Abstract
Purpose
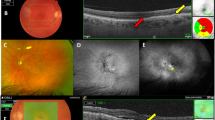
To describe the prevalence of subretinal transient hyporeflectivity (STHR) in exudative neovascular age-related macular degeneration (nAMD) and its response to a loading phase of aflibercept.
Methods
Optical coherence tomography (OCT) scans of treatment-naïve nAMD patients captured at baseline and after a loading phase of aflibercept were graded for presence of STHR, defined as a small, well-defined, round, subretinal, hyporeflective area, delimited between the ellipsoid zone (EZ) and the retinal pigmented epithelium/Bruch membrane complex. OCT parameters recorded were macular neovascularisation (MNV) subtypes, location of retinal fluids (subretinal fluid, SRF and intraretinal fluid, IRF), central retinal and choroidal thickness. Response was defined as absence of IRF and SRF. Factors associated with completely resolved STHR versus persistent STHR post-loading phase were compared.
Results
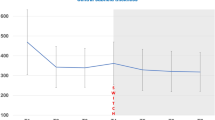
2039 eyes of 1901 patients were analysed. STHR was observed in 79 eyes of 78 patients, with an estimated prevalence of 3.87% (95% CI 3.08–4.81%). STHR were seen in 44 type 1 MNV (56%), 27 with type 2 (34%), and 8 with type 3 (10%). At baseline, a total of 303 STHR were present, ranging between 1–22 per eye. The total number of STHR reduced significantly after the loading phase to 173 (p = 0.002). Complete disappearance of STHR was seen in 44 eyes (56%) and persistent STHR in the rest (44%).
Conclusions
STHR may represent a marker of low-grade exudation in nAMD eyes with good response to a loading phase of aflibercept. However, its potential role as an independent nAMD activity biomarker is limited as most resolve after the loading phase.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The dataset generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Schmidt-Erfurth U, Klimscha S, Waldstein SM, Bogunović H. A view of the current and future role of optical coherence tomography in the management of age-related macular degeneration. Eye. 2017;31:26–44. https://doi.org/10.1038/eye.2016.227.
Hanson RLW, Airody A, Sivaprasad S, Gale RP. Optical coherence tomography imaging biomarkers associated with neovascular age-related macular degeneration: a systematic review. Eye. 2022. https://doi.org/10.1038/s41433-022-02360-4.
Spaide RF, Jaffe GJ, Sarraf D, Freund KB, Sadda SR, Staurenghi G, et al. Consensus Nomenclature for Reporting Neovascular Age-Related Macular Degeneration Data: Consensus on Neovascular Age-Related Macular Degeneration Nomenclature Study Group. Ophthalmology. 2020;127:616–36. https://doi.org/10.1016/j.ophtha.2019.11.004.
Singh SR, Lupidi M, Mishra SB, Paez-Escamilla M, Querques G, Chhablani J. Unique optical coherence tomographic features in age-related macular degeneration. Surv Ophthalmol. 2020;65:451–7. https://doi.org/10.1016/j.survophthal.2020.01.001.
Querques G, Coscas F, Forte R, Massamba N, Sterkers M, Souied EH. Cystoid Macular Degeneration in Exudative Age-Related Macular Degeneration. Am J Ophthalmol. 2011;152:100–107.e2. https://doi.org/10.1016/j.ajo.2011.01.027.
Fernández-Avellaneda P, Freund KB, Wang RK, et al. Multimodal Imaging Features and Clinical Relevance of Subretinal Lipid Globules. Am J Ophthalmol. 2021;222:112–25. https://doi.org/10.1016/j.ajo.2020.09.003.
Sacconi R, Mullins RF, Lutty GA, Borrelli E, Bandello F, Querques G. Subretinal pseudocyst: A novel optical coherence tomography finding in age-related macular degeneration. Eur J Ophthalmol. 2019;30:NP24–NP26. https://doi.org/10.1177/1120672119846437.
Hayashi-Mercado R, Pérez-Montaño C, Reyes-Sánchez J, Ramírez-Estudillo A. Findings of uncertain significance by optical coherence tomography (OCT) as prognostic factors in neovascular age-related macular degeneration (nAMD) treated with ranibizumab. Int J Retina Vitreous. 2022;8:29 https://doi.org/10.1186/s40942-022-00379-z.
Astroz P, Miere A, Amoroso F, Semoun O, Khorrami A, Srour M, et al. Subretinal transient hyporeflectivity in age-related macular degeneration: a spectral domain optical coherence tomography study. Retina. 2022;42:653–60. https://doi.org/10.1097/IAE.0000000000003377.
Schmidt-Erfurth U, Chong V, Loewenstein A, Larsen M, Souied E, Schlingemann R, et al. Guidelines for the management of neovascular age-related macular degeneration by the European Society of Retina Specialists (EURETINA). Br J Ophthalmol. 2014;98:1144–67. https://doi.org/10.1136/bjophthalmol-2014-305702.
Montesel A, Hagag AM, Chandra S, Muhammed RP, Thottarath S, Chandak S, et al. Quantitative response of macular neovascularisation to loading phase of aflibercept in neovascular age-related macular degeneration. Eye. 2023. https://doi.org/10.1038/s41433-023-02574-0.
Lumbroso B, Rispoli M, Savastano MC. Longitudinal Optical Coherence Tomography-Angiography Study of Type 2 Naive Choroidal Neovascularization Early Response After Treatment. Retina. 2015;35:2242–51. https://doi.org/10.1097/IAE.0000000000000879.
Miere A, Butori P, Cohen SY, Semoun O, Capuano V, Jung C, et al. Vascular Remodeling of Choroidal Neovascularization after Anti-Vascular Endothelial Growth Factor Therapy Visualized on Optical Coherence Tomography Angiography. Retina. 2019;39:548–57. https://doi.org/10.1097/IAE.0000000000001964.
Spaide RF. Optical Coherence Tomography Angiography Signs of Vascular Abnormalization With Antiangiogenic Therapy for Choroidal Neovascularization. Am J Ophthalmol. 2015;160:6–16. https://doi.org/10.1016/j.ajo.2015.04.012.
Zweifel SA, Engelbert M, Laud K, Margolis R, Spaide RF, Freund KB. Outer retinal tubulation: a novel optical coherence tomography finding. Arch Ophthalmol. 2009;127:1596–602. https://doi.org/10.1001/archophthalmol.2009.326.
Acknowledgements
The research was funded by Boehringer Ingelheim and supported by the NIHR Biomedical Research Centre at Moorfields Eye Hospital NHS Foundation Trust, UCL Institute of Ophthalmology and the NIHR Moorfields Clinical Research Facility. The views expressed are those of the author(s) and not necessarily those of the NHS, the NIHR or the Department of Health and Social Care.
Funding
Boehringer Ingelheim, Binger Str. 173, 55216, Ingelheim am, Rhein, Germany.
Author information
Authors and Affiliations
Contributions
AM and SS designed the study, analysed data, and drafted the manuscript. AM, RPM, DK, SC, ST, and SC collected the data. AM, VC, BJLB, GM, IP, MM, AK, JT, AG, FG, RG, AG, TCNY and SS reviewed the paper and contributed to the final version of the manuscript. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
None related to the paper. AM, RPM, SC, DK, and ST have no financial disclosures. ShC is a member of the Editorial board. SS received consultancy fees from Bayer, Allergan, Novartis Pharma AG, Roche, Boehringer Ingelheim, Optos, Apellis, Oxurion, Oculis and Heidelberg Engineering and is a member of the Eye editorial board. VC is an employee of Janssen R&D and previously of Boehringer Ingelheim. AG is an employee of Boehringer Ingelheim. TCNY is an employee of Boehringer Ingelheim. BB is in the advisory board and received international conference attendance sponsored by Novartis and Bayer. GM has conducted consultancy-advisory boards for Novartis, Bayer and Allergan, received educational travel grants from Novartis, Bayer, Allergan. IP has received lecture fees from Allergan, Bayer, Heidelberg and Novartis, consultancy fees from Allergan, Alimera, Bayer and Novartis and travel fees from Allergan, Bayer and Novartis. FG has received honorarium for consultancy-advisory boards from Alimera, Allergan, Bayer, Novartis, Oxford BioElectronics, Roche; educational travel grants from Allergan, Bayer, Novartis and is a member of the Eye editorial board. MM has received lecture and advisory board honoraria from Bayer and Novartis and an educational travel grant from Bayer. RG has conducted consultancy-advisory boards for Novartis, Bayer and Allergan, Alimera, Santen, received educational travel grants from Novartis, Bayer, Allergan, Heidelberg Engineering. JT is a consultant for Bayer and Novartis, received grant support from Bayer, Novartis and Heidelberg Engineering, and is involved in research for Allergan, Roche, Bayer, Novartis and Boehringer-Ingelheim. AK received travel support from Novartis, Bayer, and Allergan, and speaker fees from Allergan and Bayer.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Montesel, A., Pakeer Muhammed, R., Chandak, S. et al. Subretinal transient hyporeflectivity in neovascular age-related macular degeneration and its response to a loading phase of aflibercept: PRECISE report 4. Eye (2024). https://doi.org/10.1038/s41433-024-03087-0
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41433-024-03087-0