Abstract
Background/Objectives
Tessellated fundus can exist in normal healthy eyes. This study aims to evaluate the occurrence and influencing factors of tessellated fundus in preschool children aged 3–6 years.
Subjects/Methods
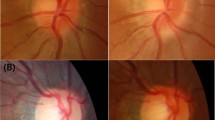
This kindergarten-based cross-sectional study included 1716 children with an age range of 3–6 years. All participants underwent a comprehensive eye examination and a questionnaire. According to the number of quadrants occupied by tessellated fundus around the optic disc in fundus photographs, it was divided into four grades.
Results
600 (35.0%) children had peripapillary tessellation. According to the spherical equivalent (SE), the subjects were divided into three groups: Hyperopia group (SE > + 0.75D, n = 1194);Pre-myopia group (−0.50D < SE ≤ + 0.75D, n = 455); Myopia group (SE ≤ −0.50D, n = 67). The proportion of peripapillary tessellated fundus was 33.0%, 38.0%, 50.7% respectively. According to the regression analysis, in the non-myopia group (Pre-myopia group and Hyperopia group), the occurrence of peripapillary tessellated fundus was associated with longer axial length (OR, 1.566; 95% CI: 1.229–1.996, p < 0.001) and larger corneal radius of curvature (OR, 1.837; 95% CI: 1.006–3.354, p = 0.048). However, in Pre-myopia group, the corneal radius of curvature was not associated with the occurrence of peripapillary tessellated fundus (p = 0.830). In Hyperopia group, the corneal radius of curvature was associated with the occurrence of peripapillary tessellated fundus (OR, 2.438; 95% CI: 1.160–5.122, p = 0.019).
Conclusions
The occurrence of peripapillary tessellated fundus is more than 30% in 3–6 year old preschool children. Tessellated fundus can also occur in non-myopic children, and is related to the length of axial length and large radius of corneal curvature.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
Data will be available upon reasonable request to the corresponding author.
References
Li SM, Kang MT, Li L, Wei SF, He X, Liu LR, et al. [Cohort study on the association between hyperopia reserve and myopia incidence in primary school students: the Anyang Childhood Eye Study]. Zhonghua Yan Ke Za Zhi. 2022;58:754–9.
Ohno-Matsui K, Kawasaki R, Jonas JB, Cheung CM, Saw SM, Verhoeven VJ, et al. International photographic classification and grading system for myopic maculopathy. Am J Ophthalmol. 2015;159:877–83.e7.
Fang Y, Yokoi T, Nagaoka N, Shinohara K, Onishi Y, Ishida T, et al. Progression of Myopic Maculopathy during 18-Year Follow-up. Ophthalmology. 2018;125:863–77.
Guo Y, Liu L, Zheng D, Duan J, Wang Y, Jonas JB, et al. Prevalence and Associations of Fundus Tessellation Among Junior Students From Greater Beijing. Invest Ophthalmol Vis Sci. 2019;60:4033–40.
Jonas JB, Grundler A. Optic disc morphology in “age-related atrophic glaucoma. Graefes Arch Clin Exp Ophthalmol. 1996;234:744–9.
Ohno-Matsui K, Lai TY, Lai CC, Cheung CM. Updates of pathologic myopia. Prog Retin Eye Res. 2016;52:156–87.
Yan YN, Wang YX, Yang Y, Xu L, Xu J, Wang Q, et al. Ten-Year Progression of Myopic Maculopathy: The Beijing Eye Study 2001-2011. Ophthalmology. 2018;125:1253–63.
Jagadeesh D, Philip K, Naduvilath TJ, Fedtke C, Jong M, Zou H, et al. Tessellated fundus appearance and its association with myopic refractive error. Clin Exp Optom. 2019;102:378–84.
Cheng T, Deng J, Xu X, Zhang B, Wang J, Xiong S, et al. Prevalence of fundus tessellation and its associated factors in Chinese children and adolescents with high myopia. Acta Ophthalmol. 2021;99:e1524–e33.
Lyu H, Chen Q, Hu G, Shi Y, Ye L, Yin Y, et al. Characteristics of Fundal Changes in Fundus Tessellation in Young Adults. Front Med (Lausanne). 2021;8:616249.
Gong W, Cheng T, Wang J, Zhang B, Chen J, Zhu J, et al. Role of corneal radius of curvature in early identification of fundus tessellation in children with low myopia. Br J Ophthalmol. 2023;107:1532–37.
Hosny M, Alio JL, Claramonte P, Attia WH, Perez-Santonja JJ. Relationship between anterior chamber depth, refractive state, corneal diameter, and axial length. J Refract Surg. 2000;16:336–40.
Park SH, Park KH, Kim JM, Choi CY. Relation between axial length and ocular parameters. Ophthalmologica. 2010;224:188–93.
Yoshihara N, Yamashita T, Ohno-Matsui K, Sakamoto T. Objective analyses of tessellated fundi and significant correlation between degree of tessellation and choroidal thickness in healthy eyes. PLoS One. 2014;9:e103586.
Yan YN, Wang YX, Xu L, Xu J, Wei WB, Jonas JB. Fundus Tessellation: Prevalence and Associated Factors: The Beijing Eye Study 2011. Ophthalmology. 2015;122:1873–80.
McBrien NA, Gentle A. Role of the sclera in the development and pathological complications of myopia. Prog Retin Eye Res. 2003;22:307–38.
Wang CY, Hsu NW, Yang YC, Chen YL, Shyong MP, Tsai DC. Premyopia at Preschool Age: Population-based Evidence of Prevalence and Risk Factors from a Serial Survey in Taiwan. Ophthalmology. 2022;129:880–9.
Wong YL, Ding Y, Sabanayagam C, Wong CW, Verkicharla P, Ohno-Matsui K, et al. Longitudinal Changes in Disc and Retinal Lesions Among Highly Myopic Adolescents in Singapore Over a 10-Year Period. Eye Contact Lens. 2018;44:286–91.
Tanaka N, Shinohara K, Yokoi T, Uramoto K, Takahashi H, Onishi Y, et al. Posterior staphylomas and scleral curvature in highly myopic children and adolescents investigated by ultra-widefield optical coherence tomography. PLoS One. 2019;14:e0218107.
Terasaki H, Yamashita T, Yoshihara N, Kii Y, Tanaka M, Nakao K, et al. Location of Tessellations in Ocular Fundus and Their Associations with Optic Disc Tilt, Optic Disc Area, and Axial Length in Young Healthy Eyes. PLoS One. 2016;11:e0156842.
Yamashita T, Terasaki H, Tanaka M, Nakao K, Sakamoto T. Relationship between peripapillary choroidal thickness and degree of tessellation in young healthy eyes. Graefes Arch Clin Exp Ophthalmol. 2020;258:1779–85.
Wang X, Zheng Y, Kong X, Zhu L, Sun X. The Characteristics of Peripapillary Retinal Perfusion by Optical Coherence Tomography Angiography in Tessellated Fundus Eyes. PLoS One. 2016;11:e0159911.
Morgan IG, French AN, Ashby RS, Guo X, Ding X, He M, et al. The epidemics of myopia: Aetiology and prevention. Prog Retin Eye Res. 2018;62:134–49.
Morgan IG, He M, Rose KA. EPIDEMIC OF PATHOLOGIC MYOPIA: What Can Laboratory Studies and Epidemiology Tell Us? Retina. 2017;37:989–97.
Acknowledgements
The authors thank Professor Yaxing Wang for critical discussions and revision of the manuscript.
Funding
The Beijing Hyperopia Reserve Research was supported by the “Capital Clinical Diagnosis and Treatment Technology Research and Translational Medicine Application” of Beijing Municipal Science and Technology Commission (2020–2024, project number Z201100005520034).
Author information
Authors and Affiliations
Contributions
XM wrote the manuscript. YJ and YF supervised the study and edited the manuscript. XM, JP, WC, RZ, DW, YY, CP, SB and HX helped to collect data. Statistical analysis support was provided by ZZ. MQ provided support in figure processing. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mi, X., Fang, Y., Pu, J. et al. Tessellated fundus occurs earlier than myopia in children aged 3–6 years. Eye (2024). https://doi.org/10.1038/s41433-024-03036-x
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41433-024-03036-x