Abstract
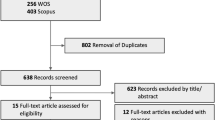
TNF-α is a multifunctional cytokine produced by macrophages and T cells. This proinflammatory substance is considered to play a crucial role in the inflammatory process associated with age-related macular degeneration (AMD). The current review aimed to describe evidence for an association between TNF-α and AMD reported in various studies. The MEDLINE, Embase, PubMed and Global Health databases were systematically searched to identify studies that investigated the role of TNF-α in AMD. A total of 24 studies were deemed eligible for the review. To better understand and integrate the evidence, the studies were categorised into four major groups in relation to the role of TNF-α in AMD: (1) those examining biological signalling pathways through which TNF-α exerts its effect; (2) investigating levels of TNF-α; (3) exploring the genetics underlying the role of TNF-α; and (4) assessing anti-TNF-α agents as potential treatments for AMD. TNF-α is thought to directly contribute to choroidal neovascularization (CNV) enhancement and has been shown to exert its effect by augmenting the inflammatory response through other signalling pathways. Additionally, different genes have been found to be associated with activities linked to TNF-α in AMD. Overall, measurement of systemic and local levels of TNF-α has not yielded consistent findings, with variable conclusions for the role of anti-TNF-α agents in remission of AMD symptoms. The role of TNF-α in neovascular AMD is not clear, and not all anti-TNF-α agents are safe. The potential of this cytokine in atrophic AMD has not been examined. Future studies should address these unresolved questions.
摘要
TNF-α是由巨噬细胞和T细胞产生的多功能细胞因子。其在与年龄相关性黄斑变性 (AMD) 的炎症过程中起重要作用。本综述旨在描述各种研究中报告的TNF-α和AMD相关联的证据。对MEDLINE、Embase、PubMed和全球健康数据库进行搜索, 确定有关TNF-α在AMD中的作用的研究。共有24项研究符合本综述条件。为更好地理解和整合证据, 根据TNF-α在AMD中的作用, 将文献分为四大类: (1) TNF-α发挥作用的细胞信号通路; (2) TNF-α的水平; (3) 探索TNF-α潜在的遗传学作用; (4) 评估抗TNF-α药物作为AMD的潜在治疗。TNF-α可直接导致脉络膜新生血管 (CNV), 并且通过其他信号通路增强炎症反应发挥其作用。此外, 发现不同基因与TNF-α在AMD的相关病理作用有关。总之, 对于TNF-α全身和局部水平还无一致结果, 对于抗TNF-α药物在缓解AMD症状的作用方面得出了多种结论。TNF-α抗新生血管的作用还不清楚, 并非所有抗TNF-α药物都是安全的。这种细胞因子在萎缩性AMD中的潜力尚未得到研究。未来的研究应解决这些尚未解决的问题。
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Wong WL, Su X, Li X, Cheung CM, Klein R, Cheng CY, et al. Global prevalence of age-related macular degeneration and disease burden projection for 2020 and 2040: a systematic review and meta-analysis. Lancet Glob Health. 2014;2:e106–16.
Kawasaki R, Yasuda M, Song SJ, Chen SJ, Jonas JB, Wang JJ, et al. The prevalence of age-related macular degeneration in Asians: a systematic review and meta-analysis. Ophthalmology. 2010;117:921–7.
Mitchell P, Smith W, Attebo K, Wang JJ. Prevalence of age-related maculopathy in Australia. The Blue Mountains Eye Study. Ophthalmology. 1995;102:1450–60.
Ferris FL 3rd, Wilkinson CP, Bird A, Chakravarthy U, Chew E, Csaky K, et al. Clinical classification of age-related macular degeneration. Ophthalmology. 2013;120:844–51.
Al-Zamil WM, Yassin SA. Recent developments in age-related macular degeneration: a review. Clin Inter Aging. 2017;12:1313–30.
Collier JAB, Collier J, Longmore M, Longmore JM, Amarakone K. Oxford Handbook of Clinical Specialties. (OUP Oxford, New York, NY, 2013).
Chernykh V, Shevchenko A, Konenkov V, Prokofiev V, Eremina A, Trunov A. TNF-α gene polymorphisms: association with age-related macular degeneration in Russian population. Int J Ophthalmol. 2019;12:25–9.
Wang H, Han X, Wittchen ES, Hartnett ME. TNF-α mediates choroidal neovascularization by upregulating VEGF expression in RPE through ROS-dependent β-catenin activation. Mol Vis. 2016;22:116–28.
Martin DF, Maguire MG, Fine SL, Ying GS, Jaffe GJ, Grunwald JE, et al. Ranibizumab and bevacizumab for treatment of neovascular age-related macular degeneration: two-year results. Ophthalmology. 2012;119:1388–98.
Johnson LV, Leitner WP, Staples MK, Anderson DH. Complement activation and inflammatory processes in Drusen formation and age related macular degeneration. Exp Eye Res. 2001;73:887–96.
Mullins RF, Dewald AD, Streb LM, Wang K, Kuehn MH, Stone EM. Elevated membrane attack complex in human choroid with high risk complement factor H genotypes. Exp Eye Res. 2011;93:565–7.
Sakurai E, Anand A, Ambati BK, Van Rooijen N, Ambati J. Macrophage depletion inhibits experimental choroidal neovascularization. Invest Ophthalmol Vis Sci. 2003;44:3578–85.
Hageman GS, Anderson DH, Johnson LV, Hancox LS, Taiber AJ, Hardisty LI, et al. A common haplotype in the complement regulatory gene factor H (HF1/CFH) predisposes individuals to age-related macular degeneration. Proc Natl Acad Sci USA. 2005;102:7227–32.
Fernández-Vega B, Fernández-Vega Á, Rangel CM, Nicieza J, Villota-Deleu E, Vega JA, et al. Blockade of tumor necrosis factor-alpha: a role for adalimumab in neovascular age-related macular degeneration refractory to anti-angiogenesis therapy? Case Rep. Ophthalmol. 2016;7:154–62.
Al-Gayyar MM, Elsherbiny NM. Contribution of TNF-α to the development of retinal neurodegenerative disorders. Eur Cytokine Netw. 2013;24:27–36.
Cordero-Coma M, Sobrin L. Anti–tumor necrosis factor-α therapy in uveitis. Surv Ophthalmol. 2015;60:575–89.
Yu Y, Reynolds R, Rosner B, Daly MJ, Seddon JM. Prospective assessment of genetic effects on progression to different stages of age-related macular degeneration using multistate Markov models. Invest Ophthalmol Vis Sci. 2012;53:1548–56.
Nagineni CN, Kommineni VK, William A, Detrick B, Hooks JJ. Regulation of VEGF expression in human retinal cells by cytokines: implications for the role of inflammation in age-related macular degeneration. J Cell Physiol. 2012;227:116–26.
Liu J, Tian Z, Li J, Zhao G. Associations of IL-8 gene polymorphisms and IL-8 levels with predisposition to age-related macular degeneration: a meta-analysis. Aging Clin Exp Res. 2020;32:2705.
Mimura T, Funatsu H, Noma H, Shimura M, Kamei Y, Yoshida M, et al. Aqueous humor levels of cytokines in patients with age-related macular degeneration. Ophthalmologica. 2019;241:81–89.
Jing L, Su L, Ring BZ. Ethnic background and genetic variation in the evaluation of cancer risk: a systematic review. PLoS One. 2014;9:e97522.
Theodossiadis PG, Markomichelakis NN, Sfikakis PP. Tumor necrosis factor antagonists: preliminary evidence for an emerging approach in the treatment of ocular inflammation. Retina. 2007;27:399–413.
MacEwan DJ. TNF ligands and receptors-a matter of life and death. Br J Pharm. 2002;135:855–75.
Idriss HT, Naismith JH. TNF alpha and the TNF receptor superfamily:structure-function relationship(s). Microsc Res Tech. 2000;50:184–95.
Khera TK, Dick AD, Nicholson LB. Mechanisms of TNFα regulation in uveitis: focus on RNA-binding proteins. Prog Retin Eye Res. 2010;29:610–21.
Sfikakis PP, Kollias G. Tumor necrosis factor biology in experimental and clinical arthritis. Curr Opin Rheumatol. 2003;15:380–6.
Oh H, Takagi H, Takagi C, Suzuma K, Otani A, Ishida K, et al. The potential angiogenic role of macrophages in the formation of choroidal neovascular membranes. Invest Ophthalmol Vis Sci. 1999;40:1891–8.
Bellezza I. Oxidative stress in age-related macular degeneration: Nrf2 as therapeutic target. Front Pharm. 2018;9:1280.
Thornalley PJ. The enzymatic defence against glycation in health, disease and therapeutics: a symposium to examine the concept. Biochem Soc Trans. 2003;31:1341–2.
Ishibashi T, Murata T, Hangai M, Nagai R, Horiuchi S, Lopez PF, et al. Advanced glycation end products in age-related macular degeneration. Arch Ophthalmol. 1998;116:1629–32.
Sharif U, Mahmud NM, Kay P, Yang YC, Harding SP, Grierson I, et al. Advanced glycation end products-related modulation of cathepsin L and NF-κB signalling effectors in retinal pigment epithelium lead to augmented response to TNFα. J Cell Mol Med. 2019;23:405–16.
Glenn JV, Mahaffy H, Wu K, Smith G, Nagai R, Simpson DA, et al. Advanced glycation end product (AGE) accumulation on Bruch’s membrane: links to age-related RPE dysfunction. Invest Ophthalmol Vis Sci. 2009;50:441–51.
Suk K, Kim SY, Kim H. Regulation of IL-18 production by IFN gamma and PGE2 in mouse microglial cells: involvement of NF-kB pathway in the regulatory processes. Immunol Lett. 2001;77:79–85.
YouTube. NF-κB signal pathway. 2019. https://www.youtube.com/watch?v=Ac1Q5yK6A50.
Im E, Kazlauskas A. The role of cathepsins in ocular physiology and pathology. Exp Eye Res. 2007;84:383–8.
Wang X, Shang QL, Ma JX, Liu SX, Wang CX, Ma C. Complement factor B knockdown by short hairpin RNA inhibits laser-induced choroidal neovascularization in rats. Int J Ophthalmol. 2020;13:382–9.
Bora NS, Kaliappan S, Jha P, Xu Q, Sohn JH, Dhaulakhandi DB, et al. Complement activation via alternative pathway is critical in the development of laser-induced choroidal neovascularization: role of factor B and factor H. J Immunol. 2006;177:1872–8.
Wang J, Ohno-Matsui K, Yoshida T, Shimada N, Ichinose S, Sato T, et al. Amyloid-beta up-regulates complement factor B in retinal pigment epithelial cells through cytokines released from recruited macrophages/microglia: another mechanism of complement activation in age-related macular degeneration. J Cell Physiol. 2009;220:119–28.
Huang Y, Krein PM, Muruve DA, Winston BW. Complement factor B gene regulation: synergistic effects of TNF-alpha and IFN-gamma in macrophages. J Immunol. 2002;169:2627–35.
Kawakami Y, Watanabe Y, Yamaguchi M, Sakaguchi H, Kono I, Ueki A. TNF-alpha stimulates the biosynthesis of complement C3 and factor B by human umbilical cord vein endothelial cells. Cancer Lett. 1997;116:21–26.
Chung EJ, Efstathiou NE, Konstantinou EK, Maidana DE, Miller JW, Young LH, et al. AICAR suppresses TNF-α-induced complement factor B in RPE cells. Sci Rep. 2017;7:17651.
Cha DM, Woo SJ, Kim HJ, Lee C, Park KH. Comparative analysis of aqueous humor cytokine levels between patients with exudative age-related macular degeneration and normal controls. Invest Ophthalmol Vis Sci. 2013;54:7038–44.
Liu F, Ding X, Yang Y, Li J, Tang M, Yuan M, et al. Aqueous humor cytokine profiling in patients with wet AMD. Mol Vis. 2016;22:352–61.
Cao S, Ko A, Partanen M, Pakzad-Vaezi K, Merkur AB, Albiani DA, et al. Relationship between systemic cytokines and complement factor H Y402H polymorphism in patients with dry age-related macular degeneration. Am J Ophthalmol. 2013;156:1176–83.
Zhu D, Yang DY, Guo YY, Zheng YF, Li JL, Wang B, et al. Intracameral interleukin 1β, 6, 8, 10, 12p, tumor necrosis factor α and vascular endothelial growth factor and axial length in patients with cataract. PLoS One. 2015;10:e0117777.
Minaker SA, Mason RH, Luna GL, Bapat P, Muni RH. Changes in aqueous and vitreous inflammatory cytokine levels in neovascular age-related macular degeneration: a systematic review and meta-analysis. Acta Ophthalmol. 2020;99:134–55.
Ioanna Z, Christian S, Christian G, Daniel B. Plasma levels of hypoxia-regulated factors in patients with age-related macular degeneration. Graefes Arch Clin Exp Ophthalmol. 2018;256:325–32.
Nassar K, Grisanti S, Elfar E, Lüke J, Lüke M, Grisanti S. Serum cytokines as biomarkers for age-related macular degeneration. Graefes Arch Clin Exp Ophthalmol. 2015;253:699–704.
Spindler J, Zandi S, Pfister IB, Gerhardt C, Garweg JG. Cytokine profiles in the aqueous humor and serum of patients with dry and treated wet age-related macular degeneration. PLoS One. 2018;13:e0203337.
Khan AH, Pierce CO, De Salvo G, Griffiths H, Nelson M, Cree AJ, et al. The effect of systemic levels of TNF-alpha and complement pathway activity on outcomes of VEGF inhibition in neovascular AMD. Eye (Lond). 2022;36:2192–9.
Rezar-Dreindl S, Sacu S, Eibenberger K, Pollreisz A, Bühl W, Georgopoulos M, et al. The intraocular cytokine profile and therapeutic response in persistent neovascular age-related macular degeneration. Invest Ophthalmol Vis Sci. 2016;57:4144–50.
Miao H, Tao Y, Li XX. Inflammatory cytokines in aqueous humor of patients with choroidal neovascularization. Mol Vis. 2012;18:574–80.
Faber C, Jehs T, Juel HB, Singh A, Falk MK, Sørensen TL, et al. Early and exudative age-related macular degeneration is associated with increased plasma levels of soluble TNF receptor II. Acta Ophthalmol. 2015;93:242–7.
Subhi Y, Nielsen MK, Molbech CR, Oishi A, Singh A, Nissen MH, et al. Plasma markers of chronic low-grade inflammation in polypoidal choroidal vasculopathy and neovascular age-related macular degeneration. Acta Ophthalmol. 2019;97:99–106.
Bonyadi MH, Bonyadi M, Ahmadieh H, Fotuhi N, Shoeibi N, Saadat S, et al. Tumor necrosis factor gene polymorphisms in advanced non-exudative age-related macular degeneration. J Ophthalmic Vis Res. 2015;10:155–9.
Wan L, Lin HJ, Tsai Y, Lee CC, Tsai CH, Tsai FJ, et al. Tumor necrosis factor-α gene polymorphisms in age-related macular degeneration. Retina. 2010;30:1595–600.
Xu J, Zhu D, He S, Spee C, Ryan SJ, Hinton DR. Transcriptional regulation of bone morphogenetic protein 4 by tumor necrosis factor and its relationship with age-related macular degeneration. FASEB J. 2011;25:2221–33.
Huang H, Liu Y, Wang L, Li W. Age-related macular degeneration phenotypes are associated with increased tumor necrosis-alpha and subretinal immune cells in aged Cxcr5 knockout mice. PLoS One. 2017;12:e0173716.
Olson JL, Courtney RJ, Mandava N. Intravitreal infliximab and choroidal neovascularization in an animal model. Arch Ophthalmol. 2007;125:1221–4.
Kirman I, Whelan RL, Nielsen OH. Infliximab: mechanism of action beyond TNF-alpha neutralization in inflammatory bowel disease. Eur J Gastroenterol Hepatol. 2004;16:639–41.
Theodossiadis PG, Liarakos VS, Sfikakis PP, Vergados IA, Theodossiadis GP. Intravitreal administration of the anti-tumor necrosis factor agent infliximab for neovascular age-related macular degeneration. Am J Ophthalmol. 2009;147:825–30.
Markomichelakis NN, Theodossiadis PG, Sfikakis PP. Regression of neovascular age-related macular degeneration following infliximab therapy. Am J Ophthalmol. 2005;139:537–40.
Van Hagen PM, Baarsma GS, Van Bilsen CE, Kuijpers RW, Van Laar JA, Van der Ent M, et al. A noncontrolled trial of anti-TNF-α chimeric monoclonal antibody (infliximab, Remicade(®)) in exudative age-related macular degeneration. Acta Ophthalmol. 2014;92:e691–2.
Wu L, Arevalo JF, Hernandez-Bogantes E, Regatieri CV, Roca JA, Farah ME. Intravitreal tumor necrosis factor-alpha inhibitors for neovascular age-related macular degeneration suboptimally responsive to antivascular endothelial growth factor agents: a pilot study from the Pan American Collaborative Retina Study Group. J Ocul Pharm Ther. 2013;29:366–71.
Arias L, Caminal JM, Badia MB, Rubio MJ, Catala J, Pujol O. Intravitreal infliximab in patients with macular degeneration who are nonresponders to antivascular endothelial growth factor therapy. Retina. 2010;30:1601–8.
Semeraro F, Romano MR, Danzi P, Angi M, Costagliola C. Intravitreal infliximab for choroidal neovascularization in patients refractory to conventional treatments. Int J Immunopathol Pharm. 2013;26:765–8.
Giganti M, Beer PM, Lemanski N, Hartman C, Schartman J, Falk N. Adverse events after intravitreal infliximab (Remicade). Retina. 2010;30:71–80.
Rosenfeld PJ, Goodman KW. When is off-label drug use in the patient’s best interest? Am J Ophthalmol. 2009;147:761–3.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The author declares no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix 1 Search terms and articles retrieved from databases
Appendix 1 Search terms and articles retrieved from databases
Database | Search terms | Results | |
|---|---|---|---|
1 | Embase 1974 to 2022 week 17 | 1# exp retina macula age-related degeneration/or exp age-related macular degeneration/or exp “neovascularization (pathology)” | 68090 |
2# exp age-related macular degeneration/or age-related maculopathy | 10376 | ||
3# exp macular degeneration | 16175 | ||
4# tumour necrosis factor alpha.mp. or exp tumour necrosis factor | 140867 | ||
5# (1 OR 2 OR 3) | 74434 | ||
6# 4 AND 5 | 703 | ||
2 | Ovid MEDLINE 1947 to 26 April 2022 | 1# exp retina macula age-related degeneration/or exp age-related macular degeneration/or exp “neovascularization (pathology)” | 23839 |
2# exp age-related macular degeneration/or age-related maculopathy | 23976 | ||
3# exp macular degeneration | 23839 | ||
4# tumour necrosis factor alpha.mp. or exp tumour necrosis factor | 129129 | ||
5# (1 OR 2 OR 3) | 23976 | ||
6# 4 AND 5 | 95 | ||
2 | Global Health 1973 to 2022 Week 17 | 1# exp retina macula age-related degeneration/or exp age-related macular degeneration/or exp “neovascularization (pathology)” | 0 |
2# exp age-related macular degeneration/or age-related maculopathy | 217 | ||
3# exp macular degeneration | 2071 | ||
4# tumour necrosis factor alpha.mp. or exp tumour necrosis factor | 6125 | ||
5# (1 OR 2 OR 3) | 2074 | ||
6# 4 AND 5 | 0 | ||
2# “macular degeneration”[MeSH Terms] OR agerelated macular degeneration [Text Word])” | 19467 | ||
3# “tumour necrosis factor-alpha”[MeSH Terms] | 123441 | ||
5# (“Age-related macular degeneration MeSH major topics” “Macular Degeneration”[Majr]) AND “Tumour Necrosis Factor-alpha”[Mesh] | 90 | ||
2 | PubMed 1973 to 2022 Week 17 | 1# Age-related macular degeneration MeSH major topics | 32609 |
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Papadopoulos, Z. The role of the cytokine TNF-α in choroidal neovascularization: a systematic review. Eye 38, 25–32 (2024). https://doi.org/10.1038/s41433-023-02634-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-023-02634-5