Abstract
Background Mersilene mesh (polyester fibre) is commonly used in ptosis surgery for frontalis suspension as it is readily available and cheap. Management of extrusion can be challenging. We report three cases of extrusion where extremely thick mesh or extremely thin tissue may have contributed to the extrusion.
Methods Retrospective case note study of three adult patients who developed chronic mesh extrusion.
Results Extrusion and chronic infection occured 5–12 months after surgery. Despite systemic antibiotics, all three patients required surgical excision of mesh from the eyelid up to the brow, which was curative.
Conclusion These cases illustrate the need for a systematic approach and the need in some cases to excise the mesh to prevent recurrent infection.
Similar content being viewed by others
Main
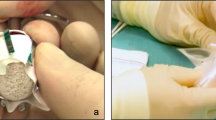
Mersilene® mesh (polyester fibre) is a commonly used nonautogenous material for frontalis suspension surgery in patients with poor levator function ptosis. A fine strip of mesh 3–8 mm wide is inserted as a Fox pentagon using a Wright's fascial needle via two stab incisions in the eyelid skin crease and three above the brow.1 The ends of the mesh are secured by a suture or knot, which must be well buried in the forehead.2,3,4,5,6,7,8,9 The complication rate from extrusion, granuloma, and/or infection ranges from 0 to 35%.2,3,4,5,6,7,8,9 We report three cases (Figure 1) referred to an oculoplastic service for management of chronic extrusion and infection of the Mersilene® mesh, where the mesh was excessively bulky and/or the soft tissue thin.
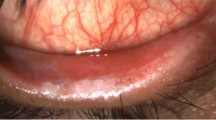
(a) Case 1: Wet infected Mersilene® mesh right upper eyelid. Note the incidental small basal cell carcinoma at medial canthus, subsequently excised. (b) Case 2: Dry extruding Mersilene® mesh on forehead and wet infected mesh in the left upper eyelid. (c) Case 3: Granuloma left upper eyelid from chronic extruding infected mesh.
Case reports
Case 1
A 70-year-old woman had a Mersilene® mesh frontalis suspension for right external ophthalmoplegia and ptosis. At 5 months after surgery, the mesh was extruding on the forehead. On exploration, it was found to be infected, therefore was removed under systemic antibiotic cover. The patient had secondary Mersilene® mesh frontalis suspension surgery a few months later. At 6 months after the second frontalis suspension, a protruding fibre on the forehead was noted and trimmed, and a course of systemic antibiotics prescribed. A month later, the mesh was visibly extruding from the eyelid and there was a chronic discharging sinus (Figure 1a). The patient was referred to the oculoplastic service.
Under systemic antibiotic cover, at least 4 cm of infected Mersilene® mesh was excised from between the eyelid and forehead—it had been tracking up from the eyelid towards the forehead (Figure 2). Postoperatively, the eyelid healed well with no recurrent infection or extrusion. The ptosis gradually recurred and the patient has since had an autogenous fascia lata frontalis suspension. There has been uneventful follow-up for over 29 months.
Case 2
An 83-year-old man with bilateral longstanding poor levator function ptosis was referred for management of extruding Mersilene® mesh, 5 months after bilateral frontalis suspension surgery. Dry white Mersilene® mesh fibres were seen extruding on the forehead bilaterally and wet smelly infected mesh in the left upper lid skin crease associated with very little redness or inflammation (Figure 1b).
Systemic antibiotics were commenced and an extensive length of infected mesh was excised from the upper eyelid towards the forehead. Since the forehead mesh had been exposed (even though dry), this was also excised as it was no longer regarded as sterile and could not justifiably be reburied. It was noted that the width of the excised mesh was in excess of 7 mm.2,4 Postoperatively, there was a slight asymmetry of the eyelid height, which was acceptable to the patient and further frontalis suspension surgery has not been required. The patient has been followed up for 27 months without further complications.
Case 3
A 46-year-old man with bilateral myotonic ptosis had bilateral Mersilene® mesh frontalis suspension. After 1 year, he developed a granuloma with a chronic intermittent discharging sinus from the left upper eyelid. The wound failed to heal; therefore, 3 months later, it was explored and pus drained, but the mesh apparently not excised.
He subsequently developed a discharging sinus on the left brow and in the left upper eyelid. Wide elliptical excision of both lesions was performed, without mesh excision. Histopathologic analysis of the excised tissue confirmed the lack of Mersilene® mesh fibres in the specimens.
After 2 months, the patient again had a discharging sinus from his left upper eyelid and a granuloma (Figure 1c). He was referred to the oculoplastic service for management of the chronic Mersilene® mesh extrusion and infection. The eyelid was explored and the granuloma with at least 2 cm of mesh was excised. There was a mild recurrent ptosis with a faint skin crease, which required skin crease revision. There has been an uneventful follow-up for 31 months.
Comment
These three cases illustrate late Mersilene® mesh complications 5–12 months after surgery. Initial management of these complications in two of the three cases was not curative, because the apparently superficial forehead extrusion masked a more extensive problem. On close examination, all three cases had chronic infected mesh extruding through the site of the eyelid stab incisions. A visible forehead problem concealed a more severe upper eyelid skin crease infection, indicating tracking of chronic infection between the eyelid towards the brow. Systemic antibiotics and granuloma excision with removal of the immediately underlying mesh is not always adequate, as shown by these cases, and more extensive dissection and excision are often required. Exploration through a skin crease incision and maximal excision of the infected mesh between the skin crease and forehead was required in all three cases. Although it may not be possible to remove the entire mesh length, it is possible to remove a long length. This is achieved by dissecting out the mesh along its track with scissors while pulling firmly on the exposed end. Although the mesh is tissue integrated, it can be removed without adjacent soft-tissue damage. There is a risk of recurrent ptosis, which can be corrected subsequently using the autogenous fascia lata (AFL), regarded by the authors as the gold standard, or a 2.0 Prolene suture as (often temporary treatment) in the very elderly under local anaesthesia or the very young (less than 4 years of age) where the leg is still too short for adequate AFL harvest.
Steps to minimise Mersilene® mesh complications include cutting the mesh 5 mm wide or less, eyelid skin crease stab incision closure, burying the mesh knot well beneath the frontalis muscle, and a postoperative course of systemic antibiotics.2,3,4,5,6,7,8,9 Some centres also recommend the mesh be soaked in antibiotics prior to insertion, but this is not regarded as mandatory.
Complications with nonautogenous frontalis suspension materials should be dealt with promptly with systemic antibiotics and if required surgical removal of the granuloma with extensive removal of the infected material, dissecting down to integrated noninfected mesh. Based on these cases, we recommend a clear management plan for treatment of postoperative infection and mesh extrusion (Table 1).
References
Fox SA . Congenital ptosis II Frontalis sling. J Pediatr Ophthalmol 1966; 3: 25.
Downes RN, Collin JRO . The Mersilene mesh ptosis sling. Eye 1990; 4: 456–463.
Whitehouse GM, Grigg JRB, Martin FJ . Congenital ptosis: results of surgical management. Aust & N Z J Ophthalmol 1995; 23: 309–314.
Hintschich CR, Zurcher M, Collin JRO . Mersilene mesh brow suspension: efficiency and complications. Br J Ophthalmol 1995; 79: 358–361.
Gabrieli CB, Recupero SM, Contestabile MT, Pacella A . Ophthalmic Surg Lasers 1996; 27: 924–928.
Yalez M, Demircan N, Yagmur M, Haciyakupoglu G . Mersilene mesh: long-term results in oculoplastic surgery. Orbit 1997; 16: 217–223.
Mutlu FM, Tuncer K, Can C . Extrusion and granuloma formation with Mersilene mesh brow suspension. Ophthalmic Surg Lasers 1999; 30: 47–51.
El-Toukhy E, Salaem M, El-Shewy T, Levine M . Mersilene mesh sling as an alternative to autogenous fascia lata in the management of ptosis. Eye 2001; 15: 178–182.
Kemp EG, MacAndie K . Mersilene mesh as an alternative to autogenous fascia lata in brow suspension. Ophthalmic Plast Reconstr Surg 2001; 17: 419–422.
Author information
Authors and Affiliations
Additional information
Presented at the Inaugural Meeting of the British Oculoplastic Surgery Society 20–21 May 2001
Rights and permissions
About this article
Cite this article
Mehta, P., Patel, P. & Olver, J. Management of Mersilene® mesh chronic eyelid complications: a systematic approach. Eye 18, 640–642 (2004). https://doi.org/10.1038/sj.eye.6700681
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.eye.6700681