Abstract
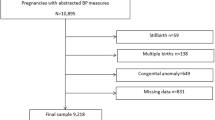
In the near future, hypertensive disorders of pregnancy (HDP) have been diagnosed by home blood pressure monitoring (HBPM) instead of clinic BP monitoring. A multicenter study of HBPM was performed in pregnant Japanese women in the non-high risk group for HDP. Participants were women (n = 218), uncomplicated pregnancy who self-measured and recorded their HBP daily. Twelve women developed HDP. HBP was appropriate (100 mmHg in systole and 63 mmHg in diastole), bottoming out at 17 to 21 weeks of gestation. It increased after 24 weeks of gestation and returned to non-pregnant levels by 4 weeks of postpartum. The upper limit of normal HBP was defined as the mean value +3 SD for systolic and mean +2 SD for diastolic with reference to the criteria for non-pregnant women. Using the polynomial equation, the hypertensive cut-off of systolic HBP was 125 mmHg at 15 weeks and 132 mmHg at 30 weeks of gestation, while it for diastolic HBP was 79 mmHg at 15 weeks and 81 mmHg at 30 weeks of gestation. Systolic HBP in women who developed HDP was higher after 24 weeks of gestation, and diastolic HBP was higher during most of the pregnancy compared to normal pregnancy. When the variability of individual HBP in women developed HDP compared to normal pregnant women was examined using the coefficient of variation (CV), the CV was lower in HDP before the onset of HDP. HBPM can be used not only for HDP determination, but also for early detection of HDP.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
O’Brien E, Asmar R, Beilin L, Imai Y, Mallion J, Mancia G, et al. on behalf of the European Society of Hypertension Working Group on Blood Pressure Monitoring. European Society of Hypertension recommendations for conventional, ambulatory and home blood pressure measurement. J Hypertens. 2003;21:821–48.
Bobrie G, Chatellier G, Genes N, Clerson P, Vaur L, Vaisse B, et al. Cardiovascular prognosis of ‘masked hypertension’ detected by blood pressure self-measurement in elderly treated hypertensive patients. JAMA. 2004;291:1342–9.
Parati G, Stergiou G, O’Brien E, Asmar R, Beilin L, Bilo G, et al. European Society of Hypertension guidelines for blood pressure monitoring at home: a summary report of the Second International Consensus Conference on Home Blood Pressure Monitoring. J Hypertens. 2008;26:1505–26.
Liyanage-Don N, Fung D, Phillips E, Kronish IM. Implementing Home Blood Pressure Monitoring into Clinical Practice. Curr Hypertens Rep. 2019;21:14.
The Japanese Society of Hypertension. Guidelines Subcommittees of the Japanese Society of Hypertension. Guidelines for the Management of Hypertension 2014. The Japanese Society of Hypertension, Life Science Publishing Co, Ltd. 2014.
Watanabe K, Matsubara K, Nakamoto O, Ushijima J, Ohkuchi A, Koide K, et al. Outline of the new definition and classification of “Hypertensive Disorders of Pregnancy (HDP)”; a revised JSSHP statement of 2005. Hypertens Res Pregnancy. 2018;6:33–37.
Glossary of Obstetrics and Gynecology, 4th edition, ed. Japan Society of Obstetrics and Gynecology, 2018, p255-6.
Best practice guide 2021 for care and treatment of hypertension in pregnancy. ed. Japan society for the study of hypertension in pregnancy, Medical View. 2021. p52-4.
Inoue M, Tsuchihashi T, Hasuo Y, Ogawa M, Tominaga M, Arakawa K, et al. Salt Intake, Home Blood Pressure, and Perinatal Outcome in Pregnant Women. Circ J. 2016;80:2165–72.
Metoki H, Ohkubo T, Obara T, Akutsu K, Yamamoto M, Ishikuro M, et al. Daily Serial Hemodynamic Data During Pregnancy and Seasonal Variation: The BOSHI Study. Clin Exp Hypertension. 2012;34:290–6.
Mikami Y, Takai Y, Era S, Ono Y, Saitoh M, Baba K, et al. Provisional criteria for the diagnosis of hypertension in pregnancy using home blood pressure measurements. Hypertens Res. 2017;40:679–84.
Hibbard J, Shroff S, Cunningham F. Cardiovascular alterations in normal and preeclamptic pregnancy.: Elsevier-Academic Press, San Diego, CA; 2015.
Umemura S, Arima H, Arima S, Asayama K, Dohi Y, Hirooka Y, et al. The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2019). Hypertens Res. 2019;42:1235–481.
Ohkuchi A, Hirashima C, Arai R, Takahashi K, Suzuki H, Ogoyama M, et al. Temporary hypertension and white coat hypertension in the first trimester as risk factors for preeclampsia. Hypertens Res. 2019;42:2002–12.
Rothwell PM, Howard SC, Dolan E, O’Brien E, Dobson JE, Dahlof B, et al. Prognostic significance of visit-to-visit variability, maximum systolic blood pressure, and episodic hypertension. Lancet. 2010;375:895–905.
Hata Y, Kimura Y, Muratani H, Fukiyama K, Kawano Y, Ashida T, et al. Office blood pressure variability as a predictor of brain infarction in elderly hypertensive patients. Hypertens Res. 2000;23:553–60.
Eguchi K, Hoshide S, Schwartz JE, Shimada K, Kario K. Visit-to-visit and ambulatory blood pressure variability as predictors of incident cardiovascular events in patients with hypertension. Am J Hypertens. 2012;25:962–8.
Stolarz-Skrzypek K, Thijs L, Richart T, Li Y, Hansen TW, Boggia J, et al. Blood pressure variability in relation to outcome in the International Database of Ambulatory blood pressure in relation to Cardiovascular Outcome. Hypertens Res. 2010;33:757–66.
Kario K, Pickering TG, Umeda Y, Hoshide S, Hoshide Y, Morinari M, et al. Morning surge in blood pressure as a predictor of silent and clinical cerebrovascular disease in elderly hypertensives: a prospective study. Circulation. 2003;107:1401–6.
Mancia G, Bombelli M, Facchetti R, Madotto F, Corrao G, Trevano FQ, et al. Long-term prognostic value of blood pressure variability in the general population: results of the Pressioni Arteriose Monitorate Loro Associazioni Study. Hypertension. 2007;49:1265–70.
Hansen TW, Thijs L, Li Y, Boggia J, Kikuya M, Björklund-Bodegård K, et al. International Database on Ambulatory Blood Pressure in Relation to Cardiovascular Outcomes Investigators. Prognostic value of reading-to-reading blood pressure variability over 24 hours in 8938 subjects from 11 populations. Hypertension. 2010;55:1049–57.
Johansson JK, Niiranen TJ, Puukka PJ, Jula AM. Prognostic value of the variability in home-measured blood pressure and heart rate: the Finn-Home Study. Hypertension. 2012;59:212–8.
Kikuya M, Ohkubo T, Metoki H, Asayama K, Hara A, Obara T, et al. Day-by-day variability of blood pressure and heart rate at home as a novel predictor of prognosis: the Ohasama study. Hypertension. 2008;52:1045–50.
Asayama K, Ohkubo T, Kikuya M, Obara T, Metoki H, Inoue R, et al. Prediction of stroke by home “morning” versus “evening” blood pressure values: the Ohasama study. Hypertension. 2006;48:737–43.
Kato T, Kikuya M, Ohkubo T, Satoh M, Hara A, Obara T, et al. Factors associated with day-by-day variability of self-measured blood pressure at home: the Ohasama study. Am J Hypertens. 2010;23:980–6.
Mena L, Pintos S, Queipo NV, Aizpurua JA, Maestre G, Sulbaran T. A reliable index for the prognostic significance of blood pressure variability. J Hypertens. 2005;23:505–11.
Rothwell PM, Howard SC, Dolan E, O’Brien E, Dobson JE, Dahlof B, et al. Effects of beta blockers and calcium-channel blockers on within-individual variability in blood pressure and risk of stroke. Lancet Neurol. 2010;9:469–80.
PaolaA A, Lanfranch, Virend KS. Arterial baroreflex function and cardiovascular variability: interactions and implications. Am J Physiol Regul Integr Comp Physiol. 2002;283:R815–R826.
McLaughlin MK, Conrad KP. Nitric oxide biosynthesis during pregnancy: Implications freduction or circulatory changes. Clin Exp Pharm Physiol. 1994;22:164–71.
Sladek SM, Magness RR, Conrad KP. Nitric oxide and pregnancy. Am J Physiol Regul Integr Comp Physiol. 1997;272:R441–R463.
Brooks VL, Dampney RA, Heesch CM. Pregnancy and the endocrine regulation of the baroreceptor reflex. Am J Physiol Regul Integr Comp Physiol. 2010;299:R439–R451.
Heesch CM, Foley CM. CNS effects of ovarian hormones and metabolites on neural control of circulation. Ann N. Y Acad Sci. 2001;940:348–60.
Fu Q, Levine BD. Autonomic circulatory control during pregnancy in humans. Semin Reprod Med. 2009;27:330–7.
Rang S, Wolf H, Montfrans GA, Karemaker JM. Non-invasive assessment of autonomic cardiovascular control in normal human pregnancy and pregnancy- associated hypertensive disorders: a review. J Hypertens. 2002;20:2111–9.
McLaughlin MK, Conrad KP. Nitric oxide biosynthesis during pregnancy: implications for circulatory changes. Clin Exp Pharm Physiol. 1995;22:164–71.
Weiner CP, Thompson LP. Nitric oxide and pregnancy. Semin Perinatol. 1997;21:367–80.
Liu JL, Murakami H, Zucker IH. Effects of NO on baroreflex control of heart rate and renal nerve activity in conscious rabbits. Am J Physiol Regul Integr Comp Physiol. 1996;270:R1361–R1370.
Matsumura K, Abe I, Tsuchihashi T, Fujishima M. Central nitric oxide attenuates the baroreceptor reflex in conscious rabbits. Am J Physiol Regul Integr Comp Physiol. 1998;274:R1142–R1149.
Poston L, McCarthy AL, Ritter JM. Control of vascular resistance in the maternal and fetoplacental arterial beds. Pharmacol Therapeutics. 1995;65:215–39.
Suzuki Y, Kajikuri J, Suzumori K, Itoh T. Mechanisms underlying the reduced endothelium-dependent relaxation in human omental resistance artery in pre-eclampsia. J Physiol. 2000;527:163–74.
Yousif D, Bellos I, Penzlin AI, Hijazi MM, Illigens BM, Pinter A, et al. Autonomic dysfunction in preeclampsia: A systematic Review. Front Neurol. www.frontiersin.org.
Weber TM, Lackner HK, Roessler A, Papousek I, Kolovetsiou-Kreiner V, Lucovnik M, et al. Heart rate variability and baroreceptor reflex sensitivity in early- versus late-onset preeclampsia. PLoS ONE. 2017;12:e0186521.
Faber R, Baumert M, Stepan H, Wessel N, Voss A, Walther T. Baroreflex sensitivity, heart rate, and blood pressure variability in hypertensive pregnancy disorders. J Hum Hypertens. 2004;18:707–12.
Niiranen TJ, Asayama K, Thijs L, Johansson JK, Ohkubo T, Kikuya M, et al. Outcome-driven thresholds for home blood pressure measurement: international database of home blood pressure in relation to cardiovascular outcome. Hypertension. 2013;61:27–34.
Acknowledgements
The authors would like to thank the following collaborators: Gen Ishikawa, Masahiro Ohashi, Mitsumasa Shimazu, Takuya Saitoh, Chiharu Fukue, Ai Iwasaki, Kenji Yamaguchi, Koji Kanda, Keisuke Fukui, and Hiroki Suzuki.
Funding
This work was supported by Intramural Research Fund (28-4-2) for Cardiovascular Disease of the National Cerebral and Cardiovascular Center and by the 2015 JSSHP Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Suzuki, Y., Matsubara, K., Watanabe, K. et al. A multicenter prospective study of home blood pressure measurement (HBPM) during pregnancy in Japanese women. Hypertens Res 45, 1563–1574 (2022). https://doi.org/10.1038/s41440-022-00992-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-022-00992-3
Keywords
This article is cited by
-
2023 update and perspectives
Hypertension Research (2023)
-
The next stage of hypertension management in Asia
Hypertension Research (2022)