med Case Rep. 2021;15:440.
Inger HE, Rogers DL, McGregor ML, Aylward SC, Reem RE. Diagnostic criteria in pediatric intracranial hypertension. J AAPOS. 2017;21, 492–95.e2
Neville L, Egan RA. Frequency and amplitude of elevation of cerebrospinal fluid resting pressure by the Valsalva maneuver. Can J Ophthalmol. 2005;40:775–7.
Schwartz KM, Luetmer PH, Hunt CH, Kotsenas AL, Diehn FE, Eckel LJ, et al. Position-related variability of CSF opening pressure measurements. Am J Neuroradiol. 2013;34:904–7.
Atas U, Aydin Ersoy M, Iltar U, Yucel OK, Turkoglu EB, Salim O. Papilledema and idiopathic intracranial hypertension due to the possible potentiation of ATRA by posaconazole in a case of acute promyelocytic leukemia. J Oncol Pharm Pract. 2022;28:1474–7.
Thaller M, Homer V, Hyder Y, Yiangou A, Liczkowski A, Fong A, et al. The idiopathic intracranial hypertension prospective cohort study: evaluation of prognostic factors and outcomes. J Neurol. 2023;270:851–63.
Huang-Link YM, Al-Hawasi A, Oberwahrenbrock T, Jin YP. OCT measurements of optic nerve head changes in idiopathic intracranial hypertension. Clin Neurol Neurosurg. 2015;130:122–7.
Pavlovic V, Weissgerber T, Stanisavljevic D, Pekmezovic T, Milicevic O, Lazovic JM, et al. How accurate are citations of frequently cited papers in biomedical literature? Clin Sci. 2021;135:671–81.
Carta A, Favilla S, Prato M, Bianchi-Marzoli S, Sadun AA, Mora P. Accuracy of Funduscopy to identify true Edema versus Pseudoedema of the optic disc. Investig Ophthalmol Vis Sci. 2012;53:1.
Author information
Authors and Affiliations
Contributions
AE and JM were responsible for designing the review protocol, conducting the search, screening eligible studies, and collecting data. AE was responsible for performing data analysis and generating charts and tables. All authors were responsible for interpreting the results, and writing and revising the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Eshtiaghi, A., Margolin, E. & Micieli, J.A. Inaccuracy of idiopathic intracranial hypertension diagnosis in case reports. Eye 37, 3243–3248 (2023). https://doi.org/10.1038/s41433-023-02499-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-023-02499-8