Abstract
Purpose To compare the optic disc topography of patients with ocular Behçet's disease (BD) with age-matched controls, using Heidelberg retina tomograph (HRT).
Methods This study included 32 patients (51 eyes) with ocular BD (active and/or inactive), 38 patients (74 eyes) with nonocular BD, and 62 normal subjects (62 eyes). All patients and control group underwent complete ophthalmologic evaluation. Intraocular pressure was less than 22 mmHg in patients and in the control group. The optic nerve heads of all subjects were imaged with the HRT (software 2.01a-M). The following stereometric parameters were calculated for each patient: disc area, cup area, cup/disc area ratio, rim area, height variation contour, cup volume, rim volume, mean cup depth, cup shape measure, mean RNFL thickness, and RNFL cross-sectional area. Differences among the groups were evaluated by Kruskal–Wallis variance analysis. When the Kruskal–Wallis test revealed a significant difference between groups, multiple comparison tests were used to find out which groups differed from which others.
Results The mean disc area was significantly smaller (P<0.05) in patients with ocular and nonocular BD. The mean cup area, mean cup depth, and mean cup volume were significantly smaller (P<0.05) in patients with ocular BD. No significant differences were found between the groups in terms of the other stereometric parameters (P>0.05).
Conclusion A small disc and cup may be an additional risk factor for retinal vaso-occlusion in ocular Behçet's disease.
Similar content being viewed by others
Introduction
Behçet's disease (BD) affects many organs, and ocular involvement is frequently termed ocular BD. The disorders are an immune complex disease, with occlusive vasculitis. The classical finding in ocular BD is iridocyclitis with hypopyon, which is present in 19–31% of the cases.1 The fundus changes include optic nerve hyperaemia, macular oedema, retinal oedema, vascular sheathing, retinal vein occlusion, retinal exudates, retinal haemorrhages, retinal and optic disc atrophy, and vitreous haemorrhage.2 HRT is used to make quantitative measurements of the optic nerve head and nerve fibre layer. Topography images have a reproducibility of the height measurements of approximately 10–20 μm. In this study, we aimed to compare the quantitative topographical optic disc analysis by confocal scanning laser ophthalmoscopy in ocular, nonocular BD and healthy adults.
Method
In this study, we investigated 70 patients with BD who were followed up at the Uveitis Service at Ankara University Medical Faculty, Department of Ophthalmology. All patients fulfilled the international criteria for BD.3 The patients were divided into two groups: 32 patients with ocular BD and 38 patients with nonocular BD. Criteria for inclusion in patients were a reliable optic disc image, refraction less than 6 dioptre ametropia, intraocular pressure less than 22 mmHg, no history of ocular hypertension and glaucoma, and no evidence of glaucomatous changes in the optic disc. The control group for this study consisted of 62 normal subjects. Criteria for inclusion in normal subjects were refraction less than 6 dioptre ametropia, intraocular pressure less than 22 mmHg, no evidence of glaucomatous changes in optic disc, no previous ocular surgery, no history of systemic disease, and primary open angle glaucoma in first-degree relatives. The data were collected from both eyes of 62 normal individuals, but only one eye, was chosen randomly. The patients and control subjects were all Turkish.
Three images were obtained for each eye, and the mean of the three topographic images was calculated by HRT (Heidelberg Engineering GmbH, Heidelberg, Germany, software version 2.01a-M). After a contour line along the inner scleral ring of the optic disc was drawn, the images were analysed using the standard reference plan. The contour line was drawn manually by the same person (OT). The standard reference plan is defined parallel to the peripapillary retinal surface, and is located 50 μm posterior to the retinal surface at the papillo-macular bundle. The field of each image was 15 × 15°. The following stereometric parameters were calculated for each patient: disc area, cup area, cup/disc area ratio, rim area, height variation contour, cup volume, rim volume, mean cup depth, cup shape measure, mean RNFL thickness, and RNFL cross-sectional area. HRT is a confocal imaging device that produces a three-dimensional image by aligning 32 consecutive, two-dimensional images of 256 × 256 pixels. The acquisition time for 32 image series was 1.6 s. The depth of each topographic image series ranges from 0.5 to 4 mm in 0.5 mm increments.
Differences among groups were evaluated by Kruskal–Wallis variance analysis. When the Kruskal–Wallis test revealed a significant difference between groups, the multiple comparison tests was used to find out which groups differ from which others. A P-value of <0.05 was accepted as statistically significant.
Results
The study groups included 32 patients (51 eyes=group 1) with ocular BD (active and/or inactive), 38 patients (74 eyes=group 2) with nonocular BD, and 62 normal subjects (62 eyes=group 3). (group 1: 13 males (40.62%) and 19 females (59.37%) with a mean age of 31±7.87, age range 17–47, group 2: 15 males (39.47%) and 23 females (60.52%) with a mean age of 35.78±9.19, age range 17–55; group 3: 26 (41.93%) males and 36 (58.06%) females with a mean age of 35.5±10.16, age range 16–50). There was no stastistically significant difference between the ages of the patients and the controls (P>0.05). The duration of disease ranged from 1 to 19 years in group 1, and from 1 to 18 years in group 2. In group 1, 26 eyes (50.98%) had anterior uveitis (six of these eyes had retinal vasculitis) and 25 eyes (49.01%) had clinical evidence of previous ocular disease. In group 1, one eye had experienced central retinal vein occlusion (CRVO). Table 1 documents the characteristics of subjects.
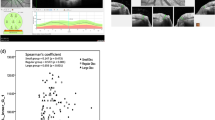
The mean disc area was significantly smaller (P<0.05) in patients with ocular and nonocular BD. The mean cup area, mean cup depth, and mean cup volume were significantly smaller (P<0.05) in patients with ocular BD (Figure 1). No significant differences were found between the groups in terms of the other stereometric parameters (P>0.05). Table 2 documents the mean values of the stereometric parameters.
Discussion
BD is a chronic, relapsing, occlusive vasculitis. Vascular sheathing, arteriolar attenuation, venous dilatation and tortuosity, and branch and central retinal vein occlusion are common posterior pole findings. Optic nerve involvements include recurrent papillitis, optic nerve vasculitis, papilloedema,4,5 optic neuropathy,6,7 neuropapillitis,8 and a ischaemic optic neuropathy.9 In the acute phase, the optic nerve vessels are affected by the angiitic process, and the nerve tissue has inflammatory cells. Progressive optic atrophy may occur as a result of microvasculitis of arterioles feeding the optic nerve.1 In all, 76–90% of the cases have bilateral ocular involvement, and the second eye is generally affected within 1 year of disease onset in the first eye.1
HRT is a confocal laser scanning ophthalmoscope designed especially for imaging and three-dimensional topography measurements at the fundus. The confocal laser scanning microscope uses a diode laser with a wavelength of 670 nm as the light source. The object under examination is scanned by the laser beam sequentially point by point. The confocal optical technique has a high optical resolution not only perpendicular but also parallel to the optical axis. Although glaucoma is a typical example for the clinical application of HRT, the clinical use of this instrument is much broader. It can be used in all cases where topographic changes at the posterior segment must be quantified.10
In our study, the mean disc area was significantly smaller in patients with ocular (2.087±0.46 mm2) and nonocular (2.126±0.41 mm2) BD, and the mean cup area, mean cup depth, and mean cup volume were significantly smaller in patients with ocular BD (0.303±0.27 mm2, 0.148±0.22 mm, and 0.065±0.12 mm3, respectively). A small physiologic cup is the consequence of a relatively small scleral canal and a small opening in Bruch's membrane, or an abundance of neural tissue, or both.11 In several studies, smaller cup/disc ratios were detected in the fellow eyes of patients with nonarteritic ischaemic optic neuropathy, and Mansour showed the horizontal diameter and disc area to be significantly smaller in the fellow eyes of patients than in controls.12,13,14,15
In BD, severe vasculitis leads to thrombosis of vessels and branch or central retinal vein occlusion may develop. Recently, Abu-el Asrar et al16 reported a case who had anterior ischaemic neuropathy associated with CRVO, and they suggested that compression of the central retinal vein by the swollen optic nerve may be a predisposing factor in the development of CRVO. Although one study reported that optic disc size and cup/disc ratio were not responsible for the development of retinal vein occlusion,17 we think that an anatomically small and crowded optic nerve head may be an additional risk factor for retinal vascular complications in ocular BD.
In conclusion, HRT may be a useful test to detect in patients with ocular BD who had an increased risk of ischaemic optic neuropathy and retinal vein occlusion.
References
Faris BM, Foster CS . Behçet's disease. In: Albert DM, Jacobiec FA, (eds) Principles and Practice of Ophthalmology: Clinical Practice, No. 2, W.B. Saunders Company: Philadelphia, 1994, pp 1018–1027.
Cassoux N, Fardeau C, Lehoang P . Ocular manifestation of Behcet's disease. Ann Med Interne (Paris) 1999; 150(7): 529–534.
Evaluation of diagnostic (classification) criteria in Behcet's disease—towards internationally agreed criteria. By the international study group for Behcet's disase. Br J Rheumatol 1992; 31: 299–308.
Teh LS, O’Connor GM, O’Sullivan MM, Pandit JC, Beck L, Williams BD . Reccurrent papilloedema and early onset optic atrophy in Behcet's syndrome. Ann Rheum Dis 1990; 49(6): 410–411.
Pamir MN, Kansu T, Erbengi A, Zileli T . Papilloedema in Behcet's syndrome. Arch Neurol 1981; 38(10): 643–645.
Salvi F, Mascalchi Malatesta R, Oliveri I, Molinotti C, Capaccioli L, Testoni S et al. Optic neuropathy in Behcet's disease. Report of two cases. Ital J Neurol Sci 1999; 20(3): 183–186.
Kansu T, Kirkali P, Kansu E, Zileli T . Optic neuropathy in Behcet's disease. J Clin Neuroophthalmol 1989; 9(4): 277–280.
Gallinaro C, Robinet-Combes A, Sale Y, Richard P, Saraux A, Colin J . Neuropapillitis in Behcet's disease. A case. J Fr Ophthalmol 1995; 18(2): 147–150.
Coticelli L, Apponi-Battini G, Federico A, Cotrufo R, Annuziata P, DiIOrio G . Behcet's disease:an unusual case with bilateral obliterating retinal panarteritis and ishemic optic atrophy. Ophthalmologica 1980; 180(6): 328–332.
Quantitative Three-dimensional Imaging of the Posterior Segment with the Heidelberg Retina Tomograph. HR7 user manual. Heidelberg Engineering GmbH, Heidelberg, Germany, 1999; 1–16.
Burde RM . Optic disc risk factors for nonarteritic anterior ischaemic optic neuropathy. Am J Ophthalmol 1993; 116(16): 759–764.
Doro S, Lessell S . Cup-disc ratio and ischaemic optic neuropathy. Arch Ophthalmol 1985; 103: 1143–1144.
Beck RW, Savino PJ, Repka MX, Schatz NJ, Sergott RC . Optic disc structure in anterior ischaemic optic neuropathy. Ophthalmology 1984; 91: 1334–1337.
Beck RW, Servais GE, Hayreh SS . Anterior ischaemic optic neuropathy: cup-to-disc ratio and its role in pathogenesis. Ophthalmology 1987; 94: 1503–1508.
Mansour A, Shoch D, Logani S . Optic disc size in ischaemic optic neuropathy. Am J Ophthalmol 1988; 106: 587–589.
Abu-el Asrar AM, Rashael SA, AbdelGader AG . Anterior ischaemic optic neuropathy associated with central retinal vein occlusion. Eye 2000; 14(part 4): 560–562.
Mansour AM, Walsh JB, Henkind P . Optic disc size in central retinal vein occlusion. Ophthalmology 1990; 97(2): 165–166.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was presented as a poster in the XXIX International Congress of Ophthalmology, Sydney 21–25 April 2002
Rights and permissions
About this article
Cite this article
Tekeli, O., Özdemir, Ö. Heidelberg retina tomograph in ocular Behçet's disease. Eye 18, 143–146 (2004). https://doi.org/10.1038/sj.eye.6700556
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.eye.6700556
Keywords
This article is cited by
-
Visual aspects of behçet’s disease
Current Treatment Options in Neurology (2006)
-
Visual aspects of BehÇet’s disease
Current Neurology and Neuroscience Reports (2005)