Abstract
Medication-related osteonecrosis of the jaw (MRONJ) is a serious adverse reaction associated with antiresorptive drugs such as bisphosphonates and denosumab. When dealing with advanced and/or multiple MRONJ lesions undergoing surgical therapy, the extent of surgery is often a topic of discussion. The aim of this study was to identify the differences in bone density in and around the MRONJ lesion before and after surgical treatment to evaluate the needed surgical extend of the modelling osteotomy. In this retrospective study 26 patients with MRONJ lesions that were surgically treated in our department were observed. Length, width and bone density were measured in panoramic radiograph pre and postoperatively with the Imaging processing software Sidexis and ImageJ (Fiji). The necrotic area, the surrounding sclerotic area as well as the healthy contralateral side were observed. Measurements were performed by two independent observers. Pearson correlation was calculated to determine the interobserver variability. Bone density was significantly reduced in the necrotic bone area compared to the healthy unaffected contralateral reference side. The sclerotic bone area surrounding the necrosis showed increased bone density compared to the contralateral unaffected reference side. The density of the sclerotic bone area was increased in the previously affected MRONJ area in the postoperative panoramic radiograph. The pre and postoperative density showed no significant correlation to healing behaviour. The focus of the modelling osteotomy in surgical treatment of mature MRONJ lesions should be predominantly on the parts that appear necrotic and less dense in the panoramic radiograph as sclerotic areas might be an expression of bone reaction.
Similar content being viewed by others
Introduction
Medication-related osteonecrosis of the jaw (MRONJ) is a severe adverse reaction caused by antiresorptive therapy (AR) or antiangiogenic therapy (AA)1. Typical clinical findings are necrotic alveolar bone, infection of the surrounding tissues and fistulas2. Around 1–15% of all patients with AR develop MRONJ in the course of disease3. The dose of AR, the frequency of application, hygiene of the oral cavity and co-medications play a role in the pathogenesis of MRONJ4,5,6.
The pathophysiology of MRONJ is still not fully elucidated which makes the treatment of MRONJ a challenge to surgeons7. Different therapy approaches have been performed as conservative treatment with antibiotics8, surgical treatment including osteotomy and removing of the sequestra and the surrounding soft tissue9, and even more radical approaches like mandibular resection followed by reconstruction10,11. Imaging is recommended to evaluate the preoperative extent of the necrosis. Panoramic radiography is still the imaging method of choice for a routine dental assessment in these patients12 and it is the most available dental imaging technique with a low radiation dose. Typical findings are osteolytic areas corresponding to the necrotic area. In some cases sequestra of the bone can be found13 and most of the patients show osseous sclerosis around the necrotic area. Also new bone formation and possible narrowing of the mandible canal are described14.
The extent of surgical treatment is often discussed as radical treatment can influence quality of life of patients due to aesthetic limitations, facial dysmorphisms or speech impairment15. The sclerotic zone that forms around the necrosis is often thought to be a pathological bone change and is therefore surgically removed16. However, considering the physiological bone metabolism, this zone is rather regarded as new formation of bone as a reaction to the inflammation17. Therefore the aim of this study was to identify the differences in bone density in panoramic radiograph in and around the MRONJ lesion before and after surgical treatment to evaluate the needed surgical extend of the modelling osteotomy.
Material and methods
This retrospective study was approved by the institutional review board of the University Hospital of the Ludwig-Maximilians-University Munich, Germany (Munich, Germany; UE Nr 22-0445). Informed consent was waived by the institutional review board of the University Hospital of the Ludwig-Maximilians-University Munich, Germany (Munich, Germany; UE Nr 22-0445) due to the retrospective nature of the data. All research was performed in accordance with the guidelines of the Declaration of Helsinki. It includes results of patients treated in an ambulant setting or as patients in our hospital between 2014 and 2022. Patients´ medical records as demographic data, number of lesions per patient, healed vs non-healed lesion, bisphosphonate medication (sort of bisphosphonate, dosis, duration of intake, underlying disease of intake) as well as pre- and postoperative panoramic radiograph have been screened, evaluated and reported according to the STROBE (STrengthening the Reporting of OBservational studies in Epidemiology) guidelines. All methods were performed in accordance with the guidelines and regulations of this journal.
Inclusion criteria
Patients with pre- and postoperative panoramic radiograph were included in this study. Patients with MRONJ caused by antiresorptive drugs (bisphosphonates and denosumab) with Stage I, II and III in the maxilla or the mandible were included. For the diagnosis of MRONJ lesions the definition of the American Association of Oral and Maxillofacial Surgeon´s positioning paper (update 2022) was used18. Only patients who received surgical therapy were included. All patients received conservative therapy prior to surgical treatment including long-term antibiotic treatment, as well as local disinfectant measures, especially locally disinfectant rinses. Patients with more than one lesion were included, as long as the lesions were not located in the same jaw in order to measure the contralateral healthy side as a reference.
Exclusion criteria
Patients with osteoradionecrosis were excluded. All patients with alio loco panoramic radiograph were excluded. Patients with low-quality panoramic radiograph (wrong positioning, too much overlap in the region of interest, metal artefacts) and without clearly visible necrosis in the panoramic radiograph (only clinical exposure of necrotic bone) were excluded. The preoperative panoramic radiograph must not be older than 2 weeks when surgery was performed. Patients with previous lesions were excluded and patients with postoperative panoramic radiograph less than 3 months after surgery were excluded as well. 148 patients were screened for eligibility. 26 patients were included in this study. The identification process of included patients is shown in Fig. 1.
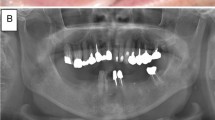
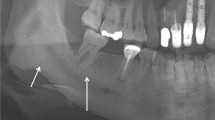
All patients received surgical treatment. Surgical treatment of MRONJ included exploration of the affected area and visualization of the entire extent of the lesion. The necrotic bone areas were resected visually and under fluorescence control. This enabled targeted and standardized therapy with reduced invasiveness. Resection was followed by a tight, tension-free wound closure if possible, in multiple layers. Depending on the localization of the defect, fibers of the mylohyoid muscle or the corpus adiposum buccae were prepared as an additional layer as part of the wound closure, mobilized vestibularly over the alveolar ridge and fixed there. Operations were performed under local anesthesia or intubation anesthesia combined with local anesthesia depending on the size of the defect and the patients constitution. In addition pre and postoperative antibiotic therapy (3 g Ampcillin/Sulbactam or 600 mg Clindamycin in case of penicillin allergy three times per day) was applied in all patients. All panoramic radiographs were taken in our department with Orthophos XG (Sirona Dental System) and equal exposition settings to avoid bias. Postoperative panoramic radiographs were performed with a minimum interval of 3 months post-operation. The density of the necrotic zone, the reactive sclerotic zone around the necrosis and the postoperative sclerotic zone were measured with Sidexis 4 (Dentsply Sirona, Charlotte, North Carolina, USA) and are reported in percent. Five points were measured equally distributed in the above localizations respectively. For a healthy reference, five mirror-image points were measured on the opposite unaffected reference side (URS) in each case. In case that the mirrored points overlapped with anatomical structures of a different density, these were slightly displaced so that the reference points were located in healthy bone areas. To further validate the findings, the complete zones were measured again with the image processing programme Fiji (ImageJ, U. S. National Institutes of Health, Bethesda, Maryland, USA) and are reported in numeric grey value. All measurements were performed by two independent observers. Pearson correlation was calculated to determine the interobserver variability. An example of the methods is shown in Fig. 2.
Statistical analysis
Qualitative and quantitative data were observed, normally distributed data were presented using mean ± standard deviation (SD). Data were tested for normal distribution with the Shapiro–Wilk test. An unpaired t-test was used for the comparison of preoperative necrosis and preoperative URS, preoperative sclerosis and URS and postoperative sclerosis and postoperative URS. For comparisons between pre- and post-operative values especialle sclerosis pre and postoperative a paired t-test was selected for hypothesis testing. The significance level was defined at p ≤ 0.05. Statistical analysis was conducted using SPSS® 24 version 4.0 (SPSS Inc., Chicago, IL, USA).
Results
26 patients were included in this study. 15 patients (57.7%) were female and 11 (42.3%) male. The mean age at time of first diagnosis of the MRONJ lesion was 70.20 years. Tables 1 and 2 show demographic data, the underlying disease that required AR and the AR itself. Patients with Zolendronate 4 mg or Pamidronate 30 mg received the medications intravenously, patients receiving Denosumab received the medication subcutaneous. Pearson correlation was calculated to determine the interobserver variability. Pearson correlation for the Preoperative URS was 0.6, 0.7 for the necrotic area, 0.6 for the preoperative sclerotic area, 0.7 for the postoperative sclerotic area and 0.6 for the postoperative URS. The average length of the necrotic area measured on panoramic radiograph was 25.3 ± 10.3 mm, the average width was 14.6 ± 7.5 mm. The preoperative density of the necrotic zone was 29.9 ± 5.5% (Sidexis) and 77.6 ± 13.4 (ImageJ). On the URS the medium bone density amounted 42.0 ± 5.0% and 101.1 ± 16.7. The sclerotic area around the necrotic area was 46.9 ± 4.0% and 108.7 ± 15.4. Postoperatively the density of the sclerotic bone area amounted 46.2% ± 4.1% and 112.7 ± 13.4 compared to the URS with 42.8% ± 5.3% and 101.1 ± 16.7. The unpaired t-test showed a statistically significant difference between the density of the necrotic zone and the preoperative URS in both measurement techniques (p = 0.00). The preoperative sclerotic zone around the MRONJ lesion showed a statistical significant difference to the UPS (p = 0.00) with Sidexis and with ImageJ (p = 0.04). The postoperative sclerotic zone showed statistical significant higher density values compared to the postoperative URS (p = 0.00) with Sidexis as well as ImageJ (p = 0.01). Tables 3 and 4 show analysis of bone density and p-values. There was no statistical significant correlation between duration of antiresorptive treatment and bone density. In addition two of the 26 patients did not show healing. In both cases, the lesion was located in the lower jaw. The pre and postoperative density showed no significant correlation to healing behaviour. The hypothesis that non-healed bone showed a higher or lower bone density was not confirmed in this study.
Discussion
Surgery has been described as an effective therapeutic regimen for reducing pain in patients suffering from MRONJ who did not respond to conservative treatment19. Surgical treatment includes sequestrectomy, debridement, resection and immediate reconstruction and may also include extraction of teeth within exposed necrotic bone20. In the treatment of MRONJ lesions, there is still disagreement about the extent of resection. While some authors suggest a more conservative approach21, such as sequestrectomy and surgical debridement others advocate more aggressive therapies, such as resections of affected bone with bigger reconstruction including free flaps and microsurgical reconstruction.
The major challenge in surgical treatment in MRONJ is the delineation between necrotic and viable bone to ensure complete removal of necrotic bone while preserving as much vital bone as possible22. Wilde et al. recommend a full-thickness mucoperiosteal flap that should be high and extended to reveal the entire area of exposed bone until disease-free margins are localized; resection of the affected bone should be extended as far as healthy-appearing, bleeding bone is reached considering to smooth sharp edges and primary soft tissue closure is achieved23. Seth et al. analysed outcomes of vascularized bone graft reconstruction of the mandible in medication-related osteonecrosis of the jaw; in eleven patients a complication rate of 36% was reported. Complications included infection, fistula, hematoma, pneumonia, deep vein thrombosis and free flap loss24. Similar results were reported by Hanasono et al. who report a complication rate of 46%25.
Meanwhile it has been shown that a moderate surgical treatment results in better healing since the periosteum and unaffected bone are preconserved26. In a case of a 73 year old women with bisphonate therapy for 10 years who was diagnosed with stage III MRONJ lesion, panoramic radiographs revealed a 3-cm-long lesion on the body of the mandible starting from the mental foramen and extending to the posterior region with a reactive bone formation as a result of periosteal activation. Necrotic bone was removed while protecting the periosteum; as a result the 1-year follow-up panoramic radiographs showed complete regeneration of the bone27.
The radiographic features of MRONJ remain relatively unspecific. In the early stages of the disease plain radiography does not typically demonstrate abnormalities of the affected bone. Cortical bone thickening and increased trabecular bone density are suspected to be early imaging features of MRONJ28. In addition osteolysis, mandibular canal enhancement, and bone sclerosis have already been described as typical findings of different MRONJ stages in panoramic radiograph29. Computed tomography diagnostic imaging findings are assumed to be more sensitive to changes in bone mineralization, compared to panoramic radiography30. Even though CT often shows a greater quality of bone changes, still, radiographic findings in panoramic radiography such as sclerosis, cortical irregularity, lucency, mottling, fragmentation/sequestra formation, sinus communication, and persistent sockets are reported to have the ability to characterize the extent of the MRONJ lesion as well31.
Regarding the imaging modality specific guidelines for routine clinical care have not yet been recommended32. While in CT the evaluation of Hounsfield Units (HU) is a valid tool for assessing bone density, in plain radiography, the observation of bone density through gray values in ImageJ is a validated tool in dentistry33 as well as in orthopedics34. Therefore, it remains to be considered individually whether the increased radiation exposure of a CT is actually relevant for the treatment decision.
Fluorescence-guided bone surgery of medication‐related osteonecrosis of the jaw can actually help to visualise vital bone intraoperatively due to autofluorescence of vital bone35. This technique may help to define the transitions between necrotic and none-necrotic bone during the surgical procedure providing a controllable therapeutic approach36. Still as this method is not always available other methods to assess the extent of surgical resection are needed.
As shown in our data, density meausrements with Sidexis and ImageJ showed a significant difference in bone density between the preoperative sclerotic appearing zone and the healthy unaffected reference bone (p = 0.00). In addition the necrotic areas showed a significant reduction in bone density compared to the URS. This indicates that the focus of the modelling osteotomy should be predominantly on the parts that appear necrotic and osteolytic in the panoramic radiograph. Sclerotic areas are already described as an expression of bone reaction during initial bone healing phase37,38 and should therefore not be removed. This observation can be explained by the principles of bone metabolism: in damaged bone, apoptotic osteocytes signal the location and size of damage to lining cells leading to the formation of the bone remodelling compartment (BRC). The BRC confines and targets remodeling to the damage in order to minimize the removal of normal bone39. As bisphosphonates bind strongly at sites of mineral deposition in osteoid as well as to resorption sites, they do not only inhibit osteoclastic bone resorption in physiological remodelling, but also in pathological processes40,41, indicating that the usage of antiresorptive agents such as bisphosphonates or denosumab increases bone density42 independently on the formation of MRONJ lesions.
This goes along with the finding, that the pre- and postoperative density showed no significant correlation to healing behaviour. The hypothesis that non-healed bone showed a higher bone density was not confirmed in this study and reinforces the hypothesis, that preoperative appearing sclerotic bone should not be removed. Postoperative appearing sclerosis as in our data has also been observed in other bone entities as a result of bone reaction after osteotomy. Even after segmental mandibulectomy in MRONJ patients sclerosis was observed in the postoperative CT16. In addition it was also shown in tibial osteotomies that the sclerosis appearing postoperative in the conventional radiograph proved to be new bone in the CT and could therefore be identified as reliable parameter for ossification43.
In this study the density of the different bone areas was identified comparing pre-and post-operative panoramic images measured by two independent observers. Pearson correlation showed an acceptable inter rater reliability in choosing the extent of necrotic and sclerotic zones, still, interrater bias are limitations of this method described in this retrospective study, even though this is also faced when segmenting CT or CBCT. In addition positioning of the patient during the radiograph might also influence the image density values. In order to minimize measurement bias, contrast as well as exposition and machine settings were set to fixed standardized parameters when acquiring the image. In Germany it is mandatory to perform a monthly constancy test using test specimen for dental x-ray systems to guarantee correct resolution, contrast and radiation field. This procedure acts as a quality control for equal imaging parameters reducing the risk of imaging bias in our study.
Therefore, ImageJ and Sidexis Density Analysis might offer a reliable tool for clinicians to improve preoperative analysis and planning on the extent of the modelling osteotomy in MRONJ lesions. It offers an option to avoid extensive surgery resulting in large defects of the jaw which further influence postoperative dental rehabilitation and quality of life44,45. Methods like ImageJ and Sidexis density analysis are fast and easy available and are therefore easily included in pre- and postoperative imaging assessment in osteonecrosis of the jaw. As the above described methods are even applicable in ambulant dental practice that perform regular dental screening in order to prevent or diagnose MRONJ in an early stage in patients with antiresorptive drugs, this methodology might also detect MRONJ lesions in early stages.
In addition advantage of the here presented methology is the low radiation exposure of the patients. In most cases there is no justifying indication for both, pre and post-operative CBCT. Therefore this method is a low radiation alternative for bone density evaluation in the jaw. Still larger studies analysing both, bone density in panoramic radiography and CT in MRONJ are desirable to further validate our findings.
Conclusion
Sclerotic-appearing bone areas around the necrosis in MRONJ lesions showed a higher bone density pre- and postoperatively compared to the healthy unaffected side. The pre- and postoperative density showed no significant correlation to healing behaviour. The hypothesis that non-healed bone showed a higher bone density was not confirmed in this study. Sclerotic areas around necrotic bone in MRONJ lesions might be an expression of bone reaction, and should therefore not be removed. Density measurements with Sidexis and ImageJ in the panoramic radiograph could be established as a handable option for dentists and oral and maxillofacial surgeons to evaluate MRONJ lesions without 3D imaging. The extent of the sclerotic area could be used as a surgical guide for the extent of surgery and modelling osteotomy.
Data availability
The datasets generated and/or analysed during the current study are not publicly available due but are available from the corresponding author on reasonable request, as during the data evaluation process all data has been anonymised.
References
Govaerts, D. et al. Adjuvant therapies for MRONJ: A systematic review. Bone 141, 115676 (2020).
Advisory Task Force on Bisphosphonate-Related Ostenonecrosis of the Jaws AAoO Maxillofacial S. American Association of Oral and Maxillofacial Surgeons position paper on bisphosphonate-related osteonecrosis of the jaws. J. Oral Maxillofac. Surg. 65(3):369–376 (2007).
Aljohani, S. et al. What is the effect of anti-resorptive drugs (ARDs) on the development of medication-related osteonecrosis of the jaw (MRONJ) in osteoporosis patients: A systematic review. J. Craniomaxillofac. Surg. 45(9), 1493–1502 (2017).
Otto, S. et al. Infection as an important factor in medication-related osteonecrosis of the jaw (MRONJ). Medicina 57(5), 463 (2021).
Nicolatou-Galitis, O. et al. Medication-related osteonecrosis of the jaw: Definition and best practice for prevention, diagnosis, and treatment. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 127(2), 117–135 (2019).
Soutome, S. et al. Factors affecting development of medication-related osteonecrosis of the jaw in cancer patients receiving high-dose bisphosphonate or denosumab therapy: Is tooth extraction a risk factor?. PLoS ONE 13(7), e0201343 (2018).
Aguirre, J. I., Castillo, E. J. & Kimmel, D. B. Preclinical models of medication-related osteonecrosis of the jaw (MRONJ). Bone 153, 116184 (2021).
Varoni, E. M. et al. Conservative management of medication-related osteonecrosis of the jaws (MRONJ): A retrospective cohort study. Antibiotics 10(2), 195 (2021).
Ribeiro, N. R., Silva Lde, F., Santana, D. M. & Nogueira, R. L. Bisphosphonate-related osteonecrosis of the jaw after tooth extraction. J. Craniofac. Surg. 26(7), e606–e608 (2015).
Hewson, I., Syme, D. & Bruscino-Raiola, F. Radical surgical treatment of bisphosphonate related osteonecrosis of the jaw. Aust. Dent. J. 57(2), 227–230 (2012).
Ghazali, N., Collyer, J. C. & Tighe, J. V. Hemimandibulectomy and vascularized fibula flap in bisphosphonate-induced mandibular osteonecrosis with polycythaemia rubra vera. Int. J. Oral Maxillofac. Surg. 42(1), 120–123 (2013).
Marx, R. E., Sawatari, Y., Fortin, M. & Broumand, V. Bisphosphonate-induced exposed bone (osteonecrosis/osteopetrosis) of the jaws: Risk factors, recognition, prevention, and treatment. J. Oral Maxillofac. Surg. 63(11), 1567–1575 (2005).
Phal, P. M., Myall, R. W., Assael, L. A. & Weissman, J. L. Imaging findings of bisphosphonate-associated osteonecrosis of the jaws. AJNR Am. J. Neuroradiol. 28(6), 1139–1145 (2007).
Arce, K., Assael, L. A., Weissman, J. L. & Markiewicz, M. R. Imaging findings in bisphosphonate-related osteonecrosis of jaws. J. Oral Maxillofac. Surg. 67(5 Suppl), 75–84 (2009).
El-Rabbany, M. et al. Development and evaluation of the clinimetric properties of the Medication-Related Osteonecrosis of the Jaw Quality of Life Questionnaire (MRONJ-QoL). Int. J. Oral Maxillofac. Surg. 51(6), 768–775 (2022).
Otsuru, M. et al. A preliminary clinical study of segmental mandibulectomy on medication-related osteonecrosis of the jaw. J. Dent. Sci. 17(1), 444–450 (2022).
Florencio-Silva, R., Sasso, G. R., Sasso-Cerri, E., Simoes, M. J. & Cerri, P. S. Biology of bone tissue: Structure, function, and factors that influence bone cells. Biomed. Res. Int. 2015, 421746 (2015).
Ruggiero, S. L. et al. American Association of Oral and Maxillofacial Surgeons’ position paper on medication-related osteonecrosis of the jaws-2022 update. J. Oral Maxillofac. Surg. 80(5), 920–943 (2022).
Bedogni, A. et al. Long-term outcomes of surgical resection of the jaws in cancer patients with bisphosphonate-related osteonecrosis. Oral Oncol. 47(5), 420–424 (2011).
Beth-Tasdogan, N. H., Mayer, B., Hussein, H. & Zolk, O. Interventions for managing medication-related osteonecrosis of the jaw. Cochrane Database Syst. Rev. 10(10), 012432 (2017).
Coropciuc, R. G. et al. Medication-related osteonecrosis of the jaw in oncological patients with skeletal metastases: Conservative treatment is effective up to stage 2. Br. J. Oral Maxillofac. Surg. 55(8), 787–792 (2017).
Otto, S. et al. Autofluorescence-guided surgery for the treatment of medication-related osteonecrosis of the jaw (MRONJ): A retrospective single-center study. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 131(5), 519–526 (2021).
Wilde, F. et al. The role of surgical therapy in the management of intravenous bisphosphonates-related osteonecrosis of the jaw. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 111(2), 153–163 (2011).
Seth, R., Futran, N. D., Alam, D. S. & Knott, P. D. Outcomes of vascularized bone graft reconstruction of the mandible in bisphosphonate-related osteonecrosis of the jaws. Laryngoscope 120(11), 2165–2171 (2010).
Hanasono, M. M., Militsakh, O. N., Richmon, J. D., Rosenthal, E. L. & Wax, M. K. Mandibulectomy and free flap reconstruction for bisphosphonate-related osteonecrosis of the jaws. JAMA Otolaryngol. Head Neck Surg. 139(11), 1135–1142 (2013).
Stanton, D. C. & Balasanian, E. Outcome of surgical management of bisphosphonate-related osteonecrosis of the jaws: Review of 33 surgical cases. J. Oral Maxillofac. Surg. 67(5), 943–950 (2009).
Esen, A., Gurses, G. & Akkulah, S. Spontaneous bone regeneration in resected non-continuous mandible due to medication-related osteonecrosis of the jaw. J. Korean Assoc. Oral Maxillofac. Surg. 47(6), 465–470 (2021).
Kim, J. E., Yoo, S. & Choi, S. C. Several issues regarding the diagnostic imaging of medication-related osteonecrosis of the jaw. Imaging Sci. Dent. 50(4), 273–279 (2020).
Izzetti, R. et al. Panoramic radiography features of medication-related osteonecrosis of the jaws (MRONJ). Int. J. Dent. 2023, 5358849 (2023).
Ruggiero, S. L. Diagnosis and staging of medication-related osteonecrosis of the jaw. Oral Maxillofac. Surg. Clin. N. Am. 27(4), 479–487 (2015).
Treister, N. S., Friedland, B. & Woo, S. B. Use of cone-beam computerized tomography for evaluation of bisphosphonate-associated osteonecrosis of the jaws. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 109(5), 753–764 (2010).
Wongratwanich, P. et al. Do various imaging modalities provide potential early detection and diagnosis of medication-related osteonecrosis of the jaw? A review. Dentomaxillofac. Radiol. 50(6), 20200417 (2021).
Dindar, M. B., Acikgoz-Alparslan, E. & Tekbas-Atay, M. Radiographic evaluation of marginal bone height and density around overhanging dental restorations. Int. J. Periodont. Restor. Dent. 42(3), 401–408 (2022).
Roessler, P. P. et al. Relative radiographic bone density measurement in revision hip arthroplasty and its correlation with qualitative subjective assessment by experienced surgeons. Technol. Health Care 27(1), 79–88 (2019).
Ristow, O. et al. Comparison of auto-fluorescence and tetracycline fluorescence for guided bone surgery of medication-related osteonecrosis of the jaw: A randomized controlled feasibility study. Int. J. Oral Maxillofac. Surg. 46(2), 157–166 (2017).
Otto, S. et al. Fluorescence-guided surgery for the treatment of medication-related osteonecrosis of the jaw: A prospective cohort study. J. Craniomaxillofac. Surg. 44(8), 1073–1080 (2016).
de Vernejoul, M. C. Sclerosing bone disorders. Best Pract. Res. Clin. Rheumatol. 22(1), 71–83 (2008).
Tyagi, R. Spinal infections in children: A review. J. Orthop. 13(4), 254–258 (2016).
Hauge, E. M., Qvesel, D., Eriksen, E. F., Mosekilde, L. & Melsen, F. Cancellous bone remodeling occurs in specialized compartments lined by cells expressing osteoblastic markers. J. Bone Miner. Res. 16(9), 1575–1582 (2001).
Azuma, Y. et al. Alendronate distributed on bone surfaces inhibits osteoclastic bone resorption in vitro and in experimental hypercalcemia models. Bone 16(2), 235–245 (1995).
Cremers, S., Drake, M. T., Ebetino, F. H., Bilezikian, J. P. & Russell, R. G. G. Pharmacology of bisphosphonates. Br. J. Clin. Pharmacol. 85(6), 1052–1062 (2019).
Ashrafi, M., Ghalichi, F., Mirzakouchaki, B. & Doblare, M. On the effect of antiresorptive drugs on the bone remodeling of the mandible after dental implantation: A mathematical model. Sci. Rep. 11(1), 2792 (2021).
Nemecek, E. et al. Analysis and quantification of bone healing after open wedge high tibial osteotomy. Wien Klin Wochenschr. 131(23–24), 587–598 (2019).
Favia, G., Tempesta, A., Limongelli, L., Crincoli, V. & Maiorano, E. Medication-related osteonecrosis of the jaw: Surgical or non-surgical treatment?. Oral Dis. 24(1–2), 238–242 (2018).
Goker, F. et al. Zygomatic implant insertion in MRONJ: A case report with a follow-up of 3 years. J. Clin. Med. 12(9), 3300 (2023).
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Contributions
Conceptualization, S.O., KT.O. I.D, methodology S.O., KT.O, I.D; resources, I.D.; data curation, KT.O., I.D.,..; writing—original draft preparation, I.D.,KT.O.writing—review and editing, R.F., Y.M. S.O., I.D.; visualization, I.D., KT.O.; supervision, S.O.; G.K; project administration, S.O.; All authors have read and agreed to the published version of the manuscript
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Obermeier, K.T., Dewenter, I., Malenova, Y. et al. Sclerotic bone: a sign of bone reaction in patients with medication related osteonecrosis of the jaw. Sci Rep 14, 7914 (2024). https://doi.org/10.1038/s41598-024-57635-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-57635-5
Keywords
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.