Abstract
Deep brain stimulation (DBS) modulates local and widespread connectivity in dysfunctional networks. Positive results are observed in several patient populations; however, the precise mechanisms underlying treatment remain unknown. Translational DBS studies aim to answer these questions and provide knowledge for advancing the field. Here, we systematically review the literature on DBS studies involving models of neurological, developmental and neuropsychiatric disorders to provide a synthesis of the current scientific landscape surrounding this topic. A systematic analysis of the literature was performed following PRISMA guidelines. 407 original articles were included. Data extraction focused on study characteristics, including stimulation protocol, behavioural outcomes, and mechanisms of action. The number of articles published increased over the years, including 16 rat models and 13 mouse models of transgenic or healthy animals exposed to external factors to induce symptoms. Most studies targeted telencephalic structures with varying stimulation settings. Positive behavioural outcomes were reported in 85.8% of the included studies. In models of psychiatric and neurodevelopmental disorders, DBS-induced effects were associated with changes in monoamines and neuronal activity along the mesocorticolimbic circuit. For movement disorders, DBS improves symptoms via modulation of the striatal dopaminergic system. In dementia and epilepsy models, changes to cellular and molecular aspects of the hippocampus were shown to underlie symptom improvement. Despite limitations in translating findings from preclinical to clinical settings, rodent studies have contributed substantially to our current knowledge of the pathophysiology of disease and DBS mechanisms. Direct inhibition/excitation of neural activity, whereby DBS modulates pathological oscillatory activity within brain networks, is among the major theories of its mechanism. However, there remain fundamental questions on mechanisms, optimal targets and parameters that need to be better understood to improve this therapy and provide more individualized treatment according to the patient’s predominant symptoms.
Similar content being viewed by others
Introduction
The use of deep brain stimulation (DBS) as a treatment for neuropsychiatric disorders and symptoms is among the most important recent advances in clinical neuromodulation. DBS is a neurosurgical procedure that involves the implantation of electrodes into specific brain targets to modulate local and widespread connectivity in dysfunctional networks [1]. To date, several thousands of patients have undergone DBS for various neuropsychiatric conditions [2,3,4,5,6]. Notably, patients with Parkinson’s disease (PD) are among the most common candidates for this treatment option [7]. In select cases, DBS can also induce long-term alleviation of symptoms in patients with dystonia [8], Tourette’s syndrome [9], or epilepsy [10]. In terms of psychiatric conditions, clinical DBS studies have shown promise in relieving symptoms of obsessive-compulsive disorder (OCD) [11, 12], major depressive disorder [13], and substance use disorder (SUD) [14, 15]. Despite encouraging reports, the optimal DBS brain targets and underlying mechanisms that lead to benefits and/or side effects in distinct pathologies remain unclear.
Experimental DBS in animal models plays an essential role in our understanding of the multiscale neurobiological mechanisms of DBS, as well as the development of new technologies. Rodents — in particular, the Norway rat (Rattus norvegicus) and the house mouse (Mus musculus) — are especially useful for this purpose. Different models can capture core features observed in neuropsychiatric disorders and can be objectively tested in a series of standardized behavioural tests. In addition, the underlying mechanisms of DBS may be explored using healthy rodent strains [16, 17]. In this article, we present a systematic review of preclinical DBS studies to synthesize the literature on the current landscape of DBS in rodent models.
Methods
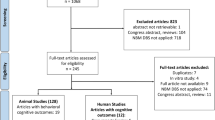
A systematic analysis of the international literature was performed in accordance with PRISMA [18] guidelines (See Supplementary Fig. 1 for PRISMA flow diagram). The PubMed MEDLINE (National Library of Medicine) database was used to search articles published between January 2000 and December 2022, using the search terms “deep brain stimulation”, “DBS”, “rodent”, “mouse”, and “rat”. Duplicates and unrelated reports were excluded. The remaining reports were first screened by title and abstract, then selected articles progressed to full-text review based on prespecified inclusion and exclusion criteria (Inclusion: Studies published in English, Original articles with full-text availability, Articles describing studies of DBS in rats or mice, Articles reporting stimulation parameters used; Exclusion: Non-original studies (i.e., conference abstracts, reviews, meta-analyses, commentaries, editorials, and protocols), Articles reporting on clinical population, Articles using other neuromodulatory techniques, Investigations performed in-vitro or using other species) See Supplementary References for full list of included studies. Data extraction was performed by three authors (KZ, RM, FVG) focusing on 5 categories: Bibliographic data, Animal model characteristics (group based on DSM-5 classification [19]; Supplementary Table 1), DBS target and settings, Behavioural outcomes, Mechanisms of action.
Results
Of the 1674 reports screened, 407 original research articles were included in this review (rat: 356, mouse: 51; Supplementary Fig. 1, Supplementary References). Considering the differences in disease models between species (which may involve distinct cellular and molecular targets), the data extracted from mouse and rat studies are presented separately (see Supplementary Table 2 for the summary of combined data).
Rodent models of DBS
Figure 1 shows the proportion of articles published by the disease model and the distribution of these articles over the years. Among rat studies, DBS effects have been investigated in 15 distinct models of disorders and in animals presenting no pathology (i.e., standard healthy strains; Fig. 1A). DBS for movement disorders was the most researched field and included Parkinson’s disease (PD; 24.2%), motor impairments (1.1%), dyskinesia (0.8%), and tremor (0.6%). Depression and epilepsy were the second and third most studied models, followed by SUD (Cocaine 2.8%, Morphine 2.8%, Alcohol 0.8%, Methamphetamine 0.6%, Heroin 0.3%). Models of dementia/cognition focused on cognitive performance (3.8%), Alzheimer’s disease (AD; 1.1%), and dementia (1.1%). Models of physical injury (traumatic brain injury, TBI: 1.4%, pain: 1.1%, spinal cord injury: 1.1%, stroke: 0.6%, ischemia: 0.3%) and eating disorders (obesity: 1.4%, food intake: 0.8%, hedonic feeding: 0.8%, glucose metabolism: 0.3%), occupied smaller portions of the rat DBS landscape. Trauma or stressor-related disorders (i.e., post-traumatic stress disorder, PTSD), obsessive-compulsive disorder, psychosis, anxiety disorders, tinnitus, neurodevelopmental disorders, bladder function (related to neurological disorders), and sleep-wake disorders represented the least studied rat models for DBS.
For mouse studies, DBS effects have been investigated in 12 distinct models of disease and in healthy strains (Fig. 1B). Dementia/cognition (AD: 9.8%, cognitive performance: 3.9%, dementia: 2.0%) and movement disorders (PD: 9.8%, ataxia: 3.9%, tremor: 2.0%) were the most studied, followed by depression models. Neurodevelopmental disorders (Rett syndrome: 5.9%, Autism Spectrum Disorder, ASD: 2.0%), SUD (alcohol: 2.0%, cocaine: 3.9%), epilepsy, anxiety disorders, eating disorder (hedonic feeding: 2.0%, obesity: 2.0%), and physical injury (TBI: 2.0%, stroke: 2.0%) were investigated less frequently. OCD, psychosis, and sleep-wake disorder represented the least studied mouse models for DBS. There has been an upward trend in preclinical DBS publications since the early 2000s (Fig. 1C & D). To our knowledge, no rat DBS study was published between 2000–2002, and no mouse DBS study was published between 2000–2007. In the early stages, these studies focused on PD, epilepsy, or healthy animals; however, the disease models evaluated for DBS effects have substantially diversified over time.
Model characteristics
Although Sprague-Dawley (SD; 52.9%) and Wistar rats (30.1%) were the main healthy strains used (Fig. 2A), a handful of studies used Long Evans or Lewis rats to model psychosis [20], OCD [21,22,23], cocaine [24, 25] or alcohol addiction [26], catalepsy [27,28,29], PD [30,31,32,33,34,35,36,37,38,39,40,41,42,43,44], TBI [45, 46], and spinal cord injury [27, 28]. The unilateral 6-hydroxydopamine (6-OHDA) nigrostriatal lesion PD model was the most commonly used ( > 87% of included studies). While neurodevelopmental disorders were modelled in SD rats by exposure to valproic acid [47, 48], apomorphine [49] or antinuclear antibody [50], the Flinders Sensitive Line and Zucker rats were used exclusively to model depression and obesity, respectively. For modelling epilepsy, most studies used SD and Wistar rats receiving chemoconvulsants (e.g., kainic acid, pilocarpine, pentylenetetrazol, or FeCl3 solution in one study [51]) or chronic electrical stimulation of the temporal lobes, predominantly the amygdala. Transgenic models of absence seizures (i.e., Generalized Absence Epilepsy in Rats from Strasbourg [52], and Wistar Albino Glaxo/Rijwijk [52, 53]), AD [54, 55] and Huntington’s disease [56] were less frequently used. Conversely, almost half of mouse models (44.2%) were generated using transgenic mice (Fig. 2B), especially for studying neurodevelopmental disorders (i.e., MECP2 [57,58,59,60], Shank3 [57], or CDKL5 [61]), OCD (i.e., Sapap3 [62]) and sleep-wake disorders (i.e., Tg(HCRT-MJD)1Stak [63]) which used transgenic animals exclusively. The C57BL/6J mouse (46.2%) was the most common healthy strain used, with animals being exposed to external factors to induce symptoms. The high percentage of studies using transgenic mouse models may help explain the great difference between the rat and mouse literature reporting on using both males and females in the same study (Rat: 1.9%, Mouse: 19.2%). Nevertheless, most studies utilized only male animals for both species (Fig. 2). Supplementary Table 3 describes the validity of rodent models of disease.
Stimulation parameters
DBS parameters are generally programmed by amplitude (Amperes [A] or Volt [V]), pulse width (seconds), and frequency (Hertz [Hz]). Among the included studies, DBS was predominantly administered at high frequency (130 Hz), short pulse duration (60 µs), and amplitudes of 100 µA or 2.7 V. Although the average parameters used in rat and mouse models fell within similar ranges, the average stimulation parameters were higher in rats. Understanding the pattern of stimulation is fundamental for advancing the preclinical field of research and interpreting the results reported. See Supplementary Table 4 for a detailed description of the stimulation parameters reported. In rats, the highest average amplitude was observed in healthy strains, neurodevelopmental disorders and epilepsy, and the lowest average amplitude was reported in models of OCD and tinnitus. However, studies using healthy strains also showed the largest amplitude range, followed by models of movement disorders and dementia/cognition. For mouse studies, the largest average amplitude was observed in models of OCD and physical injury, and the lowest was reported in models of neurodevelopmental disorders. Notably, a few studies reported stimulation intensities above 1000 µA [64,65,66], resulting in a large overall range. Most studies used high-frequency stimulation, with 1 kHz being the max for healthy rats and mice. The lowest frequency was observed in rat and mouse models of epilepsy, as well as rat studies of dementia/cognition and movement disorders. On average, studies in rats employed longer pulse widths; however, both species showed the same mode (60 µs).
There was large heterogeneity surrounding stimulation duration and administration pattern among the included studies. While acute stimulation (i.e., stimulation ≤ 1 day) was more commonly observed in rat studies, chronic stimulation (i.e., stimulation ≥ 2 days) was more frequently applied in mouse studies (Fig. 3). DBS has also been applied intermittently (series of sessions with DBS-on separated by periods of DBS-off), continuously (DBS-on only), or during behavioural testing (the least explored option in both species). Although rat studies similarly used continuous or intermittent stimulation, mouse studies focused on intermittent stimulation, performed twice as often as continuous stimulation.
Brain targets
The majority of studies targeted telencephalic brain areas (rat: 43.7%, mouse: 47.9%) and diencephalic areas (rat: 39.7%, mouse: 29.2%). While white matter structures were more commonly targeted in mouse studies (rat: 5.2%, mouse: 16.7%), mesencephalic areas were more frequently targeted in rat studies (rat: 7.1%, mouse 4.2%). The metencephalon was the target of DBS in 4% of rat studies and 2.1% of mouse studies, and the olfactory bulb was targeted in rats only (0.2%; Fig. 4). Across rat studies, the subthalamic nucleus (STN) was the most common target (22.2%), followed by the thalamus (13.5%), nucleus accumbens (nAcc; 11.7%), and frontal cortex (FC; 11.2%, Fig. 4A). Although the majority of studies targeting the STN investigated models of PD, a few articles have also explored this target in models of SUD [24, 67], depression [68, 69], epilepsy [70, 71], OCD [23], and psychosis [72]. Thalamic targets have been studied in various models, with the anterior nucleus of the thalamus (ANT) being predominantly studied in epilepsy [73,74,75,76,77,78,79,80,81,82,83]. The nAcc was targeted in over half of studies investigating SUD and has also been explored in models of eating disorders, depression, OCD, psychosis, and anxiety disorder. Overall, 17% of the studies using healthy strains targeted the core and shell aspects of the nAcc. FC structures have been extensively targeted in healthy strains [84,85,86,87,88,89,90] and in models of depression, SUD [91,92,93], psychosis [72, 94, 95], cognitive performance [96, 97], anxiety [98], ASD [48], eating disorder [99], and PTSD [100], with most studies applying chronic stimulation, including chronic continuous stimulation for several days [68]. Among mouse studies (Fig. 4B), the thalamus and nAcc were the most commonly targeted brain structures (both 14.8%), followed by the STN (13%) and fornix (10.9%). The central nucleus of the thalamus was the thalamic region most commonly targeted (40%), mainly in studies investigating underlying mechanisms of DBS in healthy strains. Stimulation of the nAcc was investigated in models of depression [101, 102], anxiety disorder [103], eating disorder [104], and SUD [105, 106] however, the number of articles on each model is limited. The STN was predominantly explored in the context of movement disorders [107,108,109] (71%), and forniceal stimulation has been investigated exclusively in models of neurodevelopmental disorders [58,59,60] and dementia/cognition [61, 110, 111].
Mechanisms of action
DBS effects on neurochemistry and electrophysiology were the most commonly investigated mechanisms. These studies focused on neuronal activity (26%), gene/protein expression (25.3%), neurotransmitter levels (23%), neuroinflammation and neuroprotection (15.5%), and neural/synaptic plasticity (6.6%). Electrophysiological studies accounted for 31.7% of published articles (Table 1). In models of depression, anxiety disorder, OCD, and PTSD, the DBS-induced antidepressant- and/or anxiolytic effects were associated with changes in serotonin and dopamine levels, as well as modulation of neuronal activity along the mesocorticolimbic circuit. In DBS for PD and movement disorders, the improvements in motor and non-motor symptoms following treatment have primarily been attributed to modulation of the striatal dopaminergic system through the protection of dopaminergic cells and normalization of dopamine signalling. In models of dementia and epilepsy, DBS attenuates aberrant cellular and molecular changes in the hippocampus, a key structure involved in both memory function and seizure generation. Electrophysiological data were limited in models of dementia and memory, OCD, physical injury, and SUD and were not reported in anxiety disorder, bladder function, and eating disorders. In contrast, the majority of studies using non-pathological strains reported on DBS-induced electrophysiology effects, which were target- and parameter-specific.
Behavioural outcomes
To investigate if DBS treatment would improve symptoms or behaviours, a large portion of the studies included behavioural tests performed either at the end or during treatment (Tables 1–2, Supplementary Table 5). While 73% of rat studies employed behavioural tests, with positive outcomes reported in 83.4%, 81.4% of mouse research investigated behavioural outcomes, reporting improvement in 88.6% of the studies. Although some behavioural tests are more frequently used in one species over the other, several tests are established and commonly performed in both rats and mice. The open-field test was widely used to assess locomotor activity and/or anxiety-like behaviour in several disease models. The Morris Water Maze was used to investigate spatial memory in models of dementia, the Forced Swimming Test was used for assessing immobility (as a measure of behaviour despair) in models of depression, and the Drug Self-Administration paradigm was used in substance use disorder models. Moreover, quantification of food intake was used in models of eating disorders for both species, as well as recording seizure frequency in models of epilepsy.
Adverse events
Only a few studies reported adverse effects from DBS treatment (rat: n = 24, mouse: n = 1). The most commonly reported side effects were brain injury at the insertion site (i.e., hemorrhage, lesions, inflammation) [70, 112,113,114,115,116] and seizures (onset or worsening) [117,118,119,120,121,122] when very high frequencies or amplitudes were used [122]. Following DBS, two articles observed depressive-like behaviours in models of movement disorders [69, 109], three articles reported increased impulsivity [21, 22, 123], and two reported tremors [20, 124]. Few studies observed side effects of anxiety-like behaviour [125], mania [126], unexpected weight change [127], fragmented sleep-wake cycles [53], impaired memory [128], and kindling [55].
Discussion
Rodent models of DBS
The strength of rodent models for DBS research is rooted in dimensions of face (model’s ability to reflect clinical symptoms), construct (similar disease etiology between human condition and preclinical models), and predictive (response to treatments seen in clinical populations) validity. Most rodent models used in DBS studies demonstrate high face and construct validity, being valuable for analyzing the pathophysiology and behavioural effects of treatment, thus facilitating the development and optimization of therapies [129,130,131]. Transgenic models of neurological and psychiatric disorders, as well as healthy strains, have been extensively used to provide insights into the intrinsic mechanisms of DBS, treatment safety, and potential adverse effects of stimulation, significantly contributing to advancing the current knowledge and showing great potential for developing targeted therapies [129,130,131]. These models, however, do not capture all features of human disease but mimic specific relevant symptoms [129,130,131]. The unilateral 6-OHDA model is the most common model of PD and involves the degeneration of nigrostriatal dopaminergic neurons [132, 133] leading to major motor dysfunctions (e.g., akinesia, tremor) and basal ganglia neuroplasticity similar to what is observed in patients [134]. Although these features support the strong face validity of the model, the behavioural and cellular effects produced in this model depend on the site of drug injection [133], and the resulting changes in glutamate release and beta band frequency in response to DBS are different from those observed in humans [135]. Transgenic models of PD are a good alternative, as they present multiple and more complex symptoms, such as observed in patients [107,108,109, 136, 137]. Neurodegenerative diseases of aging, such as AD, have also been studied in rodent models either using aged animals [55], intracranial injection of chemicals [138,139,140,141,142] or transgenic models with mutations in AD-related genes [66, 111, 143,144,145,146]. These models exhibit clinically relevant features, including the development of β-amyloid plaques and Tau protein aggregates and cognitive decline, which are excellent models for DBS research.
In epilepsy research, chemoconvulsants (e.g., kainic acid, pilocarpine, pentylenetetrazole) are frequently used to generate rodents with spontaneously recurrent seizures [147]. These drugs induce extensive hippocampal sclerosis and mossy fibre sprouting in the dentate gyrus [148,149,150], and these models have strong face validity for temporal lobe epilepsy. Electrical kindling models can be generated by delivering chronic stimulation to the hippocampus or the amygdala, allowing for the screening and study of antiseizure treatments for chronic cases of epilepsy [151]. Genetic models are also very attractive to study epilepsy, providing strong construct validity as the mechanisms underlying epileptogenesis more accurately reflect the disease etiology in humans. However, the induction of seizures through chemoconvulsants is not representative of the clinical causes of epilepsy, kindled animals do not typically exhibit spontaneous recurrent seizures, thus limiting the translatability of findings, and transgenic animals may not exhibit the full range of complex alterations observed in patients.
Depression/anxiety are widely investigated models for DBS, having strong predictive and construct validity. Models of depression/anxiety can be generated through neurobiological and genetic manipulation (i.e., selective breeding of rats with a predisposition to depression or knockouts of serotonin-related genes) or via chronic exposure to stressors, which captures the delay in antidepressant efficacy seen in patients [152]. Additionally, these models lead to impairments in the hypothalamic-pituitary-adrenal axis, altered immune reaction, and changes in monoaminergic transmission similar to those detected in patients with depression [153]. Generally, DBS applied to rodent models of depression has demonstrated comparable effects to those observed in patients, such as increased monoamine concentrations in the prefrontal cortex (PFC) [154] and hippocampus [155] and normalization of local field potential activity at the ventral tegmental area (VTA) [156, 157]. Transgenic mice, but not rats, are also widely used in investigations of neurodevelopmental disorders. These include animals with mutations targeting genes known to be related to the disease in humans, such as MECP2 [58,59,60], Shank3 [57], and CDKL5 [61]. In contrast, rat studies focused on exposing naïve rats to chemicals to induce epigenetic changes [158] and subsequent ASD-like phenotypes [47,48,49] or injecting animals with patient-derived antinuclear antibodies to induce Tourette-like symptoms [50].
One major aspect of the experimental DBS landscape that requires dire attention is the need to include females in DBS studies. In this review, we found that only 1.9% of rat studies and 19.2% of mouse studies included females. The consideration of both sexes is important because DBS can have distinct effects on males and females due to differing biological attributes, such as genetics, physiology, brain anatomy, and hormones. For instance, several groups have reported behavioural and morphological differences among male and female 6-OHDA-lesioned rats [159, 160], which may subsequently affect DBS response. Similar observations have been made in models of addiction, whereby female rodents are more likely to consume and seek drugs in self-administration paradigms [161]. Thus, future experimental DBS studies should evolve to include both male and female models in order to address differing therapeutic effects influenced by sex.
DBS parameters and electrode characteristics
DBS parameters such as amplitude, frequency, pulse width, and duration of treatment can vary across brain targets, disease indication, and electrode design. In the clinic, the ranges within which most stimulation parameters fall are in amplitudes between 1–3.5 V, frequencies between 80–185 Hz, and pulse width between 60–210 µs [162]. By means of translation to human DBS, more groups have started to apply clinically relevant DBS paradigms in rodent models. The use of high- or low-frequency stimulation to specific brain areas plays a large role in the overall effects of DBS in both rodent models and humans and may result in different local and widespread plastic brain changes that can be captured in studies evaluating electrophysiological and neurochemical responses associated with DBS [7]. For instance, high-frequency stimulation (HFS; >90 Hz) of the STN in PD models improves motor symptoms, whereas low-frequency stimulation (<50 Hz) is ineffective or exacerbates symptoms [163]. In contrast, although the majority of addiction studies employed HFS, some applying <20 Hz stimulation to the nAcc [25], lateral habenula [164], ventral striatum [165], or STN [67] demonstrated beneficial behavioural effects. In the same manner, there is debate regarding the use of intermittent vs. continuous stimulation. DBS has traditionally been delivered in a continuous fashion in the clinical setting; nonetheless, recent preclinical studies have suggested that a cyclic DBS programming approach may produce beneficial effects [55, 120]. Furthermore, several groups have begun to develop closed-loop adaptive DBS systems and advancements in this field (using both preclinical models and humans) will help us better understand the neural basis and overall effectiveness of such a technology.
The size, shape, and area of microelectrode implantation can affect the volume of tissue activated by stimulation and overall brain tissue reactivity or potential neural damage [166]. The large majority of DBS studies in rodents used bipolar stainless steel electrodes with a diameter between 125–300 µm for rats and 50–125 µm for mice. In recent years, there has been an increase in options for electrode materials such as platinum-iridium, tungsten, and carbon fibres. Platinum is a relatively non-toxic and biologically magnetic inert material in brain tissue and is similar to that used in humans [167]. Tungsten electrodes present low impedance, high conductivity, uniform plastic deformation, and MRI compatibility [168]. The use of carbon fibre electrodes for DBS and neural recording has also gained traction because of its ability to produce fewer MRI artifacts, improve magnetic field homogeneity, and induce smaller temperature changes in MR environments when compared to other metal-based electrodes [167, 169]. However, there are technical challenges surrounding the assembly and implantation of these flexible fibre electrodes, requiring a high level of surgical expertise [170].
DBS brain targets
Regarding brain targets, there is currently no universal consensus on the best target for DBS, notwithstanding the disease indication. Thus, preclinical studies provide great value in our understanding and development of potential therapeutic targets. The most evident example is the DBS of the STN in PD, which is now an extensively used target in the clinic. The STN was found to exhibit unusually increased activity in animals with Parkinsonian symptoms, and experimental lesions of the STN in rats resulted in evident improvements in motor dysfunction [171]. These findings supported the hypothesis that pathological activity occurs in the STN in PD, and modulation of this area can improve Parkinsonian symptoms. Accordingly, studies using rodent models have demonstrated that STN-DBS significantly reduces tremors, rigidity, and bradykinesia associated with PD. However, consistent with clinical observations, some rodents treated with STN-DBS also exhibited enhanced depressive-like behaviours [68, 69, 172]. Thus, other key brain structures, such as the entopeduncular nucleus [35, 173], pedunculopontine tegmental nucleus [116, 174,175,176,177], substantia nigra [178, 179], and zona incerta [172] have been considered for DBS targeting in movement disorder rodent models in hopes of alleviating non-motor symptoms.
Epilepsy research has concentrated on stimulating various aspects of the thalamus to alleviate seizure activity. Thalamic nuclei are highly interconnected with substantial bidirectional projections via the mammillothalamic, thalamocortical, and spinothalamic tracts. Thus, thalamic DBS has been shown to significantly reduce seizure frequency and increase seizure latency, as detected using electroencephalography [180]. DBS targeting the thalamus has also been studied in the context of AD, whereby high-frequency stimulation was shown to be less effective at facilitating spatial memory than the entorhinal cortex or fornix DBS [141]. In line with this finding, Hamani et al. [128]. reported that DBS delivered to the ANT at high amplitude (i.e., 500 µA) disrupts the acquisition of contextual fear conditioning and, in turn, may explain the impaired performance on spatial alternating tasks observed in these rats. In contrast, a recent study by Chamaa et al. showed that both single and repeated sessions of ANT-DBS may induce a significant increase in neurogenesis in the ipsilateral dentate gyrus [181] and improve spatial reference memory on the Y-maze test [182].
In the field of psychiatric disorders, the nAcc is a key DBS target explored for the treatment of SUD, eating disorders, treatment-resistant depression, OCD, and psychosis. Rodents receiving nAcc stimulation show a decrease in consumption, preference, and/or motivation for consuming several substances such as ethanol [26, 106, 183, 184], cocaine [24, 25, 67, 91, 92, 164, 185, 186], and morphine [93, 112, 187,188,189,190]. While most studies showed success in modulating pathologic behaviour using nAcc-DBS, there was conflicting evidence regarding the efficacy of stimulating the nAcc core vs. shell. Several addiction studies showed reduced morphine-induced conditioned place preference and ethanol self-administration regardless of whether the DBS was targeting the nAcc core or shell. In contrast, Vassoler et al. [91] and Wilden et al. [183] demonstrated that DBS of the nAcc shell, but not the nAcc core, reduced cocaine-induced reinstatement. Similar to this observation, Oterdoom et al. [191] reported a reduction in binge-eating behaviour among rats treated with DBS targeting the nAcc shell but not in those targeted at the core aspect of the nucleus. Furthermore, Sesia et al. [21] reported reduced impulsivity when targeting the nAcc core and the opposite effect when targeting the nAcc shell of OCD models. The contradicting findings regarding the optimal DBS target may be explained by the variation in volumes of tissue activated due to differing stimulation parameters applied and differences in cellular characteristics between models.
Mechanisms of action
In rodent DBS research, the most frequent study goal is to offer a better understanding of the mechanisms of action of treatment. Several hypotheses on the mechanism of DBS have been proposed, such as direct inhibition/excitation of neural activity, whereby DBS modulates pathological oscillatory activity within brain networks [7]. However, the precise action of DBS in each brain target and in each neurological or psychiatric disorder remains elusive.
Parkinson’s disease
DBS is considered the standard of care for patients with PD, and the STN represents the most well-studied target for this indication. Several studies describe a neuroprotective effect of STN-DBS on dopaminergic neurons in the substantia nigra [30, 31, 192,193,194] via increased signalling strength in the BDNF-trkB pathway (i.e., brain-derived neurotrophic factor and its receptor tropomyosin receptor kinase B), and increased autophagy through the blocking of protein phosphatase 2A activation [195, 196]. However, these results failed to be replicated in transgenic models of α-Synuclein pathology [197]. Increased levels of BDNF and cerebral dopamine neurotrophic factor in the nigrostriatal system and primary motor cortex have also been associated with positive outcomes following STN-DBS [115, 195, 198,199,200]. Furthermore, STN-DBS is thought to reduce neuroinflammation [201,202,203] due to decreased fractalkine pathway signalling [201,202,203]. Conflicting results have been reported on extracellular levels of dopamine following STN-DBS [204,205,206,207,208], with some studies showing the increase in dopamine metabolites to be associated with a better outcome [204,205,206,207,208]. STN-DBS has also been reported to inhibit serotonergic neurons in the raphe nuclei [29, 209,210,211] and decrease serotonergic transmission in the striatum, hippocampus, and PFC [212, 213], leading to depression [109, 172, 212, 213]. This effect was not observed following entopeduncular nucleus DBS, suggesting that the therapeutic effect of DBS via decreased serotonergic transmission is characteristic of STN-DBS [214, 215]. Electrophysiological studies have associated decreased beta oscillations in cortical and basal ganglia networks [43, 208, 211, 216, 217] and increased alpha power in the medial PFC [218] with improved motor and non-motor symptoms following treatment. In models of motor symptoms not associated with dopamine degeneration (e.g., haloperidol-induced catalepsy, pharmacologically-induced tremor and tardive dyskinesia [219, 220]), STN-DBS improves motor function through the modulation of serotonin transmission hippocampal-striatal coherence, and cortical beta oscillations [29, 209,210,211].
Dementias and Alzheimer’s disease
DBS represents an emerging therapeutic approach for patients with dementia. Improved memory and enhanced hippocampal neurogenesis in the dentate gyrus have been reported following DBS of several brain targets, including the fornix [54, 66], nucleus basalis of Meynert (NBM) [221], medial septum [142, 222], entorhinal cortex (EC) [144], ventral striatum [223], and thalamus [181, 182], and this effect was associated with the restoration of theta oscillations in thalamic nuclei and striatum following treatment [224]. Fornix- and NBM-DBS have also been shown to reduce hippocampal neuronal loss and neuroinflammation [54, 66], whereby fornix-DBS increased hippocampal acetylcholine levels and activity [142, 225]. NBM-DBS promoted cholinergic fibre growth in the cingulate cortex without altering hippocampal acetylcholine levels [221]. Additionally, DBS of the intralaminar thalamic nuclei leads to increased dendritic spine density in cortical and hippocampal pyramidal neurons [64, 138, 221] and altered cortical glutamatergic neurotransmission [226]. The neuropathological hallmarks of AD have also been explored following EC- and fornix-DBS treatments. While both EC- and fornix-DBS reduced cortical and hippocampal amyloid deposition [54, 143, 144, 146], EC-DBS also decreased tau protein levels in the cortex and hippocampus [143, 144, 146] by enhancing enzymes involved in tau clearance [143, 144, 146].
Epilepsy
The ANT is the primary target for treating epilepsy with DBS, as it is approved by the Food and Drug Administration as an adjunctive treatment for reducing the frequency of partial-onset seizures in adult populations [227]. Positive changes in the hippocampus following ANT-DBS have been shown, with enhanced neurogenesis, increased neurotrophic factors, reduced neuroinflammation, reduced mossy fibre sprouting, and anti-apoptotic and neuroprotective effects [75,76,77,78,79,80, 228,229,230]. ANT-DBS anti-seizure effect was also associated with increased adenosine, reduced adenosine kinase levels and changes in gamma-aminobutyric acid (GABA) transmission in the hippocampus [230,231,232,233,234]. Differentially expressed genes involved in ion channel activity, glutamatergic synapse, and regulation of immune response have also been reported in the hippocampus following ANT-DBS [235]. Electrophysiological studies described ANT-DBS to enhance the seizure threshold by decreasing theta oscillations in the hippocampus and cortex and by suppressing delta oscillations during non-rapid eye movement sleep, which results in an increased amount of rapid eye movement sleep [82, 230, 234].
Addiction
It is widely accepted that the initial reinforcing effects of addictive drugs are mediated by enhanced synaptic concentrations of dopamine in forebrain subcortical structures, particularly the nAcc [236, 237], and the prolonged use of drugs leads to an imbalance between excitatory glutamate and inhibitory GABA [236, 238]. Preclinical studies on nAcc-DBS for the treatment of addiction have shown antidromic stimulation of the cortex via cortico-accumbal afferents [91, 165, 239], decreased glutamate and increased GABA levels in the VTA, ventral pallidum, and nAcc [190], upregulation of glutamatergic receptors in the nAcc [105] and amygdala [240], and downregulation of glutamatergic receptors in the VTA [164]. Interestingly, the selective blockade of dopamine 1 receptor (D1R) along with nAcc-DBS reverses cocaine-induced hyperlocomotion and plasticity changes in GABAergic medium spiny neurons expressing D1R via activation of metabotropic glutamatergic receptors [105], suggesting an intricate interaction between neurotransmitter systems is required for the therapeutic effects of DBS.
Eating Disorder
DBS treatment for eating disorders has been described in patients suffering from morbid obesity. The nAcc and the ventral and/or lateral aspects of the hypothalamus are the targets of choice in this patient population, and although DBS was considered to be a safe procedure with encouraging outcomes, it has been associated with side effects such as hardware infection and stimulation-induced mania [241, 242]. nAcc-DBS in rodent models of obesity is associated with decreased high fat/ high sucrose intake [104, 191], improved glucagon and glucose concentrations in plasma and increased neuronal activation in the lateral hypothalamus [243]. Lateral hypothalamus DBS led to reduced body weight and food intake [244, 245], increased metabolism in the mammillary body, hippocampus, and amygdala, and decreased metabolism in the thalamus, caudate, temporal cortex, and cerebellum [245]. This treatment was also associated with reduced markers of activity-induced synaptic plasticity and memory formation in the hippocampus and EC and vesicular GABA transporter [246].
Obsessive-compulsive disorder
Changes in the mesolimbic dopaminergic reward system play a significant role in the pathological habit formation observed in OCD [236, 237]. In clinical populations, the anterior limb of the internal capsule, the nAcc, and the inferior thalamic peduncle are common targets for neuromodulatory treatments of drug-resistant OCD [247,248,249]. In rodent models of OCD, DBS targeting the internal capsule led to increased neuronal activity in the targeted area and in the PFC, which was associated with therapeutic effects [62]. Similarly, DBS of the ventral striatum increased neuronal activity in the targeted area and in the PFC, orbitofrontal cortex (OFC), and amygdala [62, 123]. When targeting the core aspect of the nAcc specifically, DBS reduced OFC neuronal firing and enhanced spontaneous local field potential oscillatory activity in the slow frequency band [239, 250]. nAcc-DBS was also shown to increase dopaminergic and serotonergic in nAcc [21]. Thalamic DBS, however, has a distinct behavioural outcome when different subnuclei are targeted; while DBS of the mediodorsal nucleus of the thalamus increases impulsivity and decreases neuronal activity in cerebellar nuclei and PFC [22], DBS of the parafascicular nucleus of the thalamus alleviates prepulse inhibition [251], a measure of sensorimotor gating which is disrupted in OCD [252, 253]
Depression
Given its key role in emotional processing and depressotypic behaviour, the infralimbic (IL) nucleus (also referred to as the mouse ventromedial PFC, a structure considered to be homologous to the human subgenual cingulum) is the most commonly studied DBS target in models of depression. IL-DBS was shown to enhance serotonin release and induce long-term alterations of serotonin receptor expression [85, 254, 255], an effect that can be blocked by depleting serotonergic transmission [255], and is thought to be mediated by direct modulation of prefrontal projections to the dorsal raphe nucleus [254,255,256,257]. Enhanced levels of serotonin were also reported following DBS of the nAcc [258,259,260], lateral habenula, and medial forebrain bundle [261, 262]. In addition to serotonergic transmission, IL-DBS is also modulated by adenosinergic and glutamatergic neurotransmission as pre-treatment with selective antagonists attenuates the antidepressant effect of treatment [257, 263]. Furthermore, IL-DBS induces beneficial neuroplasticity, such as hippocampal neurogenesis [264, 265], and increased dendrite length [154, 266], with associated increases in BDNF [264, 265, 267,268,269,270].
Post-traumatic stress disorder
The amygdala and IL have been the primary DBS targets for treating PTSD, as hyperactivity of the basolateral amygdala (BLA) is associated with PTSD symptom severity [271]. BLA-DBS has been shown to decrease and normalize local neuronal activation [272, 273] and reverse fear condition-induced changes to synaptic plasticity in the cortical-amygdala connections, suggesting BLA-DBS may disrupt the long-term retention of fear memory [274]. However, it is important to note that the chronic electrical stimulation of the temporal lobes (especially the amygdala) is known to induce seizures, therefore being a well-established model of kindling [275, 276]. IL-DBS was shown to mitigate PTSD-like behaviours while reducing BLA neuronal activity by activating GABAergic interneurons through PFC-BLA projections [100], being an effective and safer target for DBS.
Neurodevelopmental disorders
ASD and Tourette’s syndrome are the most commonly studied neurodevelopmental disorders in preclinical DBS research. In ASD models, IL-DBS restores the abnormal serotonergic transmission and modulates the expression of glutamatergic and GABAergic receptors in the targeted area while improving social deficits, anxiety-like behaviour, and hyperactivity [48]. Fornix-DBS in ASD models shows an antidepressant effect [58] and reduces memory deficits [60, 61] via normalization of the expression of genes related to intellectual disabilities [58] and restoration of hippocampal synchrony, spontaneous excitatory postsynaptic currents, long-term potentiation and feedforward inhibition [59,60,61]. Thalamus-DBS has been shown to improve repetitive behaviours in ASD models by restoring functional connectivity in corticostriatal and corticolimbic circuits and decreasing dopaminergic receptor expression in the striatum [47]. In a Tourette’s syndrome model, however, thalamus-DBS reduced local theta band activity and local field potentials in the striatum [49]. In this model, entopeduncular DBS decreased dopamine concentration and dopamine transporter in the striatum, leading to decreased tic behaviour [50].
Schizophrenia and psychosis
Several targets have been investigated for improving positive symptoms in models of schizophrenia and psychosis. While targeting the hippocampus with DBS restores the dopaminergic activity of the VTA [277], targeting the VTA with DBS leads to increased GABA neurotransmission but not dopaminergic activity [278]. Medial septum-DBS has also been shown to restore dopaminergic transmission while improving serotonergic activity [94, 95] and reducing hippocampal gamma oscillations [20], which leads to attenuated psychotic schizophrenic symptoms. Similarly, thalamic-DBS modulates neural oscillations, alleviating aberrant thalamic oscillatory activity and modulating coherence in thalamocortical networks [279].
Traumatic Brain Injury
In the context of TBI, DBS has been used to address decreased levels of consciousness, deficits in cognitive function, and motor recovery. The hypothalamus is a key region involved with wakefulness and alertness, particularly through orexin neurons of the lateral hypothalamus that have widespread projections throughout the brain [280]. In a weight-drop model of TBI, lateral hypothalamus-DBS promoted consciousness recovery along with increases in adenosine A1 receptor, decreases in GABA receptor, increases in orexin receptor, and decreased low-frequency delta oscillations in the PFC [280]. In addition, brain regions with strong connectivity with the hippocampus, such as the medial septum, have also been targeted, as these regions play a critical role in cognition. DBS of the medial septum was linked to the restoration of hippocampal theta oscillations and improved cognitive functions following TBI [281]. Furthermore, the cerebellum has been targeted for its role in influencing motor function through extensive thalamocortical projections, and DBS of the cerebellum was shown to enhance motor functions alongside the elevation of perilesional neuronal activity and suppression of neuroinflammation and apoptotic markers [45].
Limitations of DBS studies with rodent models
A few limitations need to be taken into account when considering the direct translation of data from rodent models to the clinical setting. Although experimental models have provided much value to our understanding of the underlying mechanisms and effects of DBS, it remains important to consider that these models do not fully reflect human disease but rather mimic a series of key symptoms. For instance, DBS of the fornix and lateral hypothalamus has shown promising outcomes in rodent models of AD [54, 111] and obesity [244, 245], respectively. However, the application of these approaches has not been as successful within the clinical population [282, 283], which alludes to the caution that needs to be taken when translating such therapeutic regimens to humans. The high rate of positive behavioural responses observed in these studies should also be interpreted with caution, as there is a tendency in scientific publications to focus on publishing positive results rather than negative ones. Furthermore, the anatomical organization of rodent brains is similar to that of the human brain in many aspects; however, key differences in cortical processing and, therefore, cognitive abilities prevent the direct translation of findings, especially in the context of top-down inhibitory control of motivated behaviours. Also, anatomical differences between rodents and humans in specific clinically relevant brain targets may be impeditive to a translation to rodent models. Lastly, the make of DBS electrodes, the stimulation parameters and stimulation settings (i.e., acute, chronic) used in rodents are highly variable and are typically different from those used in humans [284].
Despite these limitations, rodent studies have contributed substantially to our current knowledge of the mechanisms underlying DBS treatment. Advancements in the field have led to the development of novel stimulation techniques and rodent DBS devices that are fully implantable and/or with wireless stimulators for long-term use in freely moving animals [285]. These applications are only growing as new technologies such as closed-loop circuits [286] and specialized stimulation electrodes [167,168,169] improve the precision of targeting and decrease adverse effects.
Ethical considerations
While DBS is an efficacious surgical treatment for many neurological and psychiatric disorders in adult and pediatric populations, the precise neurobiological mechanism of action of DBS treatment remains elusive. Thus, translational research is needed to advance our understanding of disease processes and treatment mechanisms to develop novel, less invasive and more efficacious therapies. Animal experimentation, however, must be performed under strict ethical guidelines to answer sound scientific questions that cannot be addressed in in-vitro or in-silico models [287,288,289]. The “Three Rs” principle (Reduction, Refinement, and Replacement) sets the ethical standard for in-vivo research. The reduction principle refers to reducing the number of animals used per experiment or study while keeping statistical power, the Refinement principle refers to the improvement of all methods used in research to minimize pain, suffering, distress or lasting harm and improve animal welfare, and the Replacement principle refers to the full or partial replacement of live animals with technologies or alternative approaches [287,288,289].
In clinical settings, distinct ethical considerations must be made when performing DBS trials. Questions on how to provide the best care for vulnerable patients at the late stages of life, especially those with progressive degenerative disorders, must be made to assess if the benefits of treatment are superior to the potential complications [290, 291]. In patients with psychiatric disorders, major concerns arise related to the patient’s capacity to provide informed consent, the possibility of altering behaviour via brain stimulation, as well as the risks and benefits compared to traditional and less invasive treatment methods [292, 293]. Also, DBS for treating psychiatric disorders shares many features with psychosurgeries and, therefore, raises several ethical and legal concerns that must be openly discussed [294]. For the pediatric population, it is crucial to assert the potential risks and benefits of DBS, the optimal time for offering the treatment and the long-term consequences of brain stimulation [295]. Also, it is necessary to discuss the role of the informed assent given by the child in addition to the informed consent signed by the parent/guardian [295]. A bioethical framework to advance ethical discussions regarding pediatric DBS has been proposed and involves the protection of the child’s best interest, the consideration of the developmental context, the creation of strategies for mitigating known and unknown risks, the critical appraisal of the adult literature, and fostering communication and collaboration among practitioners [296]. Finally, there are several concerns related to specific devices’ capacity for detecting neuronal activity and the safe storage of these data [297]. With the advancement of DBS devices, new policies must be developed to maximize benefits and minimize harm to patients.
Conclusion
Though there has been extensive research into the effects of DBS targeted to key brain structures, there remains a dire need for standardized, protocol-based approaches to find optimal stimulation targets and parameters for distinct pathologies. Studies on rodent models have not only shed light on possible mechanisms of action of DBS treatment but also improved our understanding of the underlying disease processes. Models of psychiatric and neurodevelopmental disorders have implicated dysfunctions in the monoaminergic system and in the functional connectivity of the mesocorticolimbic network in the pathophysiology of diseases, and, therefore, modulation of these aspects with DBS resulted in improved behaviour. Similarly, the cellular and molecular complexity of PD has been further explored in rodent models, which are capable of capturing both motor and non-motor symptoms of the disease. In these models, DBS improves symptoms via modulation of the striatal dopaminergic system and suggests that treatment response is associated with dopamine availability. Although there are several limitations in translating findings from preclinical to clinical settings, these studies have shown that direct modulation of neural activity (both cellular and molecular) is among the major mechanisms of action, albeit further research is necessary for a complete understanding of this neuromodulation therapy.
Data availability
All articles included here are available in PubMed, and the complete reference list can be found in the Supplementary References.
References
Lozano AM, Eltahawy H. How does DBS work? Suppl Clin Neurophysiol. 2004;57:733–6.
Gouveia FV, Gidyk DC, Giacobbe P, Ng E, Meng Y, Davidson B, et al. Neuromodulation strategies in post-traumatic stress disorder: from preclinical models to clinical applications. Brain Sci. 2019;9. https://doi.org/10.3390/brainsci9020045.
Elias GJB, Boutet A, Parmar R, Wong EHY, Germann J, Loh A, et al. Neuromodulatory treatments for psychiatric disease: a comprehensive survey of the clinical trial landscape. Brain Stimul. 2021;14:1393–403.
Germann J, Mameli M, Elias GJB, Loh A, Taha A, Gouveia FV, et al. Deep brain stimulation of the habenula: Systematic review of the literature and clinical trial registries. Front Psychiatry. 2021;12:730931.
Gouveia FV, Germann J, Elias GJB, Boutet A, Loh A, Lopez Rios AL, et al. Multi-centre analysis of networks and genes modulated by hypothalamic stimulation in patients with aggressive behaviours. Elife. 2023;12. https://doi.org/10.7554/eLife.84566.
Lozano AM, Lipsman N. Probing and regulating dysfunctional circuits using deep brain stimulation. Neuron. 2013;77:406–24.
Lozano AM, Lipsman N, Bergman H, Brown P, Chabardes S, Chang JW, et al. Deep brain stimulation: current challenges and future directions. Nat Rev Neurol. 2019;15:148–60.
Coubes P, Cif L, El Fertit H, Hemm S, Vayssiere N, Serrat S, et al. Electrical stimulation of the globus pallidus internus in patients with primary generalized dystonia: long-term results. J Neurosurg. 2004;101:189–94.
Visser-Vandewalle V, Temel Y, Boon P, Vreeling F, Colle H, Hoogland G, et al. Chronic bilateral thalamic stimulation: a new therapeutic approach in intractable Tourette syndrome. Report of three cases. J Neurosurg. 2003;99:1094–1100.
Kim SH, Lim SC, Kim J, Son B-C, Lee KJ, Shon Y-M. Long-term follow-up of anterior thalamic deep brain stimulation in epilepsy: a 11-year, single center experience. Seizure. 2017;52:154–61.
Graat I, Mocking R, Figee M, Vulink N, de Koning P, Ooms P, et al. Long-term outcome of deep brain stimulation of the ventral part of the anterior limb of the internal capsule in a cohort of 50 patients with treatment-refractory obsessive-compulsive disorder. Biol Psychiatry. 2021;90:714–20.
Greenberg BD, Malone DA, Friehs GM, Rezai AR, Kubu CS, Malloy PF, et al. Three-year outcomes in deep brain stimulation for highly resistant obsessive-compulsive disorder. Neuropsychopharmacology. 2006;31:2384–93.
Bewernick BH, Kayser S, Sturm V, Schlaepfer TE. Long-term effects of nucleus accumbens deep brain stimulation in treatment-resistant depression: evidence for sustained efficacy. Neuropsychopharmacology. 2012;37:1975–85.
Chen L, Li N, Ge S, Lozano AM, Lee DJ, Yang C, et al. Long-term results after deep brain stimulation of nucleus accumbens and the anterior limb of the internal capsule for preventing heroin relapse: an open-label pilot study. Brain Stimul. 2019;12:175–83.
Müller UJ, Sturm V, Voges J, Heinze H-J, Galazky I, Heldmann M, et al. Successful treatment of chronic resistant alcoholism by deep brain stimulation of nucleus accumbens: first experience with three cases. Pharmacopsychiatry. 2009;42:288–91.
Campos ACP, Pople C, Silk E, Surendrakumar S, Rabelo TK, Meng Y, et al. Neurochemical mechanisms of deep brain stimulation for depression in animal models. Eur Neuropsychopharmacol. 2023;68:11–26.
Gouveia FV, Diwan M, Martinez RCR, Giacobbe P, Lipsman N, Hamani C. Reduction of aggressive behaviour following hypothalamic deep brain stimulation: involvement of 5-HT and testosterone. Neurobiol Dis. 2023;183:106179.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Rev Esp Cardiol. 2021;74:790–9.
American Psychiatric Association. Diagnostic and statistical manual of mental disorders (DSM-5 (R)). 5th ed. Arlington, TX: American Psychiatric Association Publishing; 2013.
Ma J, Leung LS. Deep brain stimulation of the medial septum or nucleus accumbens alleviates psychosis-relevant behavior in ketamine-treated rats. Behav Brain Res. 2014;266:174–82.
Sesia T, Bulthuis V, Tan S, Lim LW, Vlamings R, Blokland A, et al. Deep brain stimulation of the nucleus accumbens shell increases impulsive behavior and tissue levels of dopamine and serotonin. Exp Neurol. 2010;225:302–9.
Moers-Hornikx VMP, Sesia T, Basar K, Lim LW, Hoogland G, Steinbusch HWM, et al. Cerebellar nuclei are involved in impulsive behaviour. Behav Brain Res. 2009;203:256–63.
Adams WK, Vonder Haar C, Tremblay M, Cocker PJ, Silveira MM, Kaur S, et al. Deep-brain stimulation of the subthalamic nucleus selectively decreases risky choice in risk-preferring rats. eNeuro. 2017;4. https://doi.org/10.1523/ENEURO.0094-17.2017.
Rouaud T, Lardeux S, Panayotis N, Paleressompoulle D, Cador M, Baunez C. Reducing the desire for cocaine with subthalamic nucleus deep brain stimulation. Proc Natl Acad Sci USA. 2010;107:1196–1200.
Hamilton J, Lee J, Canales JJ. Chronic unilateral stimulation of the nucleus accumbens at high or low frequencies attenuates relapse to cocaine seeking in an animal model. Brain Stimul. 2015;8:57–63.
Knapp CM, Tozier L, Pak A, Ciraulo DA, Kornetsky C. Deep brain stimulation of the nucleus accumbens reduces ethanol consumption in rats. Pharm Biochem Behav. 2009;92:474–9.
Wang M, Jia L, Wu X, Sun Z, Xu Z, Kong C, et al. Deep brain stimulation improves motor function in rats with spinal cord injury by increasing synaptic plasticity. World Neurosurg. 2020;140:e294–e303.
Bachmann LC, Matis A, Lindau NT, Felder P, Gullo M, Schwab ME. Deep brain stimulation of the midbrain locomotor region improves paretic hindlimb function after spinal cord injury in rats. Sci Transl Med. 2013;5:208ra146.
Jackson J, Young CK, Hu B, Bland BH. High frequency stimulation of the posterior hypothalamic nucleus restores movement and reinstates hippocampal-striatal theta coherence following haloperidol-induced catalepsy. Exp Neurol. 2008;213:210–9.
Temel Y, Visser-Vandewalle V, Kaplan S, Kozan R, Daemen MARC, Blokland A, et al. Protection of nigral cell death by bilateral subthalamic nucleus stimulation. Brain Res. 2006;1120:100–5.
Temel Y, Visser-Vandewalle V, Aendekerk B, Rutten B, Tan S, Scholtissen B, et al. Acute and separate modulation of motor and cognitive performance in Parkinsonian rats by bilateral stimulation of the subthalamic nucleus. Exp Neurol. 2005;193:43–52.
McConnell GC, So RQ, Grill WM. Failure to suppress low-frequency neuronal oscillatory activity underlies the reduced effectiveness of random patterns of deep brain stimulation. J Neurophysiol. 2016;115:2791–802.
King NO, Anderson CJ, Dorval AD. Deep brain stimulation exacerbates hypokinetic dysarthria in a rat model of Parkinson’s disease. J Neurosci Res. 2016;94:128–38.
Anderson CJ, Sheppard DT, Huynh R, Anderson DN, Polar CA, Dorval AD. Subthalamic deep brain stimulation reduces pathological information transmission to the thalamus in a rat model of parkinsonism. Front Neural Circuits. 2015;9:31.
Summerson SR, Aazhang B, Kemere CT. Characterizing motor and cognitive effects associated with deep brain stimulation in the GPi of hemi-Parkinsonian rats. IEEE Trans Neural Syst Rehabil Eng. 2014;22:1218–27.
Dorval AD, Grill WM. Deep brain stimulation of the subthalamic nucleus reestablishes neuronal information transmission in the 6-OHDA rat model of parkinsonism. J Neurophysiol. 2014;111:1949–59.
McConnell GC, So RQ, Hilliard JD, Lopomo P, Grill WM. Effective deep brain stimulation suppresses low-frequency network oscillations in the basal ganglia by regularizing neural firing patterns. J Neurosci. 2012;32:15657–68.
So RQ, McConnell GC, August AT, Grill WM. Characterizing effects of subthalamic nucleus deep brain stimulation on methamphetamine-induced circling behavior in hemi-Parkinsonian rats. IEEE Trans Neural Syst Rehabil Eng. 2012;20:626–35.
Brown AR, Antle MC, Hu B, Teskey GC. High frequency stimulation of the subthalamic nucleus acutely rescues motor deficits and neocortical movement representations following 6-hydroxydopamine administration in rats. Exp Neurol. 2011;231:82–90.
Young CK, Koke SJ, Kiss ZH, Bland BH. Deep brain stimulation of the posterior hypothalamic nucleus reverses akinesia in bilaterally 6-hydroxydopamine-lesioned rats. Neuroscience. 2009;162:1–4.
Apetz N, Kordys E, Simon M, Mang B, Aswendt M, Wiedermann D, et al. Effects of subthalamic deep brain stimulation on striatal metabolic connectivity in a rat hemiparkinsonian model. Dis Model Mech. 2019;12. https://doi.org/10.1242/dmm.039065.
So RQ, McConnell GC, Grill WM. Frequency-dependent, transient effects of subthalamic nucleus deep brain stimulation on methamphetamine-induced circling and neuronal activity in the hemiparkinsonian rat. Behav Brain Res. 2017;320:119–27.
Polar CA, Gupta R, Lehmkuhle MJ, Dorval AD. Correlation between cortical beta power and gait speed is suppressed in a parkinsonian model, but restored by therapeutic deep brain stimulation. Neurobiol Dis. 2018;117:137–48.
Anderson C, Sheppard D, Dorval AD. Parkinsonism and subthalamic deep brain stimulation dysregulate behavioral motivation in a rodent model. Brain Res. 2020;1736:146776.
Chan HH, Wathen CA, Mathews ND, Hogue O, Modic JP, Kundalia R, et al. Lateral cerebellar nucleus stimulation promotes motor recovery and suppresses neuroinflammation in a fluid percussion injury rodent model. Brain Stimul. 2018;11:1356–67.
Bonizzato M, James ND, Pidpruzhnykova G, Pavlova N, Shkorbatova P, Baud L, et al. Multi-pronged neuromodulation intervention engages the residual motor circuitry to facilitate walking in a rat model of spinal cord injury. Nat Commun. 2021;12:1925.
Lin T-C, Lo Y-C, Lin H-C, Li S-J, Lin S-H, Wu H-F, et al. MR imaging central thalamic deep brain stimulation restored autistic-like social deficits in the rat. Brain Stimul. 2019;12:1410–20.
Wu H-F, Chen Y-J, Chu M-C, Hsu Y-T, Lu T-Y, Chen I-T, et al. Deep brain stimulation modified autism-like deficits via the serotonin system in a valproic acid-induced rat Model. Int J Mol Sci. 2018;19. https://doi.org/10.3390/ijms19092840.
Elle T, Alam M, Voigt C, Krauss JK, John N, Schwabe K. Deep brain stimulation of the thalamic centromedian-parafascicular nucleus improves behavioural and neuronal traits in a rat model of Tourette. Behav Brain Res. 2020;378:112251.
Zhao M, Wang X, Deng J, Guan Y, Zhou J, Li T, et al. Globus pallidus internus electric high-frequency stimulation modulates dopaminergic activity in the striatum of a rat model of tourette syndrome. World Neurosurg. 2019;127:e881–e887.
Guo H, Zhang H, Kuang Y, Wang C, Jing X, Gu J, et al. Electrical stimulation of the substantia nigra pars reticulata (SNr) suppresses chemically induced neocortical seizures in rats. J Mol Neurosci. 2014;53:546–52.
Saillet S, Gharbi S, Charvet G, Deransart C, Guillemaud R, Depaulis A, et al. Neural adaptation to responsive stimulation: a comparison of auditory and deep brain stimulation in a rat model of absence epilepsy. Brain Stimul. 2013;6:241–7.
Blik V. Electric stimulation of the tuberomamillary nucleus affects epileptic activity and sleep-wake cycle in a genetic absence epilepsy model. Epilepsy Res. 2015;109:119–25.
Leplus A, Lauritzen I, Melon C, Kerkerian-Le Goff L, Fontaine D, Checler F. Chronic fornix deep brain stimulation in a transgenic Alzheimer’s rat model reduces amyloid burden, inflammation, and neuronal loss. Brain Struct Funct. 2019;224:363–72.
Koulousakis P, van den Hove D, Visser-Vandewalle V, Sesia T. Cognitive improvements after intermittent deep brain stimulation of the nucleus basalis of meynert in a transgenic rat model for alzheimer’s disease: a preliminary approach. J Alzheimers Dis. 2020;73:461–6.
Temel Y, Cao C, Vlamings R, Blokland A, Ozen H, Steinbusch HWM, et al. Motor and cognitive improvement by deep brain stimulation in a transgenic rat model of Huntington’s disease. Neurosci Lett. 2006;406:138–41.
Chang AD, Berges VA, Chung SJ, Fridman GY, Baraban JM, Reti IM. High-frequency stimulation at the subthalamic nucleus suppresses excessive self-grooming in autism-like mouse models. Neuropsychopharmacology. 2016;41:1813–21.
Pohodich AE, Yalamanchili H, Raman AT, Wan Y-W, Gundry M, Hao S, et al. Forniceal deep brain stimulation induces gene expression and splicing changes that promote neurogenesis and plasticity. Elife 2018;7. https://doi.org/10.7554/eLife.34031.
Lu H, Ash RT, He L, Kee SE, Wang W, Yu D, et al. Loss and gain of MeCP2 cause similar hippocampal circuit dysfunction that is rescued by deep brain stimulation in a Rett syndrome mouse model. Neuron. 2016;91:739–47.
Hao S, Tang B, Wu Z, Ure K, Sun Y, Tao H, et al. Forniceal deep brain stimulation rescues hippocampal memory in Rett syndrome mice. Nature. 2015;526:430–4.
Hao S, Wang Q, Tang B, Wu Z, Yang T, Tang J. CDKL5 deficiency augments inhibitory input into the dentate gyrus that can be reversed by deep brain stimulation. J Neurosci. 2021;41:9031–46.
Pinhal CM, van den Boom BJG, Santana-Kragelund F, Fellinger L, Bech P, Hamelink R, et al. Differential effects of deep brain stimulation of the internal capsule and the striatum on excessive grooming in Sapap3 mutant mice. Biol Psychiatry. 2018;84:917–25.
Rogers AA, Aiani LM, Blanpain LT, Yuxian S, Moore R, Willie JT. Deep brain stimulation of hypothalamus for narcolepsy-cataplexy in mice. Brain Stimul. 2020;13:1305–16.
Tsai S-T, Chen L-J, Wang Y-J, Chen S-Y, Tseng G-F. Rostral intralaminar thalamic deep brain stimulation triggered cortical and hippocampal structural plasticity and enhanced spatial memory. Stereotact Funct Neurosurg. 2016;94:108–17.
Lai H-Y, Younce JR, Albaugh DL, Kao Y-CJ, Shih Y-YI. Functional MRI reveals frequency-dependent responses during deep brain stimulation at the subthalamic nucleus or internal globus pallidus. Neuroimage. 2014;84:11–18.
Huang C, Chu H, Ma Y, Zhou Z, Dai C, Huang X, et al. The neuroprotective effect of deep brain stimulation at nucleus basalis of Meynert in transgenic mice with Alzheimer’s disease. Brain Stimul. 2019;12:161–74.
Degoulet M, Tiran-Cappello A, Combrisson E, Baunez C, Pelloux Y. Subthalamic low-frequency oscillations predict vulnerability to cocaine addiction. Proc Natl Acad Sci USA. 2021;118. https://doi.org/10.1073/pnas.2024121118.
Rummel J, Voget M, Hadar R, Ewing S, Sohr R, Klein J, et al. Testing different paradigms to optimize antidepressant deep brain stimulation in different rat models of depression. J Psychiatr Res. 2016;81:36–45.
Creed MC, Hamani C, Nobrega JN. Effects of repeated deep brain stimulation on depressive- and anxiety-like behavior in rats: comparing entopeduncular and subthalamic nuclei. Brain Stimul. 2013;6:506–14.
Usui N, Maesawa S, Kajita Y, Endo O, Takebayashi S, Yoshida J. Suppression of secondary generalization of limbic seizures by stimulation of subthalamic nucleus in rats. J Neurosurg. 2005;102:1122–9.
Yu W, Walling I, Smith AB, Ramirez-Zamora A, Pilitsis JG, Shin DS. Deep brain stimulation of the ventral pallidum attenuates epileptiform activity and seizing behavior in pilocarpine-treated rats. Brain Stimul. 2016;9:285–95.
Klein J, Hadar R, Götz T, Männer A, Eberhardt C, Baldassarri J, et al. Mapping brain regions in which deep brain stimulation affects schizophrenia-like behavior in two rat models of schizophrenia. Brain Stimul. 2013;6:490–9.
Zhang Q, Wu ZC, Yu J-T, Yu NN, Zhong XL, Tan L. Mode-dependent effect of high-frequency electrical stimulation of the anterior thalamic nucleus on amygdala-kindled seizures in rats. Neuroscience. 2012;217:113–22.
Zhang Q, Wu Z-C, Yu J-T, Zhong X-L, Xing Y-Y, Tian Y, et al. Anticonvulsant effect of unilateral anterior thalamic high frequency electrical stimulation on amygdala-kindled seizures in rat. Brain Res Bull. 2012;87:221–6.
Zhu G, Meng D, Chen Y, Du T, Liu Y, Liu D, et al. Anterior nucleus of thalamus stimulation inhibited abnormal mossy fiber sprouting in kainic acid-induced epileptic rats. Brain Res. 2018;1701:28–35.
Chen Y-C, Zhu G-Y, Wang X, Shi L, Du T-T, Liu D-F, et al. Anterior thalamic nuclei deep brain stimulation reduces disruption of the blood-brain barrier, albumin extravasation, inflammation and apoptosis in kainic acid-induced epileptic rats. Neurol Res. 2017;39:1103–13.
Chen Y-C, Shi L, Zhu G-Y, Wang X, Liu D-F, Liu Y-Y, et al. Effects of anterior thalamic nuclei deep brain stimulation on neurogenesis in epileptic and healthy rats. Brain Res. 2017;1672:65–72.
Chen Y-C, Zhu G-Y, Wang X, Shi L, Jiang Y, Zhang X, et al. Deep brain stimulation of the anterior nucleus of the thalamus reverses the gene expression of cytokines and their receptors as well as neuronal degeneration in epileptic rats. Brain Res. 2017;1657:304–11.
Meng D-W, Liu H-G, Yang A-C, Zhang K, Zhang J-G. Stimulation of anterior thalamic nuclei protects against seizures and neuronal apoptosis in hippocampal CA3 region of kainic acid-induced epileptic rats. Chin Med J. 2016;129:960–6.
Tang W, He X, Feng L, Liu D, Yang Z, Zhang J, et al. The role of hippocampal neurogenesis in ANT-DBS for LiCl-pilocarpine-induced epileptic rats. Stereotact Funct Neurosurg. 2021;99:55–64.
Covolan L, de Almeida A-CG, Amorim B, Cavarsan C, Miranda MF, Aarão MC, et al. Effects of anterior thalamic nucleus deep brain stimulation in chronic epileptic rats. PLoS ONE. 2014;9:e97618.
Tseng H-T, Hsiao Y-T, Yi P-L, Chang F-C. Deep brain stimulation increases seizure threshold by altering REM sleep and delta powers during NREM sleep. Front Neurol. 2020;11:752.
Ziai WC, Sherman DL, Bhardwaj A, Zhang N, Keyl PM, Mirski MA. Target-specific catecholamine elevation induced by anticonvulsant thalamic deep brain stimulation. Epilepsia. 2005;46:878–88.
Reyes-Garcés N, Diwan M, Boyacı E, Gómez-Ríos GA, Bojko B, Nobrega JN, et al. In vivo brain sampling using a microextraction probe reveals metabolic changes in rodents after deep brain stimulation. Anal Chem. 2019;91:9875–84.
Volle J, Bregman T, Scott B, Diwan M, Raymond R, Fletcher PJ, et al. Deep brain stimulation and fluoxetine exert different long-term changes in the serotonergic system. Neuropharmacology. 2018;135:63–72.
Lehto LJ, Filip P, Laakso H, Sierra A, Slopsema JP, Johnson MD, et al. Tuning neuromodulation effects by orientation selective deep brain stimulation in the rat medial frontal cortex. Front Neurosci. 2018;12:899.
Winter C, Bregman T, Voget M, Raymond R, Hadar R, Nobrega JN, et al. Acute high frequency stimulation of the prefrontal cortex or nucleus accumbens does not increase hippocampal neurogenesis in rats. J Psychiatr Res. 2015;68:27–29.
Parthoens J, Verhaeghe J, Stroobants S, Staelens S. Deep brain stimulation of the prelimbic medial prefrontal cortex: quantification of the effect on glucose metabolism in the rat brain using [(18) F]FDG microPET. Mol Imaging Biol. 2014;16:838–45.
Casquero-Veiga M, García-García D, Desco M, Soto-Montenegro ML. Understanding deep brain stimulation: metabolic consequences of the electrode insertional effect. Biomed Res Int. 2018;2018:8560232.
Casquero-Veiga M, Hadar R, Pascau J, Winter C, Desco M, Soto-Montenegro ML. Response to deep brain stimulation in three brain targets with implications in mental disorders: a PET study in rats. PLoS ONE. 2016;11:e0168689.
Vassoler FM, White SL, Hopkins TJ, Guercio LA, Espallergues J, Berton O, et al. Deep brain stimulation of the nucleus accumbens shell attenuates cocaine reinstatement through local and antidromic activation. J Neurosci. 2013;33:14446–54.
Guercio LA, Wimmer ME, Schmidt HD, Swinford-Jackson SE, Pierce RC, Vassoler FM. Deep brain stimulation of the infralimbic cortex attenuates cocaine priming-induced reinstatement of drug seeking. Brain Res. 2020;1746:147011.
Fakhrieh-Asl G, Sadr SS, Karimian SM, Riahi E. Deep brain stimulation of the orbitofrontal cortex prevents the development and reinstatement of morphine place preference. Addict Biol. 2020;25:e12780.
Hadar R, Bikovski L, Soto-Montenegro ML, Schimke J, Maier P, Ewing S, et al. Early neuromodulation prevents the development of brain and behavioral abnormalities in a rodent model of schizophrenia. Mol Psychiatry. 2018;23:943–51.
Bikovsky L, Hadar R, Soto-Montenegro ML, Klein J, Weiner I, Desco M, et al. Deep brain stimulation improves behavior and modulates neural circuits in a rodent model of schizophrenia. Exp Neurol. 2016;283:142–50.
Tan SZK, Neoh J, Lawrence AJ, Wu EX, Lim LW. Prelimbic cortical stimulation improves spatial memory through distinct patterns of hippocampal gene expression in aged rats. Neurotherapeutics. 2020;17:2054–68.
Klanker M, Post G, Joosten R, Feenstra M, Denys D. Deep brain stimulation in the lateral orbitofrontal cortex impairs spatial reversal learning. Behav Brain Res. 2013;245:7–12.
Bhaskar Y, Lim LW, Mitra R. Enriched environment facilitates anxiolytic efficacy driven by deep-brain stimulation of medial prefrontal cortex. Front Behav Neurosci. 2018;12:204.
Sarica C, Ozkan M, Hacioglu Bay H, Sehirli U, Onat F, Ziyal MI. Prelimbic cortex deep brain stimulation reduces binge size in a chronic binge eating rat model. Stereotact Funct Neurosurg. 2018;96:33–39.
Reznikov R, Bambico FR, Diwan M, Raymond RJ, Nashed MG, Nobrega JN, et al. Prefrontal cortex deep brain stimulation improves fear and anxiety-like behavior and reduces basolateral amygdala activity in a preclinical model of posttraumatic stress disorder. Neuropsychopharmacology. 2018;43:1099–106.
Song N, Du J, Gao Y, Yang S. Epitranscriptome of the ventral tegmental area in a deep brain-stimulated chronic unpredictable mild stress mouse model. Transl Neurosci. 2020;11:402–18.
Schmuckermair C, Gaburro S, Sah A, Landgraf R, Sartori SB, Singewald N. Behavioral and neurobiological effects of deep brain stimulation in a mouse model of high anxiety- and depression-like behavior. Neuropsychopharmacology. 2013;38:1234–44.
Whittle N, Schmuckermair C, Gunduz Cinar O, Hauschild M, Ferraguti F, Holmes A, et al. Deep brain stimulation, histone deacetylase inhibitors and glutamatergic drugs rescue resistance to fear extinction in a genetic mouse model. Neuropharmacology. 2013;64:414–23.
Halpern CH, Tekriwal A, Santollo J, Keating JG, Wolf JA, Daniels D, et al. Amelioration of binge eating by nucleus accumbens shell deep brain stimulation in mice involves D2 receptor modulation. J Neurosci. 2013;33:7122–9.
Creed M, Pascoli VJ, Lüscher C. Addiction therapy. Refining deep brain stimulation to emulate optogenetic treatment of synaptic pathology. Science. 2015;347:659–64.
Ho AL, Feng AY, Barbosa DAN, Wu H, Smith ML, Malenka RC, et al. Accumbens coordinated reset stimulation in mice exhibits ameliorating aftereffects on binge alcohol drinking. Brain Stimul. 2021;14:330–4.
Visanji NP, Kamali Sarvestani I, Creed MC, Shams Shoaei Z, Nobrega JN, Hamani C, et al. Deep brain stimulation of the subthalamic nucleus preferentially alters the translational profile of striatopallidal neurons in an animal model of Parkinson’s disease. Front Cell Neurosci. 2015;9:221.
Schor JS, Gonzalez Montalvo I, Spratt PWE, Brakaj RJ, Stansil JA, Twedell EL, et al. Therapeutic deep brain stimulation disrupts movement-related subthalamic nucleus activity in parkinsonian mice. Elife 2022;11. https://doi.org/10.7554/eLife.75253.
Alosaimi F, Temel Y, Hescham S, Witzig VS, Almasabi F, Tan SKH, et al. High-frequency stimulation of the subthalamic nucleus induces a sustained inhibition of serotonergic system via loss of cell phenotype. Sci Rep. 2022;12:14011.
Wang X, Hu W-H, Zhang K, Zhou J-J, Liu D-F, Zhang M-Y, et al. Acute fornix deep brain stimulation improves hippocampal glucose metabolism in aged mice. Chin Med J. 2018;131:594–9.
Gallino D, Devenyi GA, Germann J, Guma E, Anastassiadis C, Chakravarty MM. Longitudinal assessment of the neuroanatomical consequences of deep brain stimulation: Application of fornical DBS in an Alzheimer’s mouse model. Brain Res. 2019;1715:213–23.
Liu H-Y, Jin J, Tang J-S, Sun W-X, Jia H, Yang X-P, et al. Chronic deep brain stimulation in the rat nucleus accumbens and its effect on morphine reinforcement. Addict Biol. 2008;13:40–46.
Shih Y-YI, Yash TV, Rogers B, Duong TQ. FMRI of deep brain stimulation at the rat ventral posteromedial thalamus. Brain Stimul. 2014;7:190–3.
Lindemann C, Krauss JK, Schwabe K. Deep brain stimulation of the subthalamic nucleus in the 6-hydroxydopamine rat model of Parkinson’s disease: effects on sensorimotor gating. Behav Brain Res. 2012;230:243–50.
Faust K, Vajkoczy P, Xi B, Harnack D. The effects of deep brain stimulation of the subthalamic nucleus on vascular endothelial growth factor, brain-derived neurotrophic factor, and glial cell line-derived neurotrophic factor in a rat model of Parkinson’s disease. Stereotact Funct Neurosurg. 2021;99:256–66.
Gut NK, Winn P. Deep brain stimulation of different pedunculopontine targets in a novel rodent model of parkinsonism. J Neurosci. 2015;35:4792–803.
Roet M, Pol S, Schaper FLWVJ, Hoogland G, Jahanshahi A, Temel Y. Severe seizures as a side effect of deep brain stimulation in the dorsal peduncular cortex in a rat model of depression. Epilepsy Behav. 2019;92:269–75.
Wu D-C, Zhu-Ge Z-B, Yu C-Y, Fang Q, Wang S, Jin C-L, et al. Low-frequency stimulation of the tuberomammillary nucleus facilitates electrical amygdaloid-kindling acquisition in Sprague-Dawley rats. Neurobiol Dis. 2008;32:151–6.
Nishida N, Huang Z-L, Mikuni N, Miura Y, Urade Y, Hashimoto N. Deep brain stimulation of the posterior hypothalamus activates the histaminergic system to exert antiepileptic effect in rat pentylenetetrazol model. Exp Neurol. 2007;205:132–44.
Sprengers M, Raedt R, Larsen LE, Delbeke J, Wadman WJ, Boon P, et al. Deep brain stimulation reduces evoked potentials with a dual time course in freely moving rats: Potential neurophysiological basis for intermittent as an alternative to continuous stimulation. Epilepsia. 2020;61:903–13.
da Silva JC, Scorza FA, Nejm MB, Cavalheiro EA, Cukiert A. c-FOS expression after hippocampal deep brain stimulation in normal rats. Neuromodulation. 2014;17:213–7.
da Silva JC, Amorim H, Scorza FA, Cavalheiro EA, Cukiert A. Brain electrical activity after acute hippocampal stimulation in awake rats. Neuromodulation. 2013;16:100–4.
Rodriguez-Romaguera J, Do Monte FHM, Quirk GJ. Deep brain stimulation of the ventral striatum enhances extinction of conditioned fear. Proc Natl Acad Sci USA. 2012;109:8764–9.
Oza CS, Brocker DT, Behrend CE, Grill WM. Patterned low-frequency deep brain stimulation induces motor deficits and modulates cortex-basal ganglia neural activity in healthy rats. J Neurophysiol. 2018;120:2410–22.
Bambico FR, Comai S, Diwan M, Hasan SMN, Conway JD, Darvish-Ghane S, et al. High frequency stimulation of the anterior vermis modulates behavioural response to chronic stress: involvement of the prefrontal cortex and dorsal raphe? Neurobiol Dis. 2018;116:166–78.
Kim Y, McGee S, Czeczor JK, Walker AJ, Kale RP, Kouzani AZ, et al. Nucleus accumbens deep-brain stimulation efficacy in ACTH-pretreated rats: alterations in mitochondrial function relate to antidepressant-like effects. Transl Psychiatry. 2016;6:e842.
Furlanetti LL, Coenen VA, Döbrössy MD. Ventral tegmental area dopaminergic lesion-induced depressive phenotype in the rat is reversed by deep brain stimulation of the medial forebrain bundle. Behav Brain Res. 2016;299:132–40.
Hamani C, Dubiela FP, Soares JCK, Shin D, Bittencourt S, Covolan L, et al. Anterior thalamus deep brain stimulation at high current impairs memory in rats. Exp Neurol. 2010;225:154–62.
Baker M, Hong S-I, Kang S, Choi D-S. Rodent models for psychiatric disorders: problems and promises. Lab Anim Res. 2020;36:9.
Richtand NM, Harvey BH, Hoffman KL. Editorial: animal models in psychiatry: translating animal behavior to an improved understanding and treatment of psychiatric disorders. Front Psychiatry. 2022;13:876155.
Nestler EJ, Hyman SE. Animal models of neuropsychiatric disorders. Nat Neurosci. 2010;13:1161–9.
Ungerstedt U. 6-Hydroxy-dopamine induced degeneration of central monoamine neurons. Eur J Pharm. 1968;5:107–10.
Simola N, Morelli M, Carta AR. The 6-hydroxydopamine model of Parkinson’s disease. Neurotox Res. 2007;11:151–67.
Blandini F, Levandis G, Bazzini E, Nappi G, Armentero M-T. Time-course of nigrostriatal damage, basal ganglia metabolic changes and behavioural alterations following intrastriatal injection of 6-hydroxydopamine in the rat: new clues from an old model. Eur J Neurosci. 2007;25:397–405.
Ashkan K, Rogers P, Bergman H, Ughratdar I. Insights into the mechanisms of deep brain stimulation. Nat Rev Neurol. 2017;13:548–54.
Miterko LN, Lin T, Zhou J, van der Heijden ME, Beckinghausen J, White JJ, et al. Neuromodulation of the cerebellum rescues movement in a mouse model of ataxia. Nat Commun. 2021;12:1295.
Kumar G, Asthana P, Yung WH, Kwan KM, Tin C, Ma CHE. Deep brain stimulation of the interposed nucleus reverses motor deficits and stimulates production of anti-inflammatory cytokines in Ataxia mice. Mol Neurobiol. 2022;59:4578–92.
Tsai S-T, Chen S-Y, Lin S-Z, Tseng G-F. Rostral intralaminar thalamic deep brain stimulation ameliorates memory deficits and dendritic regression in β-amyloid-infused rats. Brain Struct Funct. 2020;225:751–61.
Hescham S, Lim LW, Jahanshahi A, Steinbusch HWM, Prickaerts J, Blokland A, et al. Deep brain stimulation of the forniceal area enhances memory functions in experimental dementia: the role of stimulation parameters. Brain Stimul. 2013;6:72–77.
Hescham S, Jahanshahi A, Meriaux C, Lim LW, Blokland A, Temel Y. Behavioral effects of deep brain stimulation of different areas of the Papez circuit on memory- and anxiety-related functions. Behav Brain Res. 2015;292:353–60.
Zhang C, Hu W-H, Wu D-L, Zhang K, Zhang J-G. Behavioral effects of deep brain stimulation of the anterior nucleus of thalamus, entorhinal cortex and fornix in a rat model of Alzheimer’s disease. Chin Med J. 2015;128:1190–5.
Jeong DU, Lee JE, Lee SE, Chang WS, Kim SJ, Chang JW. Improvements in memory after medial septum stimulation are associated with changes in hippocampal cholinergic activity and neurogenesis. Biomed Res Int. 2014;2014:568587.
Akwa Y, Di Malta C, Zallo F, Gondard E, Lunati A, Diaz-de-Grenu LZ, et al. Stimulation of synaptic activity promotes TFEB-mediated clearance of pathological MAPT/Tau in cellular and mouse models of tauopathies. Autophagy. 2023;19:660–77.
Mann A, Gondard E, Tampellini D, Milsted JAT, Marillac D, Hamani C, et al. Chronic deep brain stimulation in an Alzheimer’s disease mouse model enhances memory and reduces pathological hallmarks. Brain Stimul. 2018;11:435–44.
Arrieta-Cruz I, Pavlides C, Pasinetti GM. Deep brain stimulation in midline thalamic region facilitates synaptic transmission and short term memory in a mouse model of Alzheimer’s disease. Transl Neurosci. 2010;1:188–94.
Xia F, Yiu A, Stone SSD, Oh S, Lozano AM, Josselyn SA, et al. Entorhinal cortical deep brain stimulation rescues memory deficits in both Young and old mice genetically engineered to model Alzheimer’s disease. Neuropsychopharmacology. 2017;42:2493–503.
Leite JP, Garcia-Cairasco N, Cavalheiro EA. New insights from the use of pilocarpine and kainate models. Epilepsy Res. 2002;50:93–103.
French JA, Williamson PD, Thadani VM, Darcey TM, Mattson RH, Spencer SS, et al. Characteristics of medial temporal lobe epilepsy: I. Results of history and physical examination. Ann Neurol. 1993;34:774–80.
Curia G, Longo D, Biagini G, Jones RSG, Avoli M. The pilocarpine model of temporal lobe epilepsy. J Neurosci Methods. 2008;172:143–57.
Lévesque M, Avoli M. The kainic acid model of temporal lobe epilepsy. Neurosci Biobehav Rev. 2013;37:2887–99.
Kandratavicius L, Balista PA, Lopes-Aguiar C, Ruggiero RN, Umeoka EH, Garcia-Cairasco N, et al. Animal models of epilepsy: use and limitations. Neuropsychiatr Dis Treat. 2014;10:1693–705.
Commons KG, Linnros SE. Delayed antidepressant efficacy and the desensitization hypothesis. ACS Chem Neurosci. 2019;10:3048–52.
Becker M, Pinhasov A, Ornoy A. Animal models of depression: what can they teach us about the human disease? Diagnostics (Basel). 2021;11. https://doi.org/10.3390/diagnostics11010123.
Falowski SM, Sharan A, Reyes BAS, Sikkema C, Szot P, Van Bockstaele EJ. An evaluation of neuroplasticity and behavior after deep brain stimulation of the nucleus accumbens in an animal model of depression. Neurosurgery. 2011;69:1281–90.
Meng H, Wang Y, Huang M, Lin W, Wang S, Zhang B. Chronic deep brain stimulation of the lateral habenula nucleus in a rat model of depression. Brain Res. 2011;1422:32–38.
Friedman A, Lax E, Abraham L, Tischler H, Yadid G. Abnormality of VTA local field potential in an animal model of depression was restored by patterned DBS treatment. Eur Neuropsychopharmacol. 2012;22:64–71.
Gazit T, Friedman A, Lax E, Samuel M, Zahut R, Katz M, et al. Programmed deep brain stimulation synchronizes VTA gamma band field potential and alleviates depressive-like behavior in rats. Neuropharmacology. 2015;91:135–41.
Nicolini C, Fahnestock M. The valproic acid-induced rodent model of autism. Exp Neurol. 2018;299:217–27.
Pinizzotto CC, Patwardhan A, Aldarondo D, Kritzer MF. Task-specific effects of biological sex and sex hormones on object recognition memories in a 6-hydroxydopamine-lesion model of Parkinson’s disease in adult male and female rats. bioRxiv. 2022. https://doi.org/10.1101/2022.02.15.480556.
Tamás A, Lubics A, Szalontay L, Lengvári I, Reglodi D. Age and gender differences in behavioral and morphological outcome after 6-hydroxydopamine-induced lesion of the substantia nigra in rats. Behav Brain Res. 2005;158:221–9.
Radke AK, Sneddon EA, Monroe SC. Studying sex differences in rodent models of addictive behavior. Curr Protoc. 2021;1:e119.
Spieles-Engemann AL, Collier TJ, Sortwell CE. A functionally relevant and long-term model of deep brain stimulation of the rat subthalamic nucleus: advantages and considerations. Eur J Neurosci. 2010;32:1092–9.
Birdno MJ, Grill WM. Mechanisms of deep brain stimulation in movement disorders as revealed by changes in stimulus frequency. Neurotherapeutics. 2008;5:14–25.
Friedman A, Lax E, Dikshtein Y, Abraham L, Flaumenhaft Y, Sudai E, et al. Electrical stimulation of the lateral habenula produces enduring inhibitory effect on cocaine seeking behavior. Neuropharmacology. 2010;59:452–9.
Martínez-Rivera FJ, Rodriguez-Romaguera J, Lloret-Torres ME, Do Monte FH, Quirk GJ, Barreto-Estrada JL. Bidirectional modulation of extinction of drug seeking by deep brain stimulation of the ventral striatum. Biol Psychiatry. 2016;80:682–90.
McIntyre CC, Grill WM. Finite element analysis of the current-density and electric field generated by metal microelectrodes. Ann Biomed Eng. 2001;29:227–35.
Kolaya E, Firestein BL. Deep brain stimulation: challenges at the tissue-electrode interface and current solutions. Biotechnol Prog. 2021;37:e3179.
Shuang F, Deng H, Shafique AB, Marsh S, Treiman D, Tsakalis K, et al. A first study on nanoporous tungsten recording electrodes for deep brain stimulation. Mater Lett. 2020;260:126885.
Ashok Kumar N, Chauhan M, Kandala SK, Sohn S-M, Sadleir RJ. Development and testing of implanted carbon electrodes for electromagnetic field mapping during neuromodulation. Magn Reson Med. 2020;84:2103–16.
Hejazi M, Tong W, Ibbotson MR, Prawer S, Garrett DJ. Advances in carbon-based microfiber electrodes for neural interfacing. Front Neurosci. 2021;15:658703.
Rizelio V, Szawka RE, Xavier LL, Achaval M, Rigon P, Saur L, et al. Lesion of the subthalamic nucleus reverses motor deficits but not death of nigrostriatal dopaminergic neurons in a rat 6-hydroxydopamine-lesion model of Parkinson’s disease. Braz J Med Biol Res. 2010;43:85–95.
Temel Y, Boothman LJ, Blokland A, Magill PJ, Steinbusch HWM, Visser-Vandewalle V, et al. Inhibition of 5-HT neuron activity and induction of depressive-like behavior by high-frequency stimulation of the subthalamic nucleus. Proc Natl Acad Sci USA. 2007;104:17087–92.
Alam M, Capelle H-H, Schwabe K, Krauss JK. Effect of deep brain stimulation on levodopa-induced dyskinesias and striatal oscillatory local field potentials in a rat model of Parkinson’s disease. Brain Stimul. 2014;7:13–20.
Alam M, Heissler HE, Schwabe K, Krauss JK. Deep brain stimulation of the pedunculopontine tegmental nucleus modulates neuronal hyperactivity and enhanced beta oscillatory activity of the subthalamic nucleus in the rat 6-hydroxydopamine model. Exp Neurol. 2012;233:233–42.
Saryyeva A, Nakamura M, Krauss JK, Schwabe K. c-Fos expression after deep brain stimulation of the pedunculopontine tegmental nucleus in the rat 6-hydroxydopamine Parkinson model. J Chem Neuroanat. 2011;42:210–7.
Rauch F, Schwabe K, Krauss JK. Effect of deep brain stimulation in the pedunculopontine nucleus on motor function in the rat 6-hydroxydopamine Parkinson model. Behav Brain Res. 2010;210:46–53.
Capozzo A, Vitale F, Mattei C, Mazzone P, Scarnati E. Continuous stimulation of the pedunculopontine tegmental nucleus at 40 Hz affects preparative and executive control in a delayed sensorimotor task and reduces rotational movements induced by apomorphine in the 6-OHDA parkinsonian rat. Behav Brain Res. 2014;271:333–42.
Sutton AC, Yu W, Calos ME, Smith AB, Ramirez-Zamora A, Molho ES, et al. Deep brain stimulation of the substantia nigra pars reticulata improves forelimb akinesia in the hemiparkinsonian rat. J Neurophysiol. 2013;109:363–74.
Tan SKH, Hartung H, Schievink S, Sharp T, Temel Y. High-frequency stimulation of the substantia nigra induces serotonin-dependent depression-like behavior in animal models. Biol Psychiatry. 2013;73:e1–3.
Kerrigan JF, Litt B, Fisher RS, Cranstoun S, French JA, Blum DE, et al. Electrical stimulation of the anterior nucleus of the thalamus for the treatment of intractable epilepsy. Epilepsia. 2004;45:346–54.
Chamaa F, Sweidan W, Nahas Z, Saade N, Abou-Kheir W. Thalamic stimulation in awake rats induces neurogenesis in the hippocampal formation. Brain Stimul. 2016;9:101–8.
Chamaa F, Darwish B, Nahas Z, Al-Chaer ED, Saadé NE, Abou-Kheir W. Long-term stimulation of the anteromedial thalamus increases hippocampal neurogenesis and spatial reference memory in adult rats. Behav Brain Res. 2021;402:113114.
Wilden JA, Qing KY, Hauser SR, McBride WJ, Irazoqui PP, Rodd ZA. Reduced ethanol consumption by alcohol-preferring (P) rats following pharmacological silencing and deep brain stimulation of the nucleus accumbens shell. J Neurosurg. 2014;120:997–1005.
Henderson MB, Green AI, Bradford PS, Chau DT, Roberts DW, Leiter JC. Deep brain stimulation of the nucleus accumbens reduces alcohol intake in alcohol-preferring rats. Neurosurg Focus. 2010;29:E12.
Guercio LA, Schmidt HD, Pierce RC. Deep brain stimulation of the nucleus accumbens shell attenuates cue-induced reinstatement of both cocaine and sucrose seeking in rats. Behav Brain Res. 2015;281:125–30.
Vassoler FM, Schmidt HD, Gerard ME, Famous KR, Ciraulo DA, Kornetsky C, et al. Deep brain stimulation of the nucleus accumbens shell attenuates cocaine priming-induced reinstatement of drug seeking in rats. J Neurosci. 2008;28:8735–9.
Chang H, Gao C, Sun K, Xiao L, Li X, Jiang S, et al. Continuous high frequency deep brain stimulation of the rat anterior insula attenuates the relapse post withdrawal and strengthens the extinction of morphine seeking. Front Psychiatry. 2020;11:577155.
Minbashi Moeini M, Sadr SS, Riahi E. Deep brain stimulation of the lateral hypothalamus facilitates extinction and prevents reinstatement of morphine place preference in rats. Neuromodulation. 2021;24:240–7.
Fattahi M, Ashabi G, Karimian SM, Riahi E. Preventing morphine reinforcement with high-frequency deep brain stimulation of the lateral hypothalamic area. Addict Biol. 2019;24:685–95.
Yan N, Chen N, Zhu H, Zhang J, Sim M, Ma Y, et al. High-frequency stimulation of nucleus accumbens changes in dopaminergic reward circuit. PLoS ONE. 2013;8:e79318.
Oterdoom DLM, Lok R, van Beek AP, den Dunnen WFA, Emous M, van Dijk JMC, et al. Deep brain stimulation in the nucleus accumbens for binge eating disorder: a study in rats. Obes Surg. 2020;30:4145–8.
Spieles-Engemann AL, Behbehani MM, Collier TJ, Wohlgenant SL, Steece-Collier K, Paumier K, et al. Stimulation of the rat subthalamic nucleus is neuroprotective following significant nigral dopamine neuron loss. Neurobiol Dis. 2010;39:105–15.
Fauser M, Ricken M, Markert F, Weis N, Schmitt O, Gimsa J, et al. Subthalamic nucleus deep brain stimulation induces sustained neurorestoration in the mesolimbic dopaminergic system in a Parkinson’s disease model. Neurobiol Dis. 2021;156:105404.
Musacchio T, Rebenstorff M, Fluri F, Brotchie JM, Volkmann J, Koprich JB, et al. Subthalamic nucleus deep brain stimulation is neuroprotective in the A53T α-synuclein Parkinson’s disease rat model. Ann Neurol. 2017;81. https://doi.org/10.1002/ana.24947.
Fischer DL, Kemp CJ, Cole-Strauss A, Polinski NK, Paumier KL, Lipton JW, et al. Subthalamic nucleus deep brain stimulation employs trkb signaling for neuroprotection and functional restoration. J Neurosci. 2017;37. https://doi.org/10.1523/JNEUROSCI.2060-16.2017.
Du TT, Chen YC, Lu YQ, Meng FG, Yang H, Zhang JG. Subthalamic nucleus deep brain stimulation protects neurons by activating autophagy via PP2A inactivation in a rat model of Parkinson’s disease. Exp Neurol. 2018;306. https://doi.org/10.1016/j.expneurol.2018.05.017.
Fischer DL, Manfredsson FP, Kemp CJ, Cole-Strauss A, Lipton JW, Duffy MF, et al. Subthalamic nucleus deep brain stimulation does not modify the functional deficits or axonopathy induced by nigrostriatal α-synuclein overexpression. Sci Rep. 2017; 7. https://doi.org/10.1038/s41598-017-16690-x.
Spieles-Engemann AL, Steece-Collier K, Behbehani MM, Collier TJ, Wohlgenant SL, Kemp CJ, et al. Subthalamic nucleus stimulation increases brain derived neurotrophic factor in the nigrostriatal system and primary motor cortex. J Parkinsons Dis. 2011;1.https://pubmed.ncbi.nlm.nih.gov/22328911/ (Accessed 7 Aug 2023).
Huotarinen A, Penttinen A-M, Bäck S, Voutilainen MH, Julku U, Piepponen TP, et al. Combination of CDNF and deep brain stimulation decreases neurological deficits in late-stage model Parkinson’s disease. Neuroscience. 2018;374:250–63.
Miller KM, Patterson JR, Kochmanski J, Kemp CJ, Stoll AC, Onyekpe CU, et al. Striatal afferent BDNF Is disrupted by synucleinopathy and partially restored by STN DBS. J Neurosci. 2021;41. https://doi.org/10.1523/JNEUROSCI.1952-20.2020.
Chen Y, Zhu G, Liu D, Zhang X, Liu Y, Yuan T, et al. Subthalamic nucleus deep brain stimulation suppresses neuroinflammation by Fractalkine pathway in Parkinson’s disease rat model. Brain Behav Immun. 2020;90. https://doi.org/10.1016/j.bbi.2020.07.035.
Campos ACP, Kikuchi DS, Paschoa AFN, Kuroki MA, Fonoff ET, Hamani C, et al. Unraveling the role of astrocytes in subthalamic nucleus deep brain stimulation in a Parkinson’s disease rat model. Cell Mol Neurobiol. 2020; 40. https://doi.org/10.1007/s10571-019-00784-3.
Campos A, Martinez RCR, Auada AVV, Lebrun I, Fonoff ET, Hamani C, et al. Effect of subthalamic stimulation and electrode implantation in the striatal microenvironment in a Parkinson’s disease rat model. Int J Mol Sci. 2022;23. https://doi.org/10.3390/ijms232012116.
Meissner W, Harnack D, Paul G, Reum T, Sohr R, Morgenstern R, et al. Deep brain stimulation of subthalamic neurons increases striatal dopamine metabolism and induces contralateral circling in freely moving 6-hydroxydopamine-lesioned rats. Neurosci Lett. 2002;328. https://doi.org/10.1016/s0304-3940(02)00463-9.
He Z, Jiang Y, Xu H, Jiang H, Jia W, Sun P, et al. High frequency stimulation of subthalamic nucleus results in behavioral recovery by increasing striatal dopamine release in 6-hydroxydopamine lesioned rat. Behav Brain Res. 2014;263. https://doi.org/10.1016/j.bbr.2014.01.014.
Xiao G, Song Y, Zhang Y, Xing Y, Xu S, Wang M, et al. Dopamine and striatal neuron firing respond to frequency-dependent DBS detected by microelectrode arrays in the rat model of Parkinson’s disease. Biosensors. 2020;10. https://doi.org/10.3390/bios10100136.
Walker RH, Koch RJ, Moore C, Meshul CK. Subthalamic nucleus stimulation and lesioning have distinct state-dependent effects upon striatal dopamine metabolism. Synapse. 2009;63. https://doi.org/10.1002/syn.20592.
Yamamoto T, Uchiyama T, Sakakibara R, Taniguchi J, Kuwabara S. The subthalamic activity and striatal monoamine are modulated by subthalamic stimulation. Neuroscience. 2014;259. https://doi.org/10.1016/j.neuroscience.2013.11.034.
Hameleers R, Blokland A, Steinbusch HW, Visser-Vandewalle V, Temel Y. Hypomobility after DOI administration can be reversed by subthalamic nucleus deep brain stimulation. Behav Brain Res. 2007;185. https://doi.org/10.1016/j.bbr.2007.07.011.
Ihme H, Schwarting RKW, Melo-Thomas L. Low frequency deep brain stimulation in the inferior colliculus ameliorates haloperidol-induced catalepsy and reduces anxiety in rats. PLoS ONE. 2020;15:e0243438.
Dejean C, Hyland B, Arbuthnott G. Cortical effects of subthalamic stimulation correlate with behavioral recovery from dopamine antagonist induced akinesia. Cereb Cortex. 2009;19. https://doi.org/10.1093/cercor/bhn149.
Navailles S, Benazzouz A, Bioulac B, Gross C, De Deurwaerdère P. High-frequency stimulation of the subthalamic nucleus and L-3,4-dihydroxyphenylalanine inhibit in vivo serotonin release in the prefrontal cortex and hippocampus in a rat model of Parkinson’s disease. J Neurosci. 2010;30. https://doi.org/10.1523/JNEUROSCI.5031-09.2010.
Tan SK, Hartung H, Visser-Vandewalle V, Steinbusch HW, Temel Y, Sharp T. A combined in vivo neurochemical and electrophysiological analysis of the effect of high-frequency stimulation of the subthalamic nucleus on 5-HT transmission. Exp Neurol. 2012;233. https://doi.org/10.1016/j.expneurol.2011.08.027.
Creed M, Hamani C, Nobrega JN. Deep brain stimulation of the subthalamic or entopeduncular nucleus attenuates vacuous chewing movements in a rodent model of tardive dyskinesia. Eur Neuropsychopharmacol. 2011;21. https://doi.org/10.1016/j.euroneuro.2010.06.012.
Creed MC, Hamani C, Bridgman A, Fletcher PJ, Nobrega JN. Contribution of decreased serotonin release to the antidyskinetic effects of deep brain stimulation in a rodent model of Tardive dyskinesia: comparison of the subthalamic and entopeduncular nuclei. J Neurosci. 2012;32:9574.
Li S, Arbuthnott GW, Jutras MJ, Goldberg JA, Jaeger D. Resonant antidromic cortical circuit activation as a consequence of high-frequency subthalamic deep-brain stimulation. J Neurophysiol. 2007;98 https://doi.org/10.1152/jn.00808.2007.
Cordon I, Nicolás MJ, Arrieta S, Alegre M, Artieda J, Valencia M. Theta-phase closed-loop stimulation induces motor paradoxical responses in the rat model of Parkinson disease. Brain Stimul. 2018;11. https://doi.org/10.1016/j.brs.2017.10.004.
Yamamoto T, Sakakibara R, Uchiyama T, Kuwabara S. Subthalamic stimulation inhibits bladder contraction by modulating the local field potential and catecholamine level of the medial prefrontal cortex. Front Neurosci. 2020;14:566911.
Waku I, Magalhães MS, Alves CO, de Oliveira AR. Haloperidol-induced catalepsy as an animal model for parkinsonism: A systematic review of experimental studies. Eur J Neurosci. 2021;53:3743–67.
Duty S, Jenner P. Animal models of Parkinson’s disease: a source of novel treatments and clues to the cause of the disease. Br J Pharm. 2011;164:1357–91.
Liu H, Wolters A, Temel Y, Alosaimi F, Jahanshahi A, Hescham S. Deep brain stimulation of the nucleus basalis of Meynert in an experimental rat model of dementia: Stimulation parameters and mechanisms. Neurobiol Dis. 2022;171:105797.
Jeong DU, Lee J, Chang WS, Chang JW. Identifying the appropriate time for deep brain stimulation to achieve spatial memory improvement on the Morris water maze. BMC Neurosci. 2017;18:29.
Do-Monte FH, Rodriguez-Romaguera J, Rosas-Vidal LE, Quirk GJ. Deep brain stimulation of the ventral striatum increases BDNF in the fear extinction circuit. Front Behav Neurosci. 2013;7:102.
Lin H-C, Pan H-C, Lin S-H, Lo Y-C, Shen ET-H, Liao L-D, et al. Central thalamic deep-brain stimulation alters striatal-thalamic connectivity in cognitive neural behavior. Front Neural Circuits. 2015;9:87.
Hescham S, Jahanshahi A, Schweimer JV, Mitchell SN, Carter G, Blokland A, et al. Fornix deep brain stimulation enhances acetylcholine levels in the hippocampus. Brain Struct Funct. 2016;221:4281–6.
Fernández-Cabrera MR, Selvas A, Miguéns M, Higuera-Matas A, Vale-Martínez A, Ambrosio E, et al. Parafascicular thalamic nucleus deep brain stimulation decreases NMDA receptor GluN1 subunit gene expression in the prefrontal cortex. Neuroscience. 2017;348:73–82.
Premarket Approval (PMA). https://www.accessdata.fda.gov/scripts/cdrh/cfdocs/cfpma/pma.cfm?id=P960009S219 (Accessed 8 Aug 2023).
Amorim BO, Covolan L, Ferreira E, Brito JG, Nunes DP, de Morais DG, et al. Deep brain stimulation induces antiapoptotic and anti-inflammatory effects in epileptic rats. J Neuroinflammation. 2015;12:162.
Ferreira ES, Vieira LG, Moraes DM, Amorim BO, Malheiros JM, Hamani C, et al. Long-term effects of anterior thalamic nucleus deep brain stimulation on spatial learning in the pilocarpine model of temporal lobe epilepsy. Neuromodulation. 2018;21:160–7.
Gimenes C, Motta Pollo ML, Diaz E, Hargreaves EL, Boison D, Covolan L. Deep brain stimulation of the anterior thalamus attenuates PTZ kindling with concomitant reduction of adenosine kinase expression in rats. Brain Stimul. 2022;15:892–901.
Miranda MF, Hamani C, de Almeida A-CG, Amorim BO, Macedo CE, Fernandes MJS, et al. Role of adenosine in the antiepileptic effects of deep brain stimulation. Front Cell Neurosci. 2014;8:312.
Mihály I, Molnár T, Berki Á-J, Bod R-B, Orbán-Kis K, Gáll Z, et al. Short-term amygdala low-frequency stimulation does not influence hippocampal interneuron changes observed in the pilocarpine model of epilepsy. Cells 2021;10. https://doi.org/10.3390/cells10030520.
Wu G, Wang L, Hong Z, Ren S, Zhou F. Hippocampal low-frequency stimulation inhibits afterdischarge and increases GABA (A) receptor expression in amygdala-kindled pharmacoresistant epileptic rats. Neurol Res. 2017. https://doi.org/10.1080/01616412.2017.1325120.
Bae S, Lim H-K, Jeong Y, Kim S-G, Park S-M, Shon Y-M, et al. Deep brain stimulation of the anterior nuclei of the thalamus can alleviate seizure severity and induce hippocampal GABAergic neuronal changes in a pilocarpine-induced epileptic mouse brain. Cereb Cortex. 2022;32:5530–43.
Liu D-F, Chen Y-C, Zhu G-Y, Wang X, Jiang Y, Liu H-G, et al. Effects of anterior thalamic nuclei stimulation on gene expression in a rat model of temporal lobe epilepsy. Acta Neurol Belg. 2019;120:1361–70.
Volkow ND, Morales M. The brain on drugs: from reward to addiction. Cell. 2015;162:712–25.
Koo M-S, Kim E-J, Roh D, Kim C-H. Role of dopamine in the pathophysiology and treatment of obsessive-compulsive disorder. Expert Rev Neurother. 2010;10:275–90.
Yuen J, Kouzani AZ, Berk M, Tye SJ, Rusheen AE, Blaha CD, et al. Deep brain stimulation for addictive disorders-where are we now? Neurotherapeutics. 2022;19:1193–215.
McCracken CB, Grace AA. High-frequency deep brain stimulation of the nucleus accumbens region suppresses neuronal activity and selectively modulates afferent drive in rat orbitofrontal cortex in vivo. J Neurosci. 2007;27:12601–10.
Kallupi M, Kononoff J, Melas PA, Qvist JS, de Guglielmo G, Kandel ER, et al. Deep brain stimulation of the nucleus accumbens shell attenuates cocaine withdrawal but increases cocaine self-administration, cocaine-induced locomotor activity, and GluR1/GluA1 in the central nucleus of the amygdala in male cocaine-dependent rats. Brain Stimul. 2022;15:13–22.
Gouveia FV, Silk E, Davidson B, Pople CB, Abrahao A, Hamilton J, et al. A systematic review on neuromodulation therapies for reducing body weight in patients with obesity. Obes Rev. 2021;22:e13309.
Gouveia FV, Gomes de Alvarenga P, Alho EJL, Takahashi RES, Franco R, Lopes AC, et al. The ansa subthalamica as a substrate for DBS-induced manic symptoms. Brain Stimul. 2020;13:1399–401.
Diepenbroek C, van der Plasse G, Eggels L, Rijnsburger M, Feenstra MGP, Kalsbeek A, et al. Alterations in blood glucose and plasma glucagon concentrations during deep brain stimulation in the shell region of the nucleus accumbens in rats. Front Neurosci. 2013;7:226.
Sani S, Jobe K, Smith A, Kordower JH, Bakay RAE. Deep brain stimulation for treatment of obesity in rats. J Neurosurg. 2007;107:809–13.
Soto-Montenegro ML, Pascau J, Desco M. Response to deep brain stimulation in the lateral hypothalamic area in a rat model of obesity: in vivo assessment of brain glucose metabolism. Mol Imaging Biol. 2014;16:830–7.
Casquero-Veiga M, Bueno-Fernandez C, Romero-Miguel D, Lamanna-Rama N, Nacher J, Desco M, et al. Exploratory study of the long-term footprint of deep brain stimulation on brain metabolism and neuroplasticity in an animal model of obesity. Sci Rep. 2021;11:5580.
Xu T, Gao Y, Li B, Jiang J, Guo H, Liu X, et al. The efficacy and safety of deep brain stimulation of combined anterior limb of internal capsule and nucleus accumbens (ALIC/NAcc-DBS) for treatment-refractory obsessive-compulsive disorder: protocol of a multicenter, randomized, and double-blinded study. Brain Sci. 2022;12. https://doi.org/10.3390/brainsci12070933.
Xiong B, Li B, Wen R, Gao Y, Gong F, Li D, et al. Use of differential stimulation of the nucleus accumbens and anterior limb of the internal capsule to improve outcomes of obsessive-compulsive disorder. J Neurosurg. 2023;139:1–10.
Germann J, Elias GJB, Neudorfer C, Boutet A, Chow CT, Wong EHY, et al. Potential optimization of focused ultrasound capsulotomy for obsessive compulsive disorder. Brain. 2021;144:3529–40.
McCracken CB, Grace AA. Nucleus accumbens deep brain stimulation produces region-specific alterations in local field potential oscillations and evoked responses in vivo. J Neurosci. 2009;29:5354–63.
Angelov SD, Dietrich C, Krauss JK, Schwabe K. Effect of deep brain stimulation in rats selectively bred for reduced prepulse inhibition. Brain Stimul. 2014;7:595–602.
Manning EE, Wang AY, Saikali LM, Winner AS, Ahmari SE. Disruption of prepulse inhibition is associated with compulsive behavior severity and nucleus accumbens dopamine receptor changes in Sapap3 knockout mice. Sci Rep. 2021;11:9442.
Kohl S, Gruendler TOJ, Huys D, Sildatke E, Dembek TA, Hellmich M, et al. Effects of deep brain stimulation on prepulse inhibition in obsessive-compulsive disorder. Transl Psychiatry. 2015;5:e675.
Bregman T, Nona C, Volle J, Diwan M, Raymond R, Fletcher PJ, et al. Deep brain stimulation induces antidepressant-like effects in serotonin transporter knockout mice. Brain Stimul. 2018;11:423–5.
Hamani C, Diwan M, Macedo CE, Brandão ML, Shumake J, Gonzalez-Lima F, et al. Antidepressant-like effects of medial prefrontal cortex deep brain stimulation in rats. Biol Psychiatry. 2010;67:117–24.
Lim LW, Prickaerts J, Huguet G, Kadar E, Hartung H, Sharp T, et al. Electrical stimulation alleviates depressive-like behaviors of rats: investigation of brain targets and potential mechanisms. Transl Psychiatry. 2015;5:e535.
Etiévant A, Oosterhof C, Bétry C, Abrial E, Novo-Perez M, Rovera R, et al. Astroglial control of the antidepressant-like effects of prefrontal cortex deep brain stimulation. EBioMedicine. 2015;2:898–908.
van Dijk A, Klompmakers AA, Feenstra MGP, Denys D. Deep brain stimulation of the accumbens increases dopamine, serotonin, and noradrenaline in the prefrontal cortex. J Neurochem. 2012;123:897–903.
Schumacher A, Haegele M, Spyth J, Moser A. Electrical high frequency stimulation of the nucleus accumbens shell does not modulate depressive-like behavior in rats. Behav Brain Res. 2020;378:112277.
van Dijk A, Mason O, Klompmakers AA, Feenstra MGP, Denys D. Unilateral deep brain stimulation in the nucleus accumbens core does not affect local monoamine release. J Neurosci Methods. 2011;202:113–8.
Klanker M, Feenstra M, Willuhn I, Denys D. Deep brain stimulation of the medial forebrain bundle elevates striatal dopamine concentration without affecting spontaneous or reward-induced phasic release. Neuroscience. 2017;364:82–92.
Ashouri Vajari D, Ramanathan C, Tong Y, Stieglitz T, Coenen VA, Döbrössy MD. Medial forebrain bundle DBS differentially modulates dopamine release in the nucleus accumbens in a rodent model of depression. Exp Neurol. 2020;327:113224.
Jiménez-Sánchez L, Castañé A, Pérez-Caballero L, Grifoll-Escoda M, López-Gil X, Campa L, et al. Activation of AMPA receptors mediates the antidepressant action of deep brain stimulation of the infralimbic prefrontal cortex. Cereb Cortex. 2016;26:2778–89.
Bambico FR, Bregman T, Diwan M, Li J, Darvish-Ghane S, Li Z, et al. Neuroplasticity-dependent and -independent mechanisms of chronic deep brain stimulation in stressed rats. Transl Psychiatry. 2015;5:e674.
Sun Z, Jia L, Shi D, He Y, Ren Y, Yang J, et al. Deep brain stimulation improved depressive-like behaviors and hippocampal synapse deficits by activating the BDNF/mTOR signaling pathway. Behav Brain Res. 2022;419:113709.
Bezchlibnyk YB, Stone SSD, Hamani C, Lozano AM. High frequency stimulation of the infralimbic cortex induces morphological changes in rat hippocampal neurons. Brain Stimul. 2017;10:315–23.
Bruchim-Samuel M, Lax E, Gazit T, Friedman A, Ahdoot H, Bairachnaya M, et al. Electrical stimulation of the vmPFC serves as a remote control to affect VTA activity and improve depressive-like behavior. Exp Neurol. 2016;283:255–63.
Hamani C, Machado DC, Hipólide DC, Dubiela FP, Suchecki D, Macedo CE, et al. Deep brain stimulation reverses anhedonic-like behavior in a chronic model of depression: role of serotonin and brain derived neurotrophic factor. Biol Psychiatry. 2012;71:30–35.
Dandekar MP, Saxena A, Scaini G, Shin JH, Migut A, Giridharan VV, et al. Medial forebrain bundle deep brain stimulation reverses anhedonic-like behavior in a chronic model of depression: importance of BDNF and inflammatory cytokines. Mol Neurobiol. 2019;56:4364–80.
Jiménez-Sánchez L, Linge R, Campa L, Valdizán EM, Pazos Á, Díaz Á, et al. Behavioral, neurochemical and molecular changes after acute deep brain stimulation of the infralimbic prefrontal cortex. Neuropharmacology. 2016;108:91–102.
Shin LM, Liberzon I. The neurocircuitry of fear, stress, and anxiety disorders. Neuropsychopharmacology. 2009;35:169–91.
Mokhtari Hashtjini M, Pirzad Jahromi G, Meftahi GH, Esmaeili D, Javidnazar D. Aqueous extract of saffron administration along with amygdala deep brain stimulation promoted alleviation of symptoms in post-traumatic stress disorder (PTSD) in rats. Avicenna J Phytomed. 2018;8:358–69.
Hashtjini MM, Jahromi GP, Sadr SS, Meftahi GH, Hatef B, Javidnazar D. Deep brain stimulation in a rat model of post-traumatic stress disorder modifies forebrain neuronal activity and serum corticosterone. Iran J Basic Med Sci. 2018;21:370–5.
Sui L, Huang S, Peng B, Ren J, Tian F, Wang Y. Deep brain stimulation of the amygdala alleviates fear conditioning-induced alterations in synaptic plasticity in the cortical-amygdala pathway and fear memory. J Neural Transm. 2014;121:773–82.
Pitkänen A, Dvm PB, Galanopoulou AS, Moshé SL. Models of seizures and epilepsy. Elsevier Science; 2017.
Dürmüller N, Porsolt RD. Electrical amygdala kindling. Curr Protoc Pharmacol. 2003;Chapter 5:Unit5.33. https://doi.org/10.1002/0471141755.ph0533s22.
Perez SM, Shah A, Asher A, Lodge DJ. Hippocampal deep brain stimulation reverses physiological and behavioural deficits in a rodent model of schizophrenia. Int J Neuropsychopharmacol. 2013;16:1331–9.
Lu C, Feng Y, Li H, Gao Z, Zhu X, Hu J. A preclinical study of deep brain stimulation in the ventral tegmental area for alleviating positive psychotic-like behaviors in mice. Front Hum Neurosci. 2022;16:945912.
Magdaleno-Madrigal VM, Contreras-Murillo G, Camacho-Abrego I, Negrete-Díaz JV, Valdés-Cruz A, Fernández-Mas R, et al. Short-term deep brain stimulation of the thalamic reticular nucleus modifies aberrant oscillatory activity in a neurodevelopment model of schizophrenia. Neuroscience. 2017;357:99–109.
Dong X, Ye W, Tang Y, Wang J, Zhong L, Xiong J, et al. Wakefulness-promoting effects of lateral hypothalamic area-deep brain stimulation in traumatic brain injury-induced comatose rats: upregulation of α1-adrenoceptor subtypes and downregulation of gamma-aminobutyric acid β receptor expression via the orexins pathway. World Neurosurg. 2021;152:e321–e331.
Lee DJ, Gurkoff GG, Izadi A, Seidl SE, Echeverri A, Melnik M, et al. Septohippocampal neuromodulation improves cognition after traumatic brain injury. J Neurotrauma. 2015;32:1822–32.
Majdi A, Deng Z, Sadigh-Eteghad S, De Vloo P, Nuttin B, Mc Laughlin M. Deep brain stimulation for the treatment of Alzheimer’s disease: a systematic review and meta-analysis. Front Neurosci. 2023;17:1154180.
Whiting DM, Tomycz ND, Bailes J, de Jonge L, Lecoultre V, Wilent B, et al. Lateral hypothalamic area deep brain stimulation for refractory obesity: a pilot study with preliminary data on safety, body weight, and energy metabolism. J Neurosurg. 2013;119:56–63.
Gubellini P, Salin P, Kerkerian-Le Goff L, Baunez C. Deep brain stimulation in neurological diseases and experimental models: from molecule to complex behavior. Prog Neurobiol. 2009;89:79–123.
Alpaugh M, Saint-Pierre M, Dubois M, Aubé B, Arsenault D, Kriz J, et al. A novel wireless brain stimulation device for long-term use in freely moving mice. Sci Rep. 2019;9:6444.
Parastarfeizabadi M, Kouzani AZ. Advances in closed-loop deep brain stimulation devices. J Neuroeng Rehabil. 2017;14:79.
Kiani AK, Pheby D, Henehan G, Brown R, Sieving P, Sykora P, et al. Ethical considerations regarding animal experimentation. J Prev Med Hyg. 2022;63:E255–E266.
Andersen ML, Winter LMF. Animal models in biological and biomedical research - experimental and ethical concerns. Acad Bras Cienc. 2019;91:e20170238.
Díaz L, Zambrano E, Flores ME, Contreras M, Crispín JC, Alemán G, et al. Ethical considerations in animal research: the principle of 3R’s. Rev Invest Clin. 2020;73:199–209.
Viaña JNM, Bittlinger M, Gilbert F. Ethical considerations for deep brain stimulation trials in patients with early-onset Alzheimer’s disease. J Alzheimers Dis. 2017;58:289–301.
Sankary LR, Ford PJ, Machado AG, Hoeksema LJ, Samala RV, Harris DJ. Deep brain stimulation at end of life: clinical and ethical considerations. J Palliat Med. 2020;23:582–5.
Grant RA, Halpern CH, Baltuch GH, O’Reardon JP, Caplan A. Ethical considerations in deep brain stimulation for psychiatric illness. J Clin Neurosci. 2014;21:1–5.
Lo C, Mane M, Kim JH, Berk M, Sharp RR, Lee KH, et al. Treating addiction with deep brain stimulation: Ethical and legal considerations. Int J Drug Policy. 2023;113:103964.
Stahl D, Cabrera L, Gibb T. Should DBS for psychiatric disorders be considered a form of psychosurgery? Ethical and legal considerations. Sci Eng Ethics. 2018;24:1119–42.
Behmer Hansen RT, Dubey A, Smith C, Henry PJ, Mammis A. Paediatric deep brain stimulation: ethical considerations in malignant Tourette syndrome. J Med Ethics. 2020;46:668–73.
Davidson B, Elkaim LM, Lipsman N, Ibrahim GM. Editorial. An ethical framework for deep brain stimulation in children. Neurosurg Focus. 2018;45:E11.
Muñoz KA, Kostick K, Sanchez C, Kalwani L, Torgerson L, Hsu R, et al. Researcher perspectives on ethical considerations in adaptive deep brain stimulation trials. Front Hum Neurosci. 2020;14:578695.
Funding
This work was supported by funds from Canadian Institutes of Health Research (CIHR) Postdoctoral Fellowship #472484 (FVG), CIHR Canada Graduate Scholarship-Master’s Program (KKZ), The Rising Star - Shireen and Edna Marcus Excellence Award has been made possible by Brain Canada Foundation and the Shireen and Edna Marcus Foundation (FVG).
Author information
Authors and Affiliations
Contributions
KKZ: Acquisition, analysis and interpretation of data, drafting and revising the manuscript. RM: Acquisition, analysis and interpretation of data, drafting and revising the manuscript. CG: Critically revising the manuscript and providing intellectual content. GMI: Conception and design of the study, critically revising the manuscript and providing intellectual content. FVG: Conception and design of the study, analysis and interpretation of data, critically revising the manuscript and providing intellectual content. All authors approved the final version to be published. GMI and FVG jointly supervised this work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zhang, K.K., Matin, R., Gorodetsky, C. et al. Systematic review of rodent studies of deep brain stimulation for the treatment of neurological, developmental and neuropsychiatric disorders. Transl Psychiatry 14, 186 (2024). https://doi.org/10.1038/s41398-023-02727-5
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41398-023-02727-5