Abstract
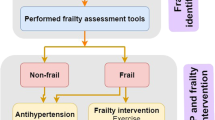
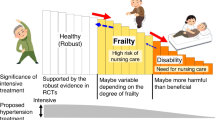
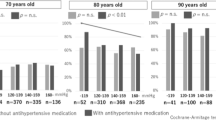
In older adults, functional decline, such as frailty and the need for nursing care, has a significant impact on quality of daily life (QOL) and life expectancy, and this is also true for older patients with hypertension. It has been shown that hypertensive patients with frailty or those in need of nursing care might be disadvantaged by conventional hypertension treatment according to the guidelines, while it is also known that inappropriate antihypertensive treatment may cause functional impairment. Therefore, in the management of older hypertensive patients, it is important to understand a patient’s condition using functional assessments, such as a comprehensive geriatric assessment (CGA) or frailty assessments, and it is strongly recommended to determine the antihypertensive target and select the antihypertensive treatment according to the degree of functional impairment or frailty.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56:M146–56.
Satake S, Shimada H, Yamada M, Kim H, Yoshida H, Gondo Y, et al. Prevalence of frailty among community-dwellers and outpatients in Japan as defined by the Japanese version of the Cardiovascular Health Study criteria. Geriatr Gerontol Int. 2017;17:2629–34.
Mitnitski AB, Mogilner AJ, Rockwood K. Accumulation of deficits as a proxy measure of aging. ScientificWorldJournal 2001;1:323–36.
Warwick J, Falaschetti E, Rockwood K, Mitnitski A, Thijs L, Beckett N, et al. No evidence that frailty modifies the positive impact of antihypertensive treatment in very elderly people: an investigation of the impact of frailty upon treatment effect in the HYpertension in the Very Elderly Trial (HYVET) study, a double-blind, placebo-controlled study of antihypertensives in people with hypertension aged 80 and over. BMC Med. 2015;13:78.
Williamson JD, Supiano MA, Applegate WB, Berlowitz DR, Campbell RC, Chertow GM, et al. Intensive vs standard blood pressure control and cardiovascular disease outcomes in adults aged >/=75 Years: a randomized clinical trial. JAMA. 2016;315:2673–82.
Pajewski NM, Williamson JD, Applegate WB, Berlowitz DR, Bolin LP, Chertow GM, et al. Characterizing frailty status in the systolic blood pressure intervention trial. J Gerontol A Biol Sci Med Sci. 2016;71:649–55.
Rockwood K, Andrew M, Mitnitski A. A comparison of two approaches to measuring frailty in elderly people. J Gerontol A Biol Sci Med Sci. 2007;62:738–43.
Benetos A, Labat C, Rossignol P, Fay R, Rolland Y, Valbusa F, et al. Treatment with multiple blood pressure medications, achieved blood pressure, and mortality in older nursing home residents: the PARTAGE Study. JAMA Intern Med. 2015;175:989–95.
Stessman J, Bursztyn M, Gershinsky Y, Hammerman-Rozenberg A, Jacobs JM. Hypertension and Its treatment at age 90 years: is there an association with 5-year mortality? J Am Med Dir Assoc. 2017;18:e13–e19. 277
Delgado J, Bowman K, Ble A, Masoli J, Han Y, Henley W, et al. Blood pressure trajectories in the 20 years before death. JAMA Intern Med. 2018;178:93–99.
Kabayama M, Kamide K, Gondo Y, Masui Y, Nakagawa T, Ogawa M, et al. The association of blood pressure with physical frailty and cognitive function in community-dwelling septuagenarians, octogenarians, and nonagenarians: the SONIC study. Hypertens Res. 2020;43:1421–9.
Todd OM, Wilkinson C, Hale M, Wong NL, Hall M, Sheppard JP, et al. Is the association between blood pressure and mortality in older adults different with frailty? A systematic review and meta-analysis. Age Ageing. 2019;48:627–35.
Tabara Y, Kohara K, Ochi M, Okada Y, Ohara M, Nagai T, et al. Association of office-based frailty score with hypertensive end organ damage in the J-SHIPP cross-sectional study. Int J Cardiol. 2016;216:25–31.
Wu C, Smit E, Peralta CA, Sarathy H, Odden MC. Functional status modifies the association of blood pressure with death in elders: health and retirement study. J Am Geriatr Soc. 2017;65:1482–9.
Hozawa A, Okamura T, Murakami Y, Kadowaki T, Okuda N, Takashima N, et al. High blood pressure in middle age is associated with a future decline in activities of daily living. NIPPON DATA80. J Hum Hypertens. 2009;23:546–52.
Canavan M, Smyth A, Bosch J, Jensen M, McGrath ER, Mulkerrin EC, et al. Does lowering blood pressure with antihypertensive therapy preserve independence in activities of daily living? A systematic review. Am J Hypertens. 2015;28:273–9.
Whelton PK, Carey RM, Aronow WS, Casey DE Jr., Collins KJ, Dennison Himmelfarb C, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Hypertension. 2018;71:1269–324.
Williams B, Mancia G, Spiering W, Agabiti Rosei E, Azizi M, Burnier M, et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension: The Task Force for the management of arterial hypertension of the European Society of Cardiology and the European Society of Hypertension: the Task Force for the management of arterial hypertension of the European Society of Cardiology and the European Society of Hypertension. J Hypertens. 2018;36:1953–2041.
Benetos A, Petrovic M, Strandberg T. Hypertension management in older and frail older patients. Circ Res. 2019;124:1045–60.
Umemura S, Arima H, Arima S, Asayama K, Dohi Y, Hirooka Y, et al. The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2019). Hypertens Res. 2019;42:1235–481.
Bromfield SG, Ngameni CA, Colantonio LD, Bowling CB, Shimbo D, Reynolds K, et al. Blood pressure, antihypertensive polypharmacy, frailty, and risk for serious fall injuries among older treated adults with hypertension. Hypertension. 2017;70:259–66.
Mol A, Slangen LRN, Trappenburg MC, Reijnierse EM, van Wezel RJA, Meskers CGM, et al. Blood pressure drop rate after standing up is associated with frailty and number of falls in geriatric outpatients. J Am Heart Assoc. 2020;9:e014688.
Butt DA, Mamdani M, Austin PC, Tu K, Gomes T, Glazier RH. The risk of hip fracture after initiating antihypertensive drugs in the elderly. Arch Intern Med. 2012;172:1739–44.
Liu P, Li Y, Zhang Y, Mesbah SE, Ji T, Ma L. Frailty and hypertension in older adults: current understanding and future perspectives. Hypertens Res. 2020;43:1352–60.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sugimoto, K., Yamamoto, K. Hypertension, the decline of activities of daily living (ADL) and frailty. Hypertens Res 45, 629–634 (2022). https://doi.org/10.1038/s41440-021-00846-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-021-00846-4
Keywords
This article is cited by
-
Long COVID and hypertension-related disorders: a report from the Japanese Society of Hypertension Project Team on COVID-19
Hypertension Research (2023)
-
The relationship between changes in exercise habits and psychosomatic activities in older hypertensive patients during the COVID-19 pandemic
Hypertension Research (2023)
-
Current issues in frailty and hypertension management
Hypertension Research (2023)