Abstract
Objective
To report on bilateral sequential macular hole repair.
Design
Retrospective case series report.
Participants
Sixteen eyes of eight patients with reduced visual acuity (VA) and metamorphopsia due to bilateral macular hole.
Intervention
Patients underwent vitrectomy surgery for bilateral macular hole. Seven patients had both eyes operated on consecutively at the same operating session. One patient had surgery to the fellow eye the next day. Strict facedown posturing was undertaken for 1 week by all patients.
Main Outcome Measures
Closure of macular hole; final VA; complications.
Results
In 15 (94%) eyes the macular holes closed with resolution of symptoms; the mean VA at discharge was 6/15; two patients had reduced VA due to age-related macular degeneration (6/36, 6/18); five eyes had entry site tears; there was one case of lens touch with elevated intraocular pressure (IOP); in one (6%) patient the macular hole reopened after later cataract surgery (VA 6/24).
Conclusions
Surgical closure of bilateral macular holes at the same operating session has distinct advantages but also considerable disadvantages. Case selection is paramount—patients require careful preoperative counselling and postoperative support, especially during the posturing week.
Similar content being viewed by others
Introduction
We report on a series of patients for whom surgery for simultaneous bilateral macular hole was performed at the same operating session. Bilateral macular holes are typically repaired with a few months between procedures as the endotamponade agent severely compromises the patient's vision until it is absorbed. To our knowledge this represents an alternative and perhaps controversial approach to bilateral macular holes of which we can find no previous reports.
Materials and methods
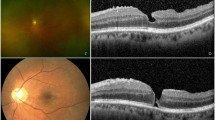
Sixteen eyes of eight patients were selected all complaining of metamorphopsia and reduced visual acuity (VA). Their mean age was 71.4 years. The mean duration of symptoms was 4.6 months and mean VA 6/30. The macular holes were classified as being stage II (1/16 eyes), stage III (12/16 eyes), and stage IV (3/16 eyes) by the Gass classification. Seven patients (14/16 eyes) were bilaterally phakic and one patient (2/16 eyes) pseudophakic.
Intervention
Four patients underwent vitrectomy surgery using sub-Tenon local anaesthetic (8 ml 50/50 mix lidocaine 2% and bupivocaine 0.5%) as day cases. One patient requested to have fellow eye surgery the next day due to anxiety over having two concurrently anaesthetized eyes. Four patients underwent the procedure under a general anaesthetic.
A 3-port 20-guage pars plana vitrectomy was performed and posterior vitreous detachment was induced, if not already present. Three internal limiting membrane (ILM) peels were performed with membrane-blue-assisted staining. Endotamponade was achieved with SF6 in 14 patients and with C3F8 in two patients who were anticipated to struggle with posturing. Patients were asked to posture strictly facedown for 1 week.
Results
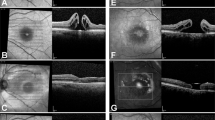
In 15 (94%) eyes, the macular holes closed with resolution of symptoms.
At discharge, the mean VA was 6/15. Two patients with age-related macular degeneration had VAs of 6/36 and 6/18. Five eyes had entry site tears. No patient had retinal tears bilaterally. One patient had a postoperative intraocular pressure (IOP) rise and lens touch without breeching the posterior capsule. In one (6%) eye the macular hole reopened after cataract surgery (VA 6/24). One patient subsequently developed an epiretinal membrane that required peeling. Of the phakic eyes, 100% developed cataract and all underwent uncomplicated bilateral sequential phacoemulsification surgery.
Discussion
Macular holes represent full-thickness defects of the neural retina at the anatomic fovea1 that result in decreased central vision.2 They occur in the middle-aged elderly group and are most commonly unilateral.3
Bilateral macular holes are atypical;4 the literature reports a variable incidence: 10,3 11,5 13,6 and 3–31%.7 The mean time-to-onset in the fellow eye is reported to be 17.5 months in one study.8
Opinion remains divided over prognostic factors for hole closure. Oz et al9 (22 eyes of 21 patients) report that only the stage of hole is important, with stage II macular hole repair yielding the best results. Jaycock et al10 suggest (55 patients) that duration of preoperative symptoms, ILM peeling, and better preoperative acuity are more most important. Mester and Becker11 in their series of 135 eyes found that only the age of the macular hole was significantly predictive. It may therefore be justified to reduce waiting times for repair as much as possible to improve success rates.
Macular holes arise in an age group for whom posturing can be especially demanding,12 particularly if there is pre-existing cervical spine disease or other co-morbidities. Moreover, posturing can be associated with complications.13, 14 It is therefore desirable that overall duration of posturing be minimized. Although some series15, 16, 17, 18, 19, 20 suggest that the success rate of macular hole surgery is unaffected by prone posturing, no randomized-controlled trial has so far addressed the issue. Facedown posturing is still routine practice for the authors.
In our series of idiopathic bilateral macular holes, we operated on both eyes of patients during the same operating session. Our literature search only found one previous report21 of a series on bilateral macular hole surgery with repair performed on separate dates. Here closure was achieved in 74% of eyes overall (46/62 eyes) and 89% (55/63 eyes) with reoperation.
In our series of a mixture of stage II (1/16), stage III (12/16) and stage IV (3/16) macular holes, closure was achieved in 94% (15/16 eyes) of cases. Importantly, from the patients’ perspective, the mean duration of symptoms was 4.6 months. This is considerably shorter than in the Tabandeh study.21 The closure rate compares favourably with results of both posturing22 and non-posturing15, 16, 17, 18, 19, 20 studies.
Our approach provides distinct advantages and disadvantages. The main advantages are the patient undergoes one surgical session; the mean duration of symptoms is reduced; patients only undergo one general anaesthetic (if required); there is only one posturing episode; there are fewer hospital visits; less systemic IOP-lowering treatment or analgesia is used where necessary.
The main disadvantages are that the patient is functionally blind until the gas is at least partly absorbed. This is a prolonged problem with those requiring longer-acting tamponade, and a compelling argument against bilateral surgery. There is also a theoretical risk of bilateral endophthalmitis, and postoperative discomfort may be greater. Careful preoperative counselling, patient selection, and postoperative home support are essential when considering bilateral sequential macular hole repair.
References
Ho AC, Guyer DR, Fine SL . Macular hole. Surv Ophthalmol 1998; 42 (5): 393–416.
Mann DF . Idiopathic macular hole. Optom Clin 1996; 5 (1): 95–110.
Yanoff M, Duker J . Ophthalmology Mosby 1999 Chapter 8 p 31.3–31.5.
Szijarto Z . Bilateral full-thickness macular hole: a case report. Ann Ophthalmol (Skokie) 2006; 38 (2): 149–151.
Niwa H, Terasaki H, Ito Y, Miyake Y . Macular hole development in fellow eyes of patients with unilateral macular hole. Am J Ophthalmol 2005; 140 (3): 370–375.
Lewis ML, Cohen SM, Smiddy WE, Gass JD . Bilaterality of Idiopathic macular holes. Graefes Arch Clin Exp Ophthalmol 1996; 234 (4): 241–244.
McDonnel PJ, Fine SL, Hills AI . Clinical features of idiopathic macular holes. Am J Ophthalmol 1982; 93: 777–781.
Lewis ML, Cohen SM, Smiddy WE, Gass JD . Bilaterality of Idiopathic macular holes. Graefes Arch Clin Exp Ophthalmol 1996; 234 (4): 241–244.
Oz O, Fudenmburg SJ, Cakir B, Jones MP, Levent A . Predictors of success in macular hole surgery with emphasis on the internal limiting membrane and ILM peeling. Ophthalmic Surg Lasers Imaging 2004; 35 (3): 207–214.
Jaycock PD, Bunce C, Xing W, Thomas D, Poon W, Gazzard G et al. Outcomes of macular hole surgery: implications for surgical management and clinical governance. Eye 2005; 19 (8): 879–884.
Mester U, Becker M . Prognostic factors in surgery of macular holes. Ophthalmologe 1998; 95 (3): 158–162.
Charles S, Katz A, Wood B . Vitreous Microsurgery 3rd edn. Lippincott: Williams and Wilkins, 2002, Chapter 1, p 2.
Holekamp NM . Ulnar neuropathy as a complication of macular hole surgery. Arch Ophthalmol 1999; 117 (12): 1607–1610.
Vincent JM, Peyman Ga, Ratnakaram R . Bilateral Ulnar decubitis as a complication of macular hole surgery. Ophthalmic Surg Lasers Imaging 2003; 34 (6): 485–486.
Szurman P, Di Tizio FM, Lafaut B, Aisenbrey S, Grisanti S, Roters S et al. Significance of postoperative face-down positioning after surgery for idiopathic macular holes: consecutive case–control study. Klin Monatsbl Augenheilkd 2000; 217 (6): 351–355.
Simcock PR, Scalia S . Phacovitrectomy without prone posture for full thickness macular holes. Br J Ophthalmol 2001; 85 (11): 1316–1319.
Rubenstein A, Ang A, Patel CK . Vitrectomy without post-operative posturing for idiopathic macular holes. Clin Experiment Ophthalmol 2007; 35 (5): 458–461.
Merkur AB, Tuli R . Macular hole repair with limited non-supine posturing. Retina 2007; 27 (3): 365–369.
Tornambe PE, Poliner LS, Grote K . Macular hole surgery without face-down posturing. A pilot study. Retina 1997; 17 (3): 179–185.
Tranos PG, Peter NM, Nath R, Singh M, Dimitrakos S, Charteris D et al. Macular hole surgery without prone posturing. Eye 2007; 21 (6): 802–806.
Tabandeh H, Smiddy WE, Mello M, Flynn HW, Feuer WJ . Outcomes of bilateral macular hole surgery. Ophthalmic Sur Lasers 2002; 33 (1): 9–15.
Benson WE, Cruickshanks KC, Fong DS, Williams GA, Bloome MA, Frambach DA et al. Surgical management of macular holes: a report by the American Academy of Ophthalmology. Ophthalmology 2001; 108: 1328–1335.
Author information
Authors and Affiliations
Corresponding author
Additional information
No proprietary interests or research funding.
Rights and permissions
About this article
Cite this article
Gupta, D., Goldsmith, C. & Burton, R. Surgery for bilateral macular holes. Eye 23, 556–558 (2009). https://doi.org/10.1038/eye.2008.75
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/eye.2008.75
Keywords
This article is cited by
-
Immediate sequential bilateral vitreoretinal surgery (ISBVS): retrospective study from a tertiary academic center
Graefe's Archive for Clinical and Experimental Ophthalmology (2023)